| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Juvenile Myoclonic epilepsy (JME)
Related Subjects: |Status Epilepticus (Epilepsy) |Coma management |Lorazepam |Phenytoin |Levetiracetam |Epilepsy - General Management |First Seizure |Epilepsy in Pregnancy |Febrile seizures
🧠 About
- Juvenile Myoclonic Epilepsy (JME) is a classic genetic generalised epilepsy. Myoclonic jerks are often misinterpreted as clumsiness, leading to delayed diagnosis.
- ⚠️ Can deteriorate with inappropriate antiseizure medicines (carbamazepine, phenytoin, vigabatrin).
- Non-progressive condition with preserved intellect and normal neurological examination.
🧬 Aetiology & Genetics
- Strong heritable component with altered thalamocortical excitability.
- Positive family history in ~50% of patients.
- Mild female predominance; multiple susceptibility genes suspected rather than a single defect.
📊 Epidemiology
- Prevalence: ~1 in 2000.
- Onset typically between 10–18 years.
- Typical sequence: childhood absence → adolescent myoclonus → generalised tonic–clonic seizures in late teens.
⚡ Seizure Types
- Absence Seizures: Brief lapses in awareness, often shortly after waking.
- Myoclonic Jerks: Sudden bilateral upper-limb jerks within an hour of waking - the classic “🍳 breakfast-time” phenomenon.
- Generalised Tonic–Clonic Seizures: Commonly follow clusters of morning myoclonus.
🔍 Clinical Features & Triggers
- Morning predominance of all seizure types.
- Triggers include sleep loss, alcohol (especially next morning), stress, and photic activation in some.
- No cognitive decline, behavioural regression, or motor deterioration.
🧪 Investigations
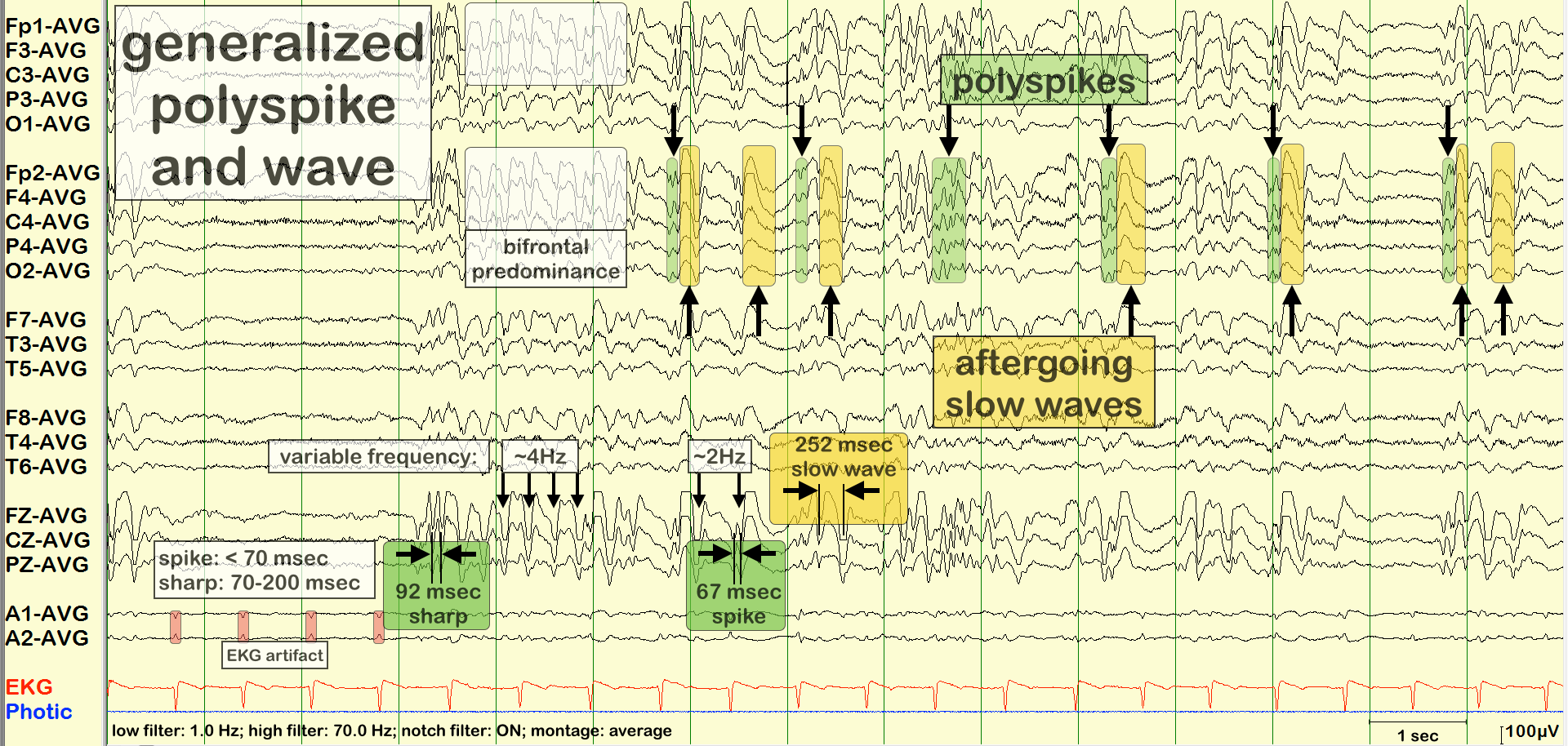
- EEG: Generalised 3–6 Hz polyspike–wave discharges. Markedly enhanced by sleep-deprivation, hyperventilation, or photic stimulation.
