Related Subjects:
|Fever in a traveller
|Bell's (Facial nerve) Palsy
🦠 Lyme disease is a multisystem inflammatory disorder caused by the spirochaete Borrelia burgdorferi.
🐞 Transmitted by Ixodid (deer) ticks, it is common in the USA, Asia, and Europe.
💡 Early recognition and treatment are crucial to prevent long-term complications.
🔬 Infectious Agents
- Borrelia burgdorferi sensu stricto – USA.
- Borrelia afzelii – Europe (skin manifestations such as acrodermatitis).
- Borrelia garinii – Europe (neuroborreliosis).
- All transmitted by Ixodes ticks (I. scapularis, I. ricinus).
📅 Seasonality
- Spring and summer: higher tick activity.
- Linked to woodland, grassy and rural environments.
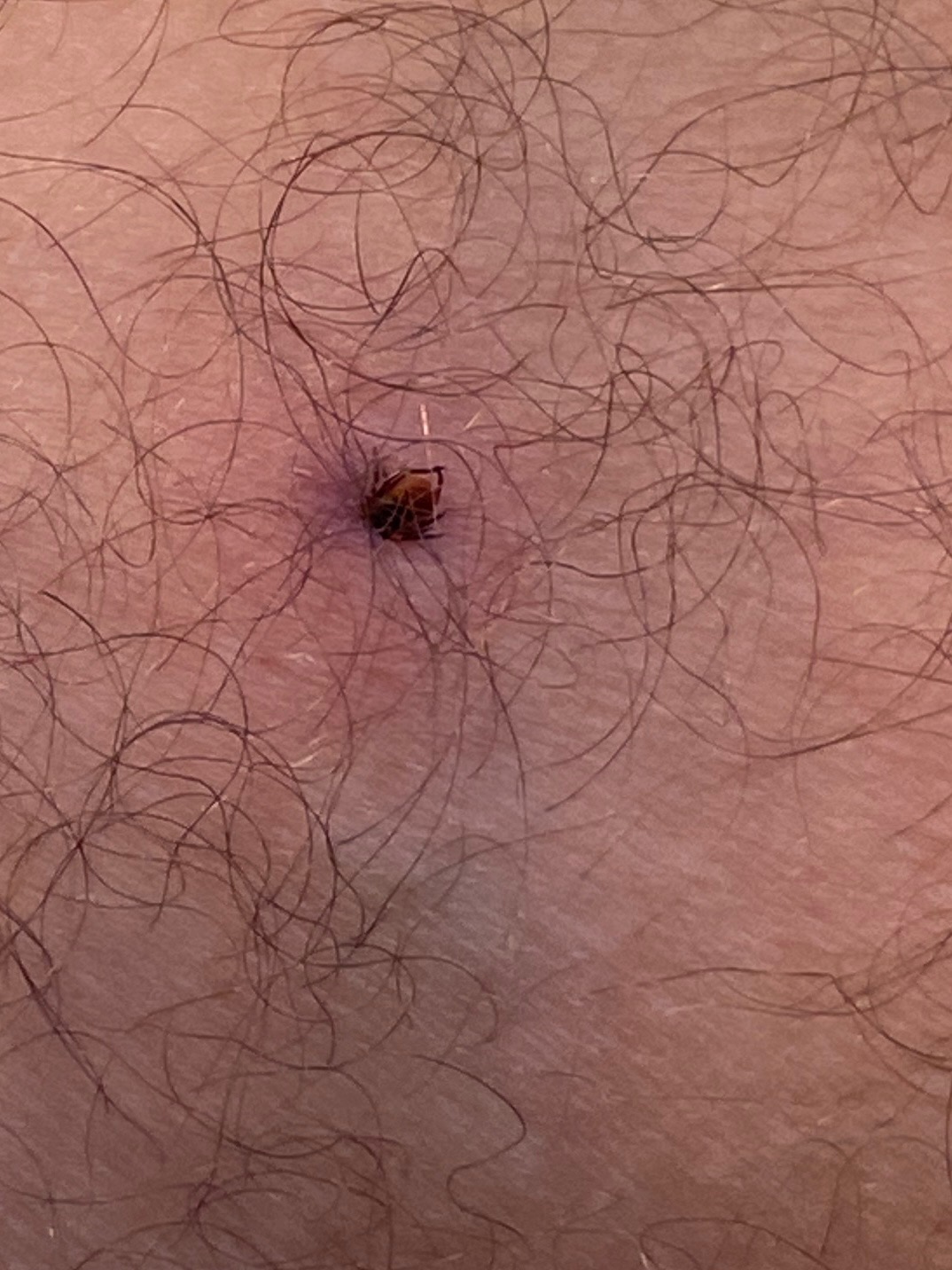 🕷️ Ixodid tick (vector for Lyme disease).
