| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Acne Rosacea ✅
Related Subjects: | Nikolsky's sign | Koebner phenomenon | Erythema Multiforme | Pyoderma gangrenosum | Erythema Nodosum | Dermatitis Herpetiformis | Lichen Planus | Acanthosis Nigricans | Acne Rosacea | Acne Vulgaris | Alopecia | Vitiligo | Urticaria | Basal Cell Carcinoma | Malignant Melanoma | Squamous Cell Carcinoma | Mycosis Fungoides (Sezary Syndrome) | Xeroderma pigmentosum | Bullous Pemphigoid | Pemphigus Vulgaris | Seborrheic Dermatitis | Pityriasis/Tinea versicolor infections | Pityriasis rosea | Scabies | Dermatomyositis | Toxic Epidermal Necrolysis | Stevens-Johnson Syndrome | Atopic Eczema/Atopic Dermatitis | Psoriasis
🌹 Acne Rosacea is a chronic inflammatory disorder of the central face. It is non-infectious and often worsened by triggers such as topical steroids or systemic drugs (e.g., amiodarone, vasodilators). 💡 Early recognition and trigger avoidance are key to preventing progression and complications.
📖 Overview
- 🔥 Characterised by recurrent flushing, persistent erythema, papules, pustules, telangiectasia, and phymatous changes.
- 🧬 Inflammatory changes are perifollicular and perivascular; no microbial pathogen is primary.
- ⚖️ Often misdiagnosed as acne vulgaris – key distinction: no comedones and later age of onset.
🧪 Aetiology & Pathophysiology
- 🕷 Demodex folliculorum mites: may trigger innate immune response and inflammation.
- 💓 Vascular dysregulation: abnormal vasomotor response → flushing, persistent erythema.
- 🧠 Neurovascular factors: TRPV1 receptor hyperreactivity contributes to burning/stinging.
- 🌍 Environmental factors: UV light, temperature extremes, wind, humidity.
- 🧬 Genetic predisposition: family clustering suggests heritable susceptibility.
- 💊 Exacerbating medications: corticosteroids, vasodilators, niacin, amiodarone, topical irritants.
- 🔥 Chronic inflammation: cytokine-mediated perivascular and perifollicular infiltrates → papules/pustules, phymatous changes in sebaceous glands.
📊 Epidemiology
- 👩 Typically adults 40–60 years; rare in children.
- 👨 Males: more severe phymatous changes; females: more frequent erythematotelangiectatic subtype.
- 🚩 Triggers: alcohol, spicy foods, hot beverages, sunlight, heat, stress, exercise, topical steroids.
🩺 Clinical Subtypes (NICE / ROSACEA Grading)
- 🌡 Erythematotelangiectatic: flushing, persistent erythema, visible telangiectasia.
- 🔴 Papulopustular: central facial papules/pustules, no comedones.
- 👃 Phymatous: sebaceous gland hypertrophy → rhinophyma, mostly in men.
- 👁 Ocular rosacea: blepharitis, conjunctivitis, keratitis, corneal involvement.
🚩 Triggers to Avoid
- 🍷 Alcohol, hot drinks
- 🌶 Spicy foods
- ☀️ Sunlight (SPF ≥30 advised), 💨 wind, ❄️ cold, high temperature
- 🏃 Exercise or heat exposure
- 😰 Stress
- 💊 Topical steroids or irritating cosmetics
🔍 Diagnosis & Examination
- ✅ Clinical diagnosis: central facial erythema, papules/pustules, telangiectasia, phymatous changes, ocular involvement.
- 🚫 Key differentiator from acne vulgaris: absence of comedones.
- 👁 Examine for ocular involvement: lid margin inflammation, conjunctival injection, corneal changes.
- 🧾 Consider dermoscopy for telangiectasia and inflammatory changes.
- 🧪 Investigations only if atypical presentation: exclude lupus, seborrhoeic dermatitis, or drug-induced eruptions.
💊 Management (NICE-Aligned)
- General care & lifestyle:
- SPF ≥30 daily, gentle cleansers, avoid irritants.
