| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
AIDS (HIV) Respiratory disease
Related Subjects: |AIDS (HIV) Neurological Disease |AIDS (HIV) Respiratory disease |AIDS Dementia Complex (HIV) |AIDS HIV Infection |AIDS(HIV) Gastrointestinal Disease |Acute Retroviral Syndrome (HIV) |HIV and Post-Exposure Prophylaxis (PEP) |HIV and Pre-exposure prophylaxis |HIV associated nephropathy (HIVAN) |HIV disease Assessment
🫁 Respiratory diseases are common in individuals with AIDS (Acquired Immunodeficiency Syndrome) due to their weakened immune systems. 🛡️⬇️
These diseases can be caused by a variety of opportunistic pathogens, including bacteria 🦠, viruses 🧬, fungi 🍄, and parasites 🪱.
Below is an overview of some common respiratory diseases associated with AIDS.
✅ UK guideline framing: In people living with HIV, the “big three” practical considerations are:
(1) CD4 count/viral load 📉 (risk stratifies OIs), (2) urgency of treatment ⏱️ (e.g., PCP, TB), and (3) ART timing + drug–drug interactions 💊⚠️.
BHIVA’s pulmonary opportunistic infection guidance provides UK-specific recommendations for diagnosis, treatment and prophylaxis. 🇬🇧📚
🧫 Bacterial Infections
- 🫁 Pneumonia :
- Often caused by Streptococcus pneumoniae and Haemophilus influenzae.
- Symptoms: Cough 😷, fever 🌡️, chest pain 💥, and difficulty breathing 😮💨.
- Treatment: Antibiotics 💊 and supportive care 🛌.
- Guideline notes (UK): treat promptly using local CAP pathway 🧾 and consider broader cover if severe disease/very low CD4; always send cultures 🧪 where possible and reassess early if no response. (BHIVA pulmonary OI guidance)
- 🧬 Mycobacterium tuberculosis (TB) :
- HIV-infected individuals are at higher risk for active TB.
- Symptoms: Chronic cough 😷, weight loss ⚖️⬇️, night sweats 🌙💦, and fever 🌡️.
- CXR: atypical features e.g. infectivity without cavitation. Mid zonal rather than apical findings. 🩻
- Treatment: Combination of anti-tuberculous drugs 💊💊 for an extended period.
- Guideline notes (UK): send sputum for AFB smear/culture + rapid molecular testing 🧪 (e.g., rifampicin resistance where available); manage with TB/HIV specialist team because ART timing and interactions (rifampicin) are critical ⚠️. (BHIVA TB/HIV; NICE TB NG33)
- 🧫 Mycobacterium avium complex (MAC) :
- Occurs in advanced HIV infection (CD4 count < 50 cells/µL) 📉.
- Symptoms: Fever 🌡️, weight loss ⚖️⬇️, night sweats 🌙💦, and respiratory symptoms 😮💨.
- Treatment: Combination antibiotic therapy 💊.
- Guideline notes (UK): think “advanced disease” + consider disseminated NTM (blood cultures 🧪, systemic symptoms); BHIVA has dedicated NTM guidance and discusses prophylaxis and management strategies. (BHIVA NTM OI guidance)
🧬 Viral Infections
- 🧬 Cytomegalovirus (CMV) :
- Can cause pneumonia in HIV-infected individuals.
- Symptoms: Fever 🌡️, cough 😷, and shortness of breath 😮💨.
- Treatment: Antiviral medications 💊 such as ganciclovir or valganciclovir.
- Guideline notes (UK): CMV pneumonitis is uncommon but serious in advanced immunosuppression; BHIVA pulmonary OI guidance recommends ganciclovir as standard therapy and highlights treating co-pathogens first if present and reassessing response 🔁. (BHIVA pulmonary OI guidance)
- 🧬 Herpes Simplex Virus (HSV) :
- May cause severe respiratory disease in immunocompromised patients.
- Symptoms: Fever 🌡️, cough 😷, and respiratory distress 🚨.