🕷️ Ixodid tick (vector for Lyme disease).
📖 Clinical Stages
| 🩺 Stages of Lyme Disease |
|---|
| Stage 1 (Early Localized) |
~1 month after bite |
🟢 Erythema migrans (bull’s-eye rash), fever, malaise, headache, fatigue, lymphadenopathy. |
| Stage 2 (Early Disseminated) |
Weeks–months |
🌍 Multiple skin lesions, migratory arthralgia, myalgia.
❤️ Carditis (AV block).
🧠 Neurology: meningitis, facial palsy, radiculopathy. |
| Stage 3 (Late Lyme) |
Months–years |
🦵 Chronic arthritis (large joints).
🧠 Encephalopathy, peripheral neuropathy.
🌐 Acrodermatitis chronica atrophicans (Europe). |
🧠 Bannwarth’s Syndrome
- Painful radiculitis + lymphocytic meningitis.
- Often with multiple cranial nerve palsies, radiculopathy, and peripheral motor deficits.
🧪 Investigations
- Serology: ELISA → confirmed with Western blot. May be negative early but nearly always positive late.
- IgM = early infection; rising titres suggest recent disease (beware false positives).
- PCR: CSF, joint aspirate, skin biopsy useful in neuroborreliosis.
- CSF: lymphocytic pleocytosis, ↑ protein.
- MRI: white matter changes may mimic demyelination.
🛡️ Prevention
- Prompt tick removal (<24h) reduces transmission risk.
- Protective clothing + tick repellents in endemic zones.
- Check skin folds, scalp, behind knees after outdoor exposure.
- No widely available human vaccine (some under development).
- PEP: Doxycycline 200 mg single dose can reduce risk if given within 72h of high-risk bite.
💊 Management
- Early/localized disease: Doxycycline 100 mg BD × 14 days (Amoxicillin if pregnant or child).
- Alternative agents: Amoxicillin, Cefuroxime, Azithromycin.
- Late/disseminated disease: Longer courses (14–30 days).
Severe neuro/cardiac disease → IV Ceftriaxone or Benzylpenicillin.
- Jarisch–Herxheimer reaction: Temporary worsening after starting antibiotics due to spirochaete die-off.
- Carditis: Usually resolves with antibiotics; pacing rarely required.
- Bell’s palsy (Lyme-associated): Doxycycline 100 mg BD × 2–4 weeks (if no contraindication).
📌 Key Points & Considerations
- Long-term sequelae possible if untreated: arthritis, neuropathy, cognitive impairment.
- Complicated disease → discuss with infectious disease specialists.
- Public health: tick control, awareness campaigns, and early treatment reduce morbidity.
📚 References
- CDC – Lyme Disease
- UpToDate: Lyme Disease (clinical guidance).
- NICE: Lyme Disease Management Guidelines.
💡 Exam Pearl: The triad of erythema migrans, facial palsy, and AV block is highly suggestive of Lyme disease.
 🕷️ Ixodid tick (vector for Lyme disease).
🕷️ Ixodid tick (vector for Lyme disease).
