| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
General Basic Fracture management
Fracture Management 🦴 follows the sequence: 👉 ABCDE → Analgesia → Assessment → Imaging → Reduction & Stabilisation → Rehabilitation. Always prioritise life before limb (ATLS principles).
📖 About
- A fracture = break in bone continuity, partial or complete.
- Causes: trauma (falls, RTAs, sports) and pathological states (osteoporosis, malignancy, Paget’s).
⚙️ Aetiology
- Direct trauma: blow at site of injury (e.g., tibial shaft fracture from kick 🚲).
- Indirect trauma: force transmitted (e.g., FOOSH → clavicle fracture ✋).
- Stress fracture: repetitive microtrauma (athletes, military recruits 🏃).
- Pathological fracture: weakened bone (osteoporosis, metastasis).
- Insufficiency fracture: minimal trauma on osteoporotic/metabolic bone.
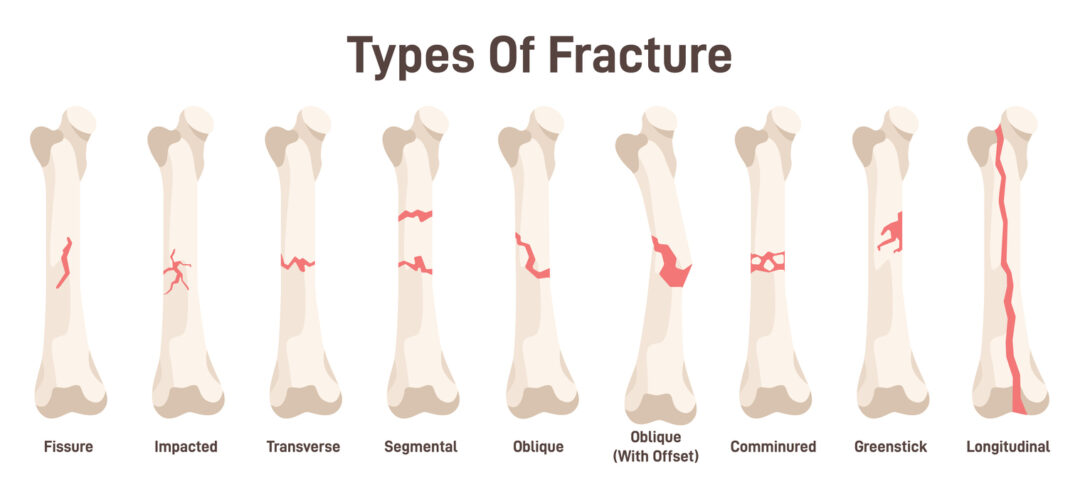
🔎 Types of Fracture
- By skin integrity: Open (compound) 🚨 vs Closed.
- By joint involvement: Intra-articular vs Extra-articular.
- By pattern: Transverse, oblique, spiral, comminuted.
- By mechanism: Avulsion, stress, crush, burst.
- By age: Greenstick, buckle/torus (paediatrics 👶).
- Fracture–dislocation: fracture associated with joint dislocation.
🩺 Clinical Assessment
- History: mechanism, handedness, occupation, comorbidities, medications (esp. steroids, bisphosphonates).
- Symptoms: pain, swelling, deformity, loss of function.
- Always examine joints above and below.
- Neurovascular exam: distal pulses, cap refill, motor & sensory function.
- Red flags 🚨: Compartment syndrome → pain out of proportion, pain on passive stretch, paraesthesia, pallor, pulselessness, paralysis.
👀 LOOK, FEEL, MOVE, ADDITIONAL
- LOOK: deformity, swelling, wounds, skin tenting, perfusion.
- FEEL: tenderness, crepitus, distal pulses, sensory loss.
- MOVE: active/passive ROM of joints above/below.
- ADDITIONAL: hand dominance (UL), weight-bearing status (LL).
🧪 Investigations
- Bloods: FBC, U&E, coagulation, G&S (esp. pelvic/femoral fractures).
- X-ray: First-line. Rule: “Two views (AP + lateral), Two joints (above + below).” 📸
- CT: complex intra-articular, spine, pelvic fractures.
- MRI: stress or occult fractures; soft tissue injury.
- Ultrasound: paediatrics - radiation-free.
💊 Management
- Initial (ATLS): ABCDE, analgesia (opioids/NSAIDs), IV fluids if NBM.
- Principles:
- Reduction: restore anatomy (closed vs open).
- Stabilisation: cast, splint, traction, external fixator, or surgical fixation.
- Rehabilitation: early mobilisation, physiotherapy, occupational therapy.
- Open fractures 🚨:
- Irrigate with saline, apply sterile saline-soaked dressing.
- IV antibiotics (e.g., cefuroxime 1.5 g IV within 1 hr).
- Tetanus prophylaxis.
- Immobilise in backslab/splint.
- Urgent orthopaedic referral for debridement + fixation (within 6 hrs if possible).
- Surgical indications:
- Open fractures
- Neurovascular compromise
- Compartment syndrome
- Unstable displaced fractures
- Intra-articular incongruity
🔧 Reduction
- Closed: manipulation, traction under sedation/anaesthesia.
- Open: surgical fixation (ORIF) - more accurate alignment but risks infection, bleeding.
📌 OSCE / Exam Pearls
- Always document neurovascular status before and after manipulation.
- Don’t forget compartment syndrome red flags - pain out of proportion is the earliest sign.
- Remember BOAST principle: “First do no harm - splint before shifting.”
- Two views, two joints rule is examinable in finals.
- Children’s greenstick fractures often remodel → conservative management preferred.
📚 References
- NICE Clinical Knowledge Summaries: Fractures.
- ATLS®: Advanced Trauma Life Support, 10th edition.
- Rockwood & Green’s Fractures in Adults, 9th edition.
- British Orthopaedic Association Standards for Trauma (BOAST).
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
