| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Sodium Physiology
Related Subjects: |Water Physiology |Sodium Physiology |Potassium Physiology |Aldosterone Physiology |Atrial Natriuretic Peptide (ANP) |Brain Natriuretic Peptide (BNP)
🧂 Sodium (Na⁺) is the dominant extracellular cation and the single most important determinant of extracellular fluid (ECF) volume. A key “exam + clinical” principle is: total body sodium controls volume, while water balance controls sodium concentration. So most hyponatraemia is fundamentally a water excess (ADH problem), whereas most hypernatraemia is a water deficit.
📍 Distribution and why it matters
- Where sodium lives
- ECF (plasma + interstitial fluid): ~135–145 mmol/L (normal lab reference range).
- ICF: ~10–15 mmol/L.
- This steep gradient is essential for membrane potentials, nerve conduction, and coupled transport.
- How the gradient is maintained: Na⁺/K⁺-ATPase
- Pumps 3 Na⁺ out and 2 K⁺ in per ATP → maintains low intracellular Na⁺ and contributes to a negative resting membrane potential.
- Creates the “stored energy” used by secondary active transport (e.g. glucose uptake in the gut, renal reabsorption).
🧠 Sodium, osmolality, and brain adaptation (high-yield)
- Tonicity vs osmolality
- Osmolality = total dissolved particles per kg water (includes urea).
- Tonicity (effective osmolality) = particles that do not freely cross cell membranes and therefore shift water (mainly Na⁺ and glucose).
- That’s why hyperglycaemia can cause “dilutional” hyponatraemia (water shifts out of cells).
- Why rapid Na correction is dangerous
- In chronic hyponatraemia, brain cells adapt by expelling osmoles to reduce cerebral oedema.
- If you raise serum Na⁺ too fast, water rapidly leaves brain cells → risk of osmotic demyelination syndrome (ODS).
- In acute hyponatraemia, there’s less time to adapt → cerebral oedema and seizures are the main threat.
⚙️ Key physiological functions of sodium
- ECF volume and blood pressure
- Sodium content of ECF drives water retention → determines circulating volume and therefore perfusion pressure.
- Chronic sodium excess contributes to hypertension via volume expansion and vascular remodelling.
- Electrical excitability (nerve and muscle)
- Fast Na⁺ influx through voltage-gated channels generates the upstroke of action potentials in neurons and skeletal muscle.
- In cardiac tissue, Na⁺ is crucial for phase 0 depolarisation (esp. atrial/ventricular myocytes and Purkinje fibres).
- Secondary active transport
- Gut: SGLT1 co-transports Na⁺ + glucose (basis of oral rehydration therapy).
- Kidney: Na⁺ gradients power multiple solute transporters along the nephron.
- Acid–base physiology (advanced but useful)
- Na⁺ is the major “strong cation”; changes in accompanying anions (especially chloride) influence acid–base balance.
- Large volumes of 0.9% saline (high chloride) can contribute to hyperchloraemic metabolic acidosis, hence interest in balanced crystalloids in some settings.
🧪 Renal handling of sodium (where it’s reabsorbed + key transporters)
- Filtered load
- Na⁺ is freely filtered at the glomerulus; the kidney then “chooses” how much to reclaim.
- Small changes in fractional excretion make big differences in volume status.
- Proximal tubule (~65% reabsorbed)
- Major transporter: NHE3 (Na⁺/H⁺ exchanger) + Na⁺ co-transport with glucose, amino acids, phosphate.
- “Iso-osmotic reabsorption”: water follows solute → preserves tonicity.
- Thick ascending limb (~25%)
- Major transporter: NKCC2 (Na⁺-K⁺-2Cl⁻ cotransporter).
- Water-impermeable → helps create the medullary gradient (countercurrent multiplication).
- Loop diuretics act here.
- Distal convoluted tubule (~5%)
- Major transporter: NCC (Na⁺-Cl⁻ cotransporter).
- Thiazides act here and are a classic cause of hyponatraemia.
- Collecting duct (~2–3% but “fine-tuning”)
- Major channel: ENaC (epithelial Na⁺ channel), stimulated by aldosterone.
- Coupled to K⁺ and H⁺ secretion → explains hyperkalaemia and acidosis risk in hypoaldosteronism.
- Amiloride blocks ENaC; spironolactone/eplerenone block mineralocorticoid receptor.
🧠 Hormonal control: sodium balance vs sodium concentration
- RAAS (renin–angiotensin–aldosterone system)
- Triggered by low effective arterial blood volume (EABV): renal hypoperfusion, low NaCl delivery to macula densa, sympathetic activation.
- Angiotensin II: vasoconstriction + increases proximal Na⁺ reabsorption + stimulates aldosterone and thirst.