- Treatment: Antiviral therapy 💊 with acyclovir or valacyclovir.
- Guideline notes (UK): true HSV lower respiratory tract disease is rare; consider alternative diagnoses and confirm with appropriate sampling/PCR 🧪 where possible (especially if ventilated). (BHIVA pulmonary OI guidance)
🍄 Fungal Infections
- 🍄 Pneumocystis jirovecii pneumonia (PCP) :
- One of the most common opportunistic infections in AIDS patients.
- Mild to moderate dyspnoea 😮💨, exercise hypoxia 🧗♂️⬇️O₂. Pulmonary infiltrates on CXR 🩻. Low CD4 count < 200 📉.
- Symptoms: Fever 🌡️, non-productive cough 😷, and shortness of breath 😮💨.
- Complications: Pneumothorax 💥🫁
- Treatment: Trimethoprim-sulfamethoxazole (TMP-SMX) 💊 or alternative regimens if allergic ⚠️.
- Guideline notes (UK): PCP is often subacute with exertional desaturation and disproportionate hypoxia; BHIVA pulmonary OI guidance covers severity assessment, corticosteroids in moderate–severe disease, and primary/secondary prophylaxis (typically for CD4 <200). (BHIVA pulmonary OI guidance; BNF/NICE PCP summary)
- 🍄 Cryptococcosis :
- Caused by Cryptococcus neoformans, can lead to severe pneumonia.
- Symptoms: Cough 😷, fever 🌡️, and chest pain 💥.
- Treatment: Antifungal medications 💊 such as fluconazole or amphotericin B.
- Guideline notes (UK): always ask about headache 🤕/photophobia 💡 and consider meningitis; management is usually specialist-led with induction/ consolidation phases. (BHIVA OI guidance)
- 🍄 Histoplasmosis :
- Caused by Histoplasma capsulatum, can disseminate in immunocompromised individuals.
- Symptoms: Fever 🌡️, cough 😷, and shortness of breath 😮💨.
- Treatment: Antifungal therapy 💊 with itraconazole or amphotericin B.
- UK note: consider travel/exposure history ✈️🌍; uncommon in the UK but important in returned travellers and can mimic TB or malignancy. (BHIVA OI guidance)
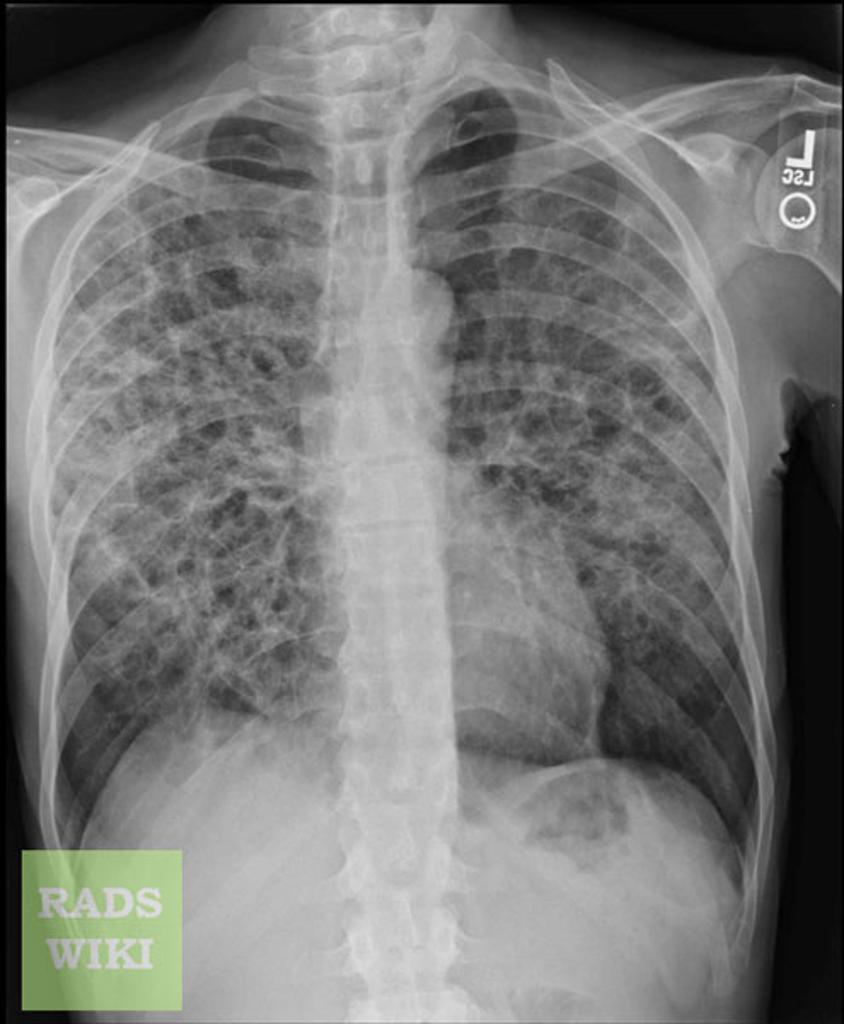 🩻 Pneumocystis Pneumonia
🩻 Pneumocystis Pneumonia
🪱 Parasitic Infections
- 🪱 Toxoplasmosis :
- Caused by Toxoplasma gondii, can lead to severe respiratory symptoms.
