| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Carotid Endarterectomy ✅
Related Subjects: Renal Colic | Abdominal Aortic Aneurysm | Acute Abdominal Pain | Assessing Abdominal Pain | Penetrating Abdominal Trauma | Peripheral Arterial Disease (PAD) |Abdominal Aortic Aneurysm (AAA) | Carotid Endarterectomy | Buerger's disease (Thromboangiitis obliterans ) | Leriche syndrome (aortoiliac occlusive disease) | Vascular Surgery: Introduction | Acute Limb Ischaemia | Ankle-Brachial Pressure Index (ABPI) and Peripheral Vascular Disease | Peripheral Arterial Disease (PAD) | Abdominal Aortic Aneurysm (AAA) | Carotid Endarterectomy | Buerger's disease (Thromboangiitis obliterans) | Leriche syndrome (aortoiliac occlusive disease) |Acute Rhabdomyolysis |Hyperkalaemia |Acute Kidney Injury
Carotid Endarterectomy (CEA) is recommended for symptomatic carotid stenosis of 50–99% (NASCET criteria) or 70–99% (ECST criteria) in patients with recent TIA or non-disabling stroke (modified Rankin Scale ≤2), provided they are stable neurologically. Perform **urgently** — ideally as soon as possible and within **2 weeks** of the index event for maximum benefit (NICE NG128 1.2.4). Greatest absolute risk reduction occurs early after symptoms.
🧠 Evidence & Indications (NICE NG128 Compliant)
- CEA first described in the 1950s; randomised evidence from NASCET (1991) and ECST (1998) established benefit in symptomatic stenosis, reducing ipsilateral stroke risk.
- Strongest benefit: Symptomatic ≥70% stenosis (NASCET); absolute risk reduction (ARR) ~13–17% over 5 years vs medical therapy alone.
- Modest benefit: 50–69% stenosis (ARR ~7%; consider in men, recent symptoms, high-risk plaque features).
- No benefit: <50% stenosis, complete occlusion, or delayed intervention (>3–6 months).
- Timing critical: Benefit highest if CEA performed early (within days to 2 weeks of TIA/non-disabling stroke); delays reduce efficacy. Urgent referral via TIA clinic mandatory.
- Operator/centre factors: Perioperative stroke/death rate should be <6% (NICE standard); high-volume surgeons/centres preferred (audit via national registries e.g., UK National Vascular Registry).
- Stenosis measurement formula (NASCET): % stenosis = [1 - (minimal residual lumen diameter ÷ normal distal ICA diameter)] × 100. Reports must specify NASCET or ECST method (NG128 1.2.6).
- No routine CEA for asymptomatic stenosis (NG128 does not recommend; focus on BMT unless very high-risk features in specialist settings per other guidances).
🔬 Investigations
- First-line: Duplex ultrasound (carotid Doppler USS) — non-invasive, widely available, good sensitivity/specificity for ≥50% stenosis.
- Confirmatory/Planning: Contrast-enhanced MRA or CTA (preferred for detailed anatomy, plaque characteristics, and planning intervention).
- Consider dual-modality imaging (e.g., USS + MRA/CTA) before CEA to confirm degree and exclude tandem lesions (NG128 supports urgent carotid imaging in candidates).
- Avoid routine invasive DSA unless non-invasive imaging inconclusive.
- Brain imaging: MRI (diffusion-weighted) if needed to confirm ischaemic territory or exclude alternatives (NG128 1.2.2).
⚙️ The Procedure
- Anaesthesia: Local (preferred for neurological monitoring) or general.
