| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Artery of Percheron stroke
Related Subjects: |Acute Stroke Assessment (ROSIER&NIHSS) |Atrial Fibrillation |Atrial Myxoma |Causes of Stroke |Ischaemic Stroke |Cancer and Stroke |Cardioembolic stroke |CT Basics for Stroke |Endocarditis and Stroke |Haemorrhagic Stroke |Stroke Thrombolysis |Hyperacute Stroke Care
🧠 Artery of Percheron (AOP) is a rare vascular variant where a single perforating artery supplies both paramedian thalami (± midbrain). This is unusual because most cerebral arteries respect the midline.
📖 About
- First described in 1973 by French neurologist Gérard Percheron.
- Supplies bilateral paramedian thalami (≈30% of cases).
- Important cause of acute coma with otherwise normal early CT.
⚙️ Pathophysiology
- Occlusion → bilateral medial thalamic infarcts ± midbrain involvement.
- 🛌 Classic triad: altered mental status, vertical gaze palsy, memory disturbance.
- Coma occurs due to involvement of the thalamic–reticular activating system.
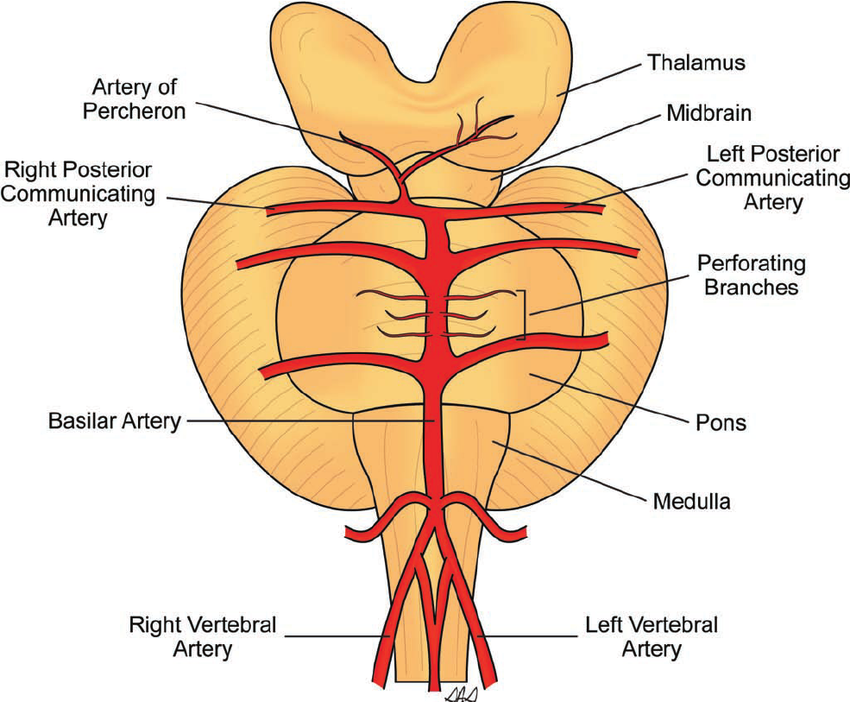
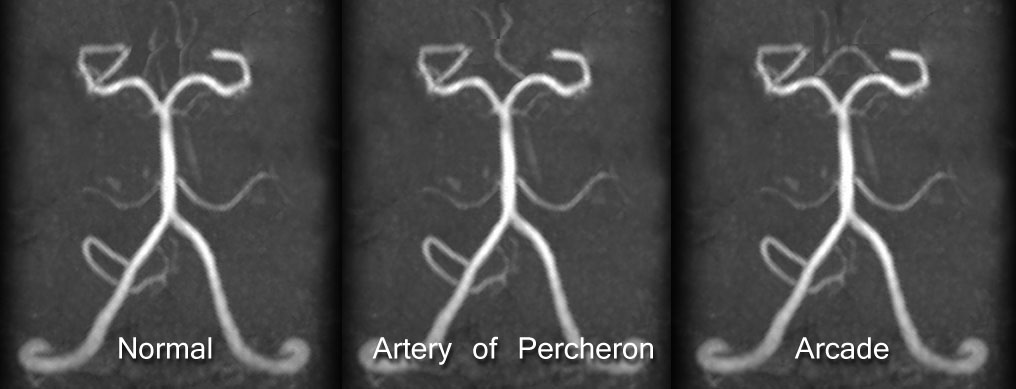
🧩 Anatomy
- Usually, each medial thalamus has its own arterial supply.
- AOP arises from a single P1/P2 segment of the PCA → bifurcates to supply both thalami.
- Common error: It comes from the PCA, not the posterior communicating artery.
📊 Epidemiology
- Rare: 0.1–2% of all ischaemic strokes.
- A typical UK stroke centre (~1,000 cases/yr) may see only 1–2 cases annually.
🧬 Aetiology
- Cardioembolic (AF, LV thrombus) or artery-to-artery embolism.
- Less common: vertebral artery dissection.
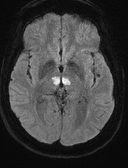
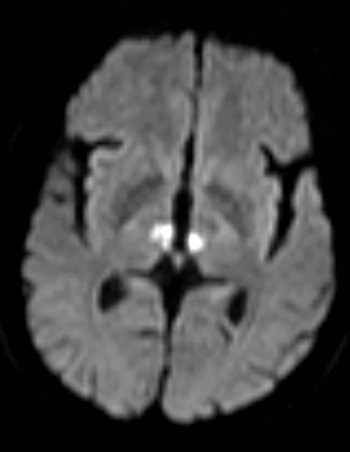
🧲 MRI Appearance
- 🎯 “Butterfly sign”: bilateral paramedian thalamic infarcts.
- 🪶 “V sign” in interpeduncular fossa (seen in ~67%).
🩺 Clinical Presentation
- Acute coma 🛌 or profound somnolence.
- Vertical gaze palsy 👀 and pupillary abnormalities (± pinpoint pupils).
- ⚡ Memory/cognitive deficits often persist.
- If midbrain involved → hemiplegia or CN III palsy.
🔑 Mnemonic: AOP → “3 C’s”: Coma, Cognition, Cranial nerve palsy.
🔍 Differentials (Coma with normal CT)
- Meningoencephalitis 🦠
- Opiate/sedative overdose 💊
- Pontine stroke 🧠
- Post-ictal state ⚡
- Hypoglycaemia 🍬
🧪 Investigations
- Bloods: FBC, U&E, CRP, ESR, cholesterol.
- Cardiac: ECG + Holter, echo (look for AF or thrombus).
- CT: often normal early; later → thalamic hypodensity.
- MRI DWI: diagnostic (butterfly/V-sign).
- CTA/MRA: may show vertebral dissection.
- LP: usually normal, rules out infection.
💊 Management
- Immediate ABC support.
- Thrombolysis/thrombectomy if within window (rarely achieved due to delayed Dx).
- If diagnosis uncertain → treat empirically for infection until confirmed.
- Standard secondary prevention: antiplatelets, BP control, statins.
- Neurorehab + neuropsychology for cognitive recovery.
📌 Exam Pearl: “Coma + normal CT” → always think of Artery of Percheron infarct as a differential.
📚 References
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
