| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Mycosis Fungoides (Sezary Syndrome)
Related Subjects: |Nikolsky's sign |Koebner phenomenon |Erythema Multiforme |Pyoderma gangrenosum |Erythema Nodosum |Dermatitis Herpetiformis |Lichen Planus |Acanthosis Nigricans |Acne Rosacea |Acne Vulgaris |Alopecia |Vitiligo |Urticaria |Basal Cell Carcinoma |Malignant Melanoma |Squamous Cell Carcinoma |Mycosis Fungoides (Sezary Syndrome) |Xeroderma pigmentosum |Bullous Pemphigoid |Pemphigus Vulgaris |Seborrheic Dermatitis |Pityriasis/Tinea versicolor infections |Pityriasis rosea |Scabies |Dermatomyositis |Toxic Epidermal Necrolysis |Stevens-Johnson Syndrome |Atopic Eczema/Atopic Dermatitis |Psoriasis
📖 About
- Mycosis fungoides is a rare cutaneous T-cell lymphoma (CTCL), and the most common subtype.
- It manifests primarily on the skin with multiple erythematous, itchy lesions, often mistaken for eczema or psoriasis → delayed diagnosis.
- Usually progresses slowly 🐢 and may not shorten life expectancy in early/limited disease.
- When malignant T-cells circulate in blood with systemic involvement → classified as Sézary Syndrome (aggressive form 🔴).
🧬 Aetiology
- A neoplastic proliferation of CD4+ T-helper lymphocytes with skin-homing properties.
- Typically affects adults aged 40–60 years, with a slight male predominance.
- Exact cause unknown, but chronic antigenic stimulation, genetic factors, and immune dysregulation are implicated.
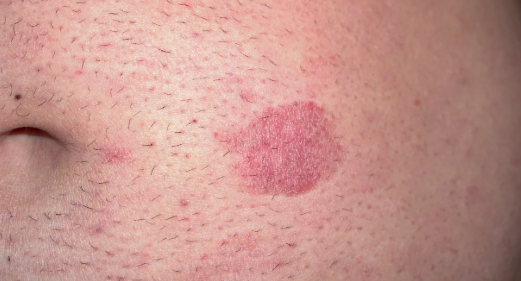
👀 Clinical Features
- Chronic, itchy, erythematous patches → slowly progress over years.
- Early lesions: scaly, irregular patches on sun-protected areas (buttocks, thighs, trunk).
- Can mimic psoriasis/eczema, delaying diagnosis ⏳.
- Later: plaques, nodules, ulcerated tumours (may discharge).
- Diffuse redness of skin → erythroderma.
- Advanced: exfoliative dermatitis, generalised lymphadenopathy, and ~10% risk of visceral organ involvement (liver, spleen, lung).
- Sézary syndrome: erythroderma + lymphadenopathy + malignant T-cells in blood.
🔬 Investigations
- Skin biopsy (diagnostic): infiltrate of atypical CD4+ T-cells with cerebriform (Sézary-Lutzner) nuclei; epidermotropism with Pautrier’s microabscesses.
- Blood tests: usually normal in early disease; check for systemic spread.
- Flow cytometry if Sézary syndrome suspected (circulating malignant T-cells).
- Staging workup: CT/PET to assess nodal/visceral involvement.
📊 Staging (simplified)
- Patch stage – erythematous scaly patches (years to decades).
- Plaque stage – thickened, raised lesions.
- Tumour stage – nodules, ulcerating masses.
- Systemic stage – blood, lymph node, organ involvement (Sézary syndrome).
💊 Management
- No absolute cure, but remission and long-term control possible.
- Early disease often treated with skin-directed therapies:
- Regular emollients + topical corticosteroids for itch/inflammation.
- Phototherapy (NB-UVB or PUVA) for widespread skin involvement.
- Local radiotherapy (electron beam, low-voltage X-rays) for thick plaques/tumours.
- For refractory or advanced disease → systemic therapies:
- Methotrexate – immunosuppressive, first-line systemic agent.
- Oral retinoids – normalise keratinocyte growth.
- Interferon-alpha – immune modulation.
- Extracorporeal photopheresis – esp. in Sézary syndrome.
- Chemotherapy – reserved for aggressive/refractory disease (e.g., CHOP regimen).
- Care is MDT-led 👥 → dermatology, haematology, oncology input.
✅ Key Exam Pearls
- Most common cutaneous T-cell lymphoma.
- Biopsy shows cerebriform CD4+ cells + epidermotropism.
- Sézary syndrome = triad (erythroderma + lymphadenopathy + circulating malignant cells).
- Treatment is stage-based → skin therapies early, systemic if advanced.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