- MRI: Typically normal; used to exclude structural mimics.
- Bloods: Normal; performed to rule out metabolic provocation.
💊 Management
- Long-term antiseizure therapy is usually required due to high relapse risk.
- First-line: Sodium valproate (most effective; avoid in women of childbearing potential).
- Alternatives: Levetiracetam, topiramate, lamotrigine (may aggravate myoclonus), and zonisamide.
- Avoid: Carbamazepine, phenytoin, gabapentin, vigabatrin - all may worsen generalised epilepsies.
- Lifestyle: Emphasise sleep hygiene, alcohol moderation, and strict adherence to medication.
📌 References
- Strong heritable component with altered thalamocortical excitability.
- Positive family history in ~50% of patients.
- Mild female predominance; multiple susceptibility genes suspected rather than a single defect.
📊 Epidemiology
- Prevalence: ~1 in 2000.
- Onset typically between 10–18 years.
- Typical sequence: childhood absence → adolescent myoclonus → generalised tonic–clonic seizures in late teens.

⚡ Seizure Types
- Absence Seizures: Brief lapses in awareness, often shortly after waking.
- Myoclonic Jerks: Sudden bilateral upper-limb jerks within an hour of waking - the classic “🍳 breakfast-time” phenomenon.
- Generalised Tonic–Clonic Seizures: Commonly follow clusters of morning myoclonus.
🔍 Clinical Features & Triggers
- Morning predominance of all seizure types.
- Triggers include sleep loss, alcohol (especially next morning), stress, and photic activation in some.
- No cognitive decline, behavioural regression, or motor deterioration.
🧪 Investigations
- EEG: Generalised 3–6 Hz polyspike–wave discharges. Markedly enhanced by sleep-deprivation, hyperventilation, or photic stimulation.
- MRI: Typically normal; used to exclude structural mimics.
- Bloods: Normal; performed to rule out metabolic provocation.
💊 Management
- Long-term antiseizure therapy is usually required due to high relapse risk.
- First-line: Sodium valproate (most effective; avoid in women of childbearing potential).
- Alternatives: Levetiracetam, topiramate, lamotrigine (may aggravate myoclonus), and zonisamide.
- Avoid: Carbamazepine, phenytoin, gabapentin, vigabatrin - all may worsen generalised epilepsies.
- Lifestyle: Emphasise sleep hygiene, alcohol moderation, and strict adherence to medication.
📌 References
- Absence Seizures: Brief lapses in awareness, often shortly after waking.
- Myoclonic Jerks: Sudden bilateral upper-limb jerks within an hour of waking - the classic “🍳 breakfast-time” phenomenon.
- Generalised Tonic–Clonic Seizures: Commonly follow clusters of morning myoclonus.
🔍 Clinical Features & Triggers
- Morning predominance of all seizure types.
- Triggers include sleep loss, alcohol (especially next morning), stress, and photic activation in some.
- No cognitive decline, behavioural regression, or motor deterioration.
🧪 Investigations
- EEG: Generalised 3–6 Hz polyspike–wave discharges. Markedly enhanced by sleep-deprivation, hyperventilation, or photic stimulation.
- MRI: Typically normal; used to exclude structural mimics.
- Bloods: Normal; performed to rule out metabolic provocation.
💊 Management
- Long-term antiseizure therapy is usually required due to high relapse risk.
- First-line: Sodium valproate (most effective; avoid in women of childbearing potential).
- Alternatives: Levetiracetam, topiramate, lamotrigine (may aggravate myoclonus), and zonisamide.
- Avoid: Carbamazepine, phenytoin, gabapentin, vigabatrin - all may worsen generalised epilepsies.
- Lifestyle: Emphasise sleep hygiene, alcohol moderation, and strict adherence to medication.
📌 References
- EEG: Generalised 3–6 Hz polyspike–wave discharges. Markedly enhanced by sleep-deprivation, hyperventilation, or photic stimulation.
- MRI: Typically normal; used to exclude structural mimics.
- Bloods: Normal; performed to rule out metabolic provocation.
💊 Management
- Long-term antiseizure therapy is usually required due to high relapse risk.
- First-line: Sodium valproate (most effective; avoid in women of childbearing potential).
- Alternatives: Levetiracetam, topiramate, lamotrigine (may aggravate myoclonus), and zonisamide.
- Avoid: Carbamazepine, phenytoin, gabapentin, vigabatrin - all may worsen generalised epilepsies.
- Lifestyle: Emphasise sleep hygiene, alcohol moderation, and strict adherence to medication.
📌 References
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
