| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Neurofibromatosis Type 1
Related Subjects: |Neurofibromatosis Type 1 |Neurofibromatosis Type 2 |Tuberous sclerosis |Café-au-lait spots |McCune Albright syndrome
📊 About
- Prevalence: NF1 is around 10× more common than NF2. Estimated prevalence ≈ 1 in 3,000. 🧬
- Exam Focus: NF1 features are far more likely to appear in exams than NF2 due to its distinctive skin, eye, and tumour manifestations. 🎓
🧬 Aetiology
- Inheritance: Autosomal dominant (50% chance of transmission), but ~50% arise from de novo mutations. 👪
- Gene: Mutation in NF1 gene on chromosome 17, encoding neurofibromin, a tumour suppressor protein regulating the Ras/MAPK pathway.
- Pathophysiology: Loss of neurofibromin → ↑ Ras activity → uncontrolled cell growth → neurofibroma formation. 🔬
🩺 Clinical Features
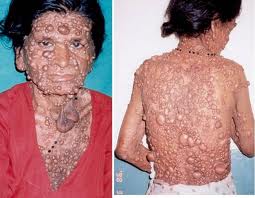
- Cutaneous Neurofibromas: Multiple, soft, rubbery nodules under the skin. May cause cosmetic concerns or compress structures.
- Plexiform Neurofibromas: Larger, deeper tumours, can cause disfigurement or functional loss; risk of malignant peripheral nerve sheath tumour (~10%). ⚠️
- Axillary/Inguinal Freckling: “Crowe’s sign” – pathognomonic for NF1. 🌟
- Café-au-lait Spots: ≥6 macules (>5 mm in children, >15 mm in adults). Best seen with Wood’s lamp on pale skin. ☕
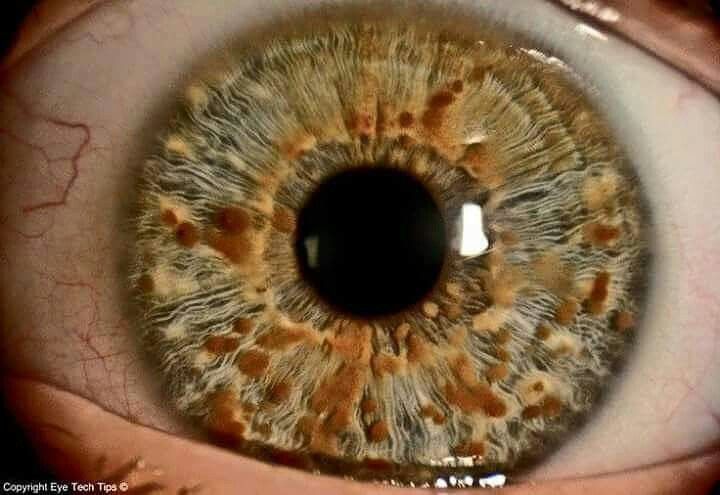
- Lisch Nodules: Iris hamartomas, visible on slit-lamp exam, usually asymptomatic but highly diagnostic. 👁️
- Optic Gliomas: Can impair vision, often detected in childhood. 👓
- Bony Abnormalities: Tibial bowing, scoliosis, pseudoarthrosis, macrocephaly, short stature. 🦴
- Hypertension: May be due to renal artery stenosis or phaeochromocytoma. 🩸
Lisch Nodules:
🔗 Associated Conditions
- Renal Artery Stenosis: Secondary hypertension, common in children with NF1.
- Phaeochromocytoma: Catecholamine-secreting tumour → paroxysmal hypertension, palpitations, sweats. ⚡
- CNS Tumours: Optic glioma (classic), astrocytoma, glioblastoma, ependymoma, meningioma.
- Pulmonary Fibrosis and Cardiomyopathy – rare but reported complications.
- Rare links: Medullary thyroid carcinoma in some NF1 patients, overlap with MEN syndromes is debated. 🦋
🛠️ Management
- Monitoring: Annual BP, ophthalmology review (children), dermatology/neurology surveillance for tumour burden.
- Genetic Counselling: Key for affected families (autosomal dominant inheritance, variable penetrance). 👨👩👧👦
- Multidisciplinary Care: Dermatology, neurology, ophthalmology, genetics, orthopaedics.
- Surgery: Reserved for symptomatic or function-threatening neurofibromas; plexiform lesions can be challenging to excise.
- New Therapies: MEK inhibitors (e.g. selumetinib) show promise in shrinking plexiform neurofibromas. 💊
📌 Key Exam Pearls
✅ Café-au-lait spots + axillary freckling + neurofibromas = think NF1.
✅ Always check BP in NF1 patients – hypertension may be due to renal artery stenosis or phaeochromocytoma.
✅ Lisch nodules are highly specific for NF1, best seen with slit-lamp.
✅ NF1 ↑ risk of malignant peripheral nerve sheath tumours → any rapidly enlarging/painful neurofibroma = red flag. 🚨
📖 References
Cases - Neurofibromatosis Type 1 (NF1)
- Case 1 - Child with Café-au-Lait Spots: A 7-year-old boy is referred for multiple light-brown skin patches. Exam: ≥6 café-au-lait spots >5 mm, axillary freckling, and a soft, pedunculated nodule on the arm (cutaneous neurofibroma). Ophthalmology exam reveals Lisch nodules on the iris. Diagnosis: NF1 based on NIH diagnostic criteria. Management: Multidisciplinary follow-up (neurology, dermatology, ophthalmology); annual BP monitoring (risk of renal artery stenosis); genetic counselling.
- Case 2 - Adolescent with Plexiform Neurofibroma: A 14-year-old girl with known NF1 presents with a large, soft, “bag-of-worms” mass along her neck that has been enlarging. Exam: scoliosis and multiple cutaneous neurofibromas. MRI: plexiform neurofibroma extending along the brachial plexus. Diagnosis: NF1 with plexiform neurofibroma. Management: Surgical debulking if symptomatic or compressive; regular imaging for malignant transformation risk (MPNST); psychosocial support.
Teaching Commentary 🧬
NF1 is an autosomal dominant neurocutaneous disorder (chromosome 17, neurofibromin gene). Diagnostic features (need ≥2): - ≥6 café-au-lait spots, - ≥2 neurofibromas or 1 plexiform neurofibroma, - Axillary/inguinal freckling, - Optic glioma, - ≥2 Lisch nodules (iris hamartomas), - Distinctive bone lesion (sphenoid dysplasia, tibial bowing), - First-degree relative with NF1. Complications: learning disability, hypertension (renal artery stenosis, phaeochromocytoma), scoliosis, optic gliomas, malignant peripheral nerve sheath tumours. Management: lifelong surveillance with multidisciplinary input.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