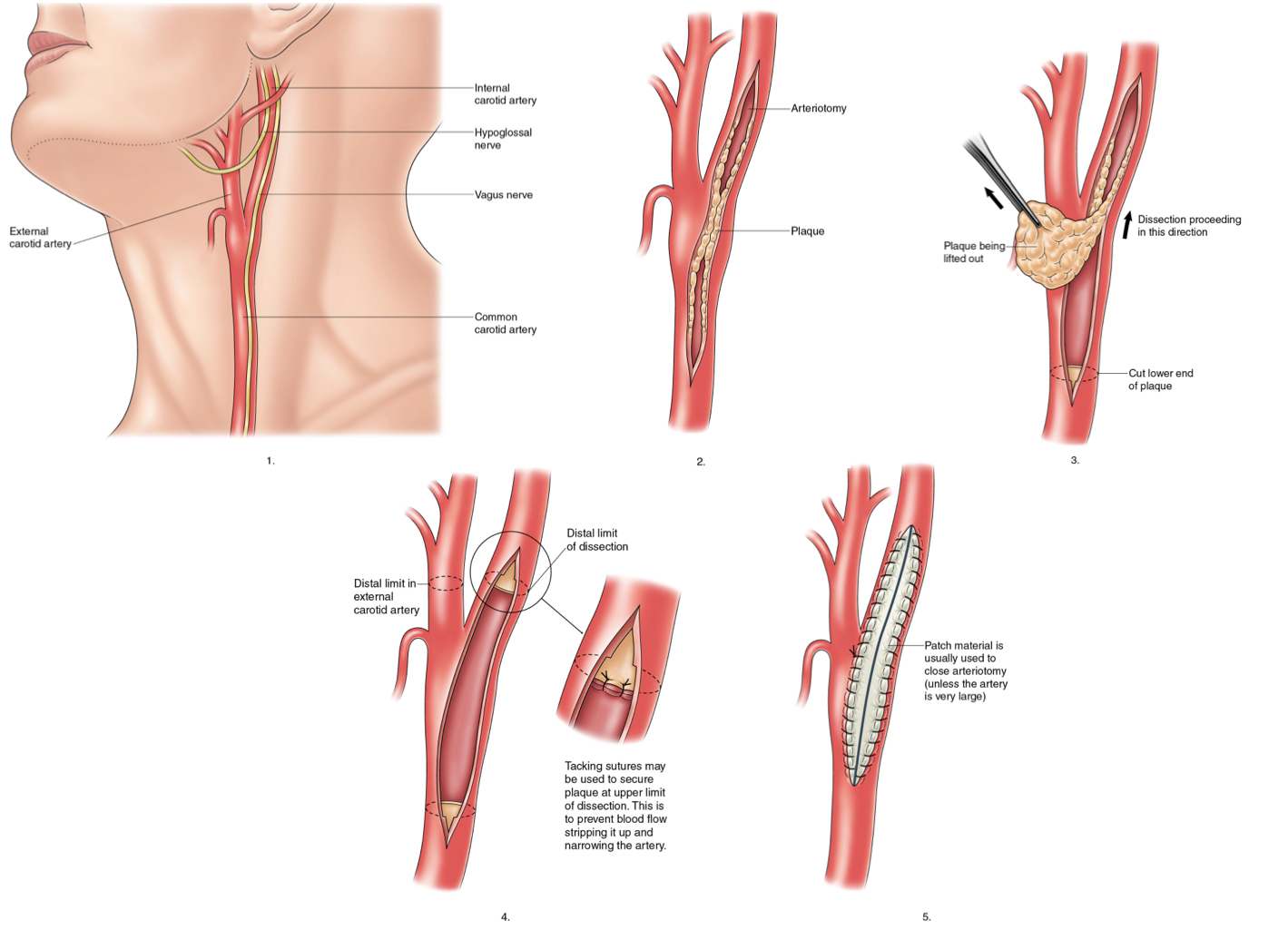
- Surgical steps: Neck incision; carotid exposure; clamping (test clamping or routine/selective shunting to maintain cerebral perfusion); arteriotomy; plaque endarterectomy; closure (primary suture or patch angioplasty — synthetic or vein — to reduce restenosis risk).
- Duration: Typically 60–120 minutes.