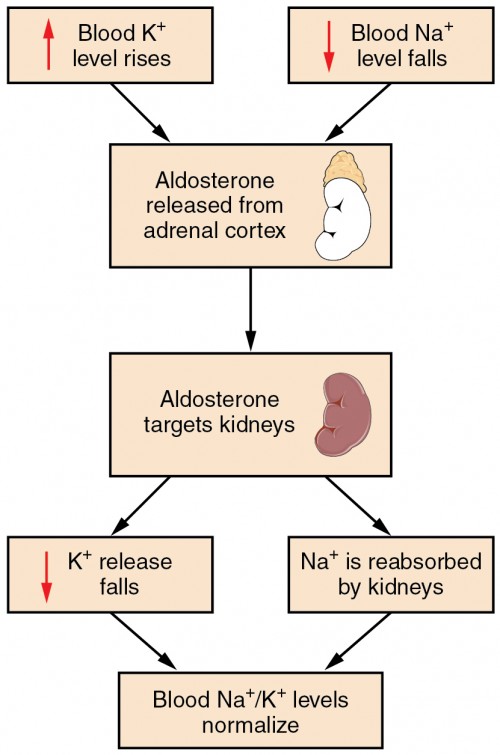
- Aldosterone: increases ENaC and Na⁺/K⁺-ATPase activity → Na⁺ retention (with K⁺/H⁺ loss).
- Natriuretic peptides (ANP/BNP)
- Released with atrial/ventricular stretch → promote natriuresis and vasodilation, suppress renin/aldosterone.
- ADH (vasopressin): mainly water, not sodium
- Increases water reabsorption in collecting duct via aquaporin-2 insertion.
- Therefore ADH changes serum Na⁺ concentration by changing water balance.
- Thirst
- Osmoreceptors in hypothalamus respond to small rises in tonicity → drives water intake.
- In frail older adults, impaired thirst/access to water is a common hypernatraemia mechanism.
🏥 Clinical approach to abnormal sodium (the framework that wins exams)
1) Hyponatraemia (Na⁺ <135)
- Step 1: check osmolality
- Hypotonic hyponatraemia (most common): true water excess.
- Isotonic: pseudohyponatraemia (very high lipids/protein; lab artifact with some methods).
- Hypertonic: translocational hyponatraemia (e.g., hyperglycaemia, mannitol).
- Step 2: assess volume status clinically
- Hypovolaemic: GI losses, diuretics, adrenal insufficiency, renal salt wasting.
- Euvolaemic: SIADH, hypothyroidism, glucocorticoid deficiency, primary polydipsia.
- Hypervolaemic: heart failure, cirrhosis, nephrotic syndrome (low EABV → high ADH despite oedema).
- Step 3: use urine studies to “read ADH and aldosterone”
- Urine osmolality:
- <100 mOsm/kg suggests suppressed ADH (e.g., primary polydipsia, low solute intake).
- >100 mOsm/kg suggests ADH is active (common in SIADH, hypovolaemia, heart failure).
- Urine sodium (often with a threshold around 30 mmol/L):
- Low urine Na⁺ suggests kidneys avidly retaining sodium (low EABV states).
- Higher urine Na⁺ suggests renal sodium loss or SIADH pattern.
- Urine osmolality:
- Symptoms (brain swelling = the danger)
- Mild: nausea, headache, gait instability.
- Severe: confusion, seizures, coma (treat as emergency).
Emergency hyponatraemia (what you actually do)
- If seizures or severe neurological symptoms: give hypertonic saline in controlled boluses with frequent Na⁺ checks.
- Targets are modest early rises (e.g., ~4–6 mmol/L) to relieve cerebral oedema, then slow correction to avoid ODS.
- Do not “normalise” sodium quickly - you are treating brain oedema first, not the lab number.
2) Hypernatraemia (Na⁺ >145)
- Core concept: almost always water deficit relative to sodium.
- Common causes
- Reduced intake: impaired thirst, reduced access to water, delirium.
- Excess losses: diarrhoea, sweating, burns, osmotic diuresis (e.g., hyperglycaemia).
- Diabetes insipidus: inadequate ADH (central) or renal resistance (nephrogenic).
- Treatment principle
- If shocked/hypovolaemic: resuscitate first (isotonic fluid), then replace free water.
- Correct gradually if chronicity uncertain to reduce cerebral oedema risk.
💉 Sodium content of common IV fluids (practical prescribing)
- 0.9% sodium chloride: ~154 mmol/L sodium (and 154 mmol/L chloride).
- 3% sodium chloride: very concentrated hypertonic saline (~513 mmol/L sodium).
- In hyponatraemia, giving isotonic saline may raise Na⁺ very little directly, but can stop hypovolaemia-driven ADH → brisk water diuresis and a faster-than-expected Na rise (watch for overcorrection).
📝 Summary
Sodium is the main extracellular cation and the key determinant of extracellular volume and perfusion. The kidneys fine-tune sodium via segment-specific transporters (PT → TAL → DCT → collecting duct) under RAAS and natriuretic peptide control, while ADH and thirst primarily regulate water and therefore sodium concentration. Clinically, think in frameworks: hyponatraemia = check tonicity → assess volume → urine osm/Na; hypernatraemia = water deficit. In emergencies, treat the brain first (seizures/cerebral oedema) and correct sodium slowly enough to avoid iatrogenic neurological injury.
🔗 Useful UK-friendly links: | NICE CKS: Hyponatraemia | NICE CG174: IV fluids in adults | Society for Endocrinology (2022): emergency hyponatraemia
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