- Identify and avoid triggers (diet, alcohol, heat, stress, topical steroids).
- Topical therapy:
- Metronidazole 0.75–1% gel/cream OD–BD
- Azelaic acid 15–20% gel/cream BD
- Brimonidine 0.33% gel: vasoconstrictor for persistent erythema (short-term effect)
- Oral therapy:
- Doxycycline 40–100 mg/day (anti-inflammatory dose) – typically 4–12 weeks
- Lymecycline as alternative
- Oxytetracycline or minocycline less preferred (pigmentation, side effects)
- Refractory/severe cases: low-dose isotretinoin or specialist dermatology input
- Procedures: Pulsed dye laser or IPL for telangiectasia/erythema; surgical/laser rhinophyma reduction
- Ocular rosacea: eyelid hygiene, lubricating drops, topical/oral antibiotics if keratitis or blepharitis; urgent ophthalmology referral if corneal involvement
🖼 Images
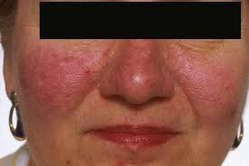
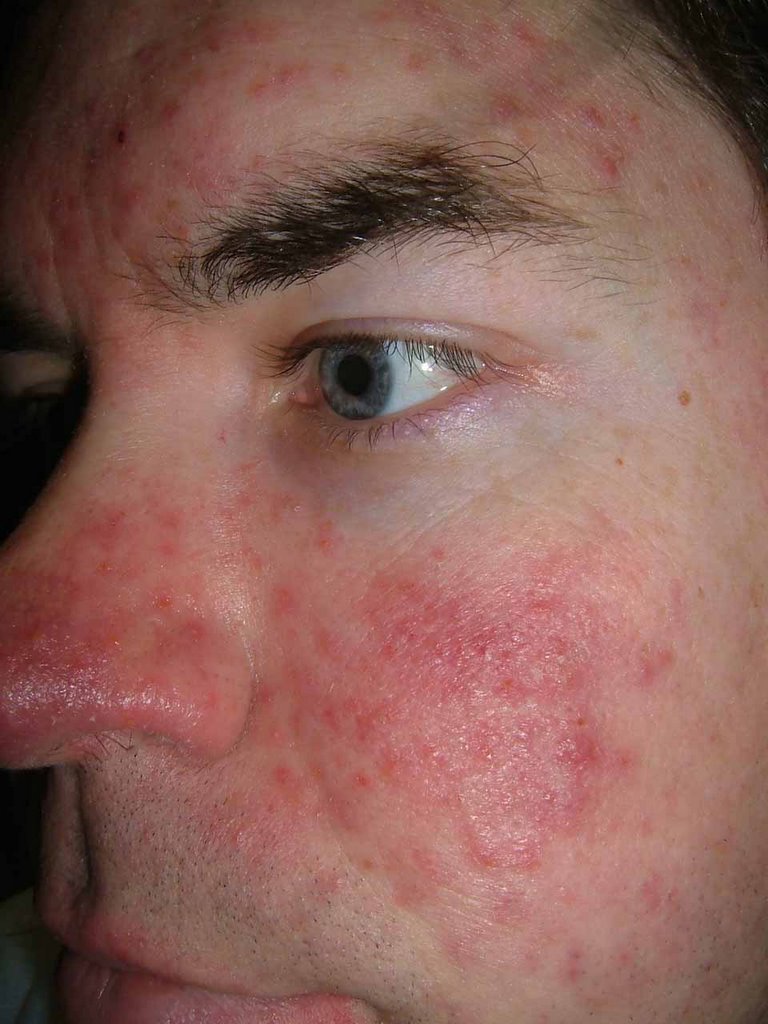
📝 Exam Pearls
- 🚫 No comedones → key differentiator from acne vulgaris
- 👃 Rhinophyma → severe, late complication, mostly in men
- 👁 Ocular involvement → sight-threatening if untreated, urgent referral
- 💡 Flushing precedes persistent erythema; papules/pustules appear later
- 🧪 Topical steroids worsen rosacea → teach patients to avoid
📚 References & NICE Resources

Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