- Post-op: HDU/ICU monitoring for 24 hours (BP control to prevent hyperperfusion; neurological checks); most discharged day 1–2 if uncomplicated.
- Alternatives: Carotid artery stenting (CAS) considered in select high-surgical-risk patients (e.g., hostile neck, recent MI) per NICE IPG389 (2011; still current).
⚠️ Complications
| Complication | Incidence & Details | Management |
|---|---|---|
| Perioperative ischaemic stroke | ~2–6% (target <6%); embolic, thrombotic, or haemodynamic. | Urgent CT head (exclude ICH); CTA/MRA; antiplatelets ± re-exploration/endovascular rescue. |
| Cerebral hyperperfusion syndrome | 1–3%; days 3–10 post-op; headache, seizures, focal deficits, ICH due to impaired autoregulation. | Strict BP control (<140/90 mmHg or lower); anticonvulsants if seizures; neuroimaging (CT/MRI). |
| Restenosis | ~5–10% at 2–5 years; early (neointimal) or late (atherosclerotic). | Surveillance Duplex; medical optimisation; CAS or redo CEA if symptomatic. |
| Cranial nerve injury | 5–10% (hypoglossal, vagus, marginal mandibular, glossopharyngeal); usually transient. | Conservative; speech/swallow therapy; rarely permanent. |
| Post-op ICH | Rare (<1%); often related to hyperperfusion or antithrombotics. | Reverse anticoagulation; neurosurgical consult if large/mass effect. |
| Wound haematoma/infection | 1–5%; airway compromise possible. | Evacuation if expanding; antibiotics. |
| Myocardial infarction | 1–3%; higher in cardiac comorbidity. | Peri-op risk stratification (e.g., revised cardiac risk index). |
💊 Best Medical Therapy (Alongside or Instead of CEA – NG128 Compliant)
- Antiplatelet: Aspirin 75 mg daily (or clopidogrel 75 mg if intolerant); dual short-term in some high-risk cases.
- Lipid-lowering: High-intensity statin (e.g., atorvastatin 80 mg) targeting LDL <1.8 mmol/L.
- BP control: Target <130/80 mmHg (or lower if tolerated); ACEi/ARB first-line.
- Lifestyle: Smoking cessation (vital — halves recurrence risk); healthy diet, regular exercise, diabetes optimisation, alcohol moderation.
- Continue lifelong; BMT alone for non-surgical candidates or <50% stenosis.
📊 Secondary Stroke Prevention Benefit with CEA (Pooled NASCET/ECST Data)
| Severity of Stenosis (Symptomatic) | Relative Risk Reduction (5 yrs) | Absolute Risk Reduction (2 yrs approx.) | NNT (to prevent 1 stroke over 2–5 yrs) |
|---|---|---|---|
| Occluded | No role for CEA | — | — |
| 70–99% (NASCET) | ~65% | ~13–17% | ~6–8 |
| 50–69% (NASCET) | ~30% | ~7% | ~14 |
| <50% (NASCET) | No benefit | — | — |
💡 Key takeaway: Greatest benefit from CEA occurs early after TIA/non-disabling stroke (within 2 weeks; days if TIA-dominant). Reduced efficacy in women (lower ARR), ocular-only events (amaurosis fugax), lacunar strokes, contralateral occlusion, or delayed presentation. Always combine with aggressive BMT. Discuss in multidisciplinary team; refer urgently to vascular/stroke services meeting national standards.
📚 References (Current as of March 2026)
- NICE NG128 – Stroke and transient ischaemic attack in over 16s (2019; current) – Sections 1.2.3–1.2.6 on carotid imaging & urgent CEA.
- NASCET & ECST pooled analyses (Lancet/Rothwell et al.).
- NICE interventional procedures (e.g., IPG389 on CAS as alternative).
- 2023 NICE exceptional surveillance: No update needed for CEA recommendations.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