- Symptoms: Fever 🌡️, cough 😷, and shortness of breath 😮💨.
- Treatment: Combination therapy 💊 with pyrimethamine and sulfadiazine.
- Guideline note: pulmonary toxoplasmosis is uncommon; in advanced HIV, always assess for CNS symptoms 🧠 because encephalitis is a classic presentation. (BHIVA OI guidance)
🩺 Practical approach (UK bedside framing)
- Risk stratify: latest CD4 📉, viral load 🧬, ART status/adherence 💊✅, prophylaxis history (PCP prophylaxis?) 🛡️, recent travel ✈️ and TB exposure 🧫.
- Immediate tests: CXR 🩻, SpO2/ABG if hypoxic 🫁⬇️, blood cultures if febrile 🧪, sputum for microscopy/culture + TB testing where appropriate; consider CT chest if CXR non-diagnostic and suspicion persists 🔍.
- Don’t miss: PCP (subacute dyspnoea + exertional desaturation) 😮💨, TB (systemic symptoms) 🌙💦, bacterial CAP (acute consolidation) 🩻, PE (hypercoagulability + immobility) 🩸, malignancy (Kaposi/lymphoma) 🎗️.
- Drug interactions: rifampicin–ART ⚠️, azoles–ART ⚠️, macrolides–ART ⚠️ → involve HIV/TB/ID pharmacists early 👩⚕️👨⚕️. (BHIVA TB/HIV; BHIVA OI guidance)
🛡️ Prevention and Management
- Prophylactic medications (e.g., TMP-SMX for PCP) 💊🛡️ for high-risk patients.
- Regular monitoring of CD4 counts 📉 and viral load 🧬.
- Early initiation of antiretroviral therapy (ART) 💊 to maintain immune function 🛡️.
- Vaccinations (e.g., pneumococcal, influenza) 💉 to prevent infections.
- Prompt treatment of respiratory symptoms and infections 🚨.
- Guideline notes (UK): BHIVA pulmonary OI guidance covers PCP prophylaxis thresholds and stopping rules after immune reconstitution; annual influenza vaccination follows UK national programme guidance; pneumococcal vaccination is recommended for many people living with HIV depending on age/risk and local schedule. (BHIVA pulmonary OI guidance; BNF immunisation schedule; UKHSA flu programme)
📚 References (UK)
- BHIVA pulmonary opportunistic infections guideline (2024) 📘
- BHIVA pulmonary OI guideline PDF (2024) 📄
- BHIVA TB/HIV guidelines (2018 with updates highlighted) 🧫
- NICE NG33: Tuberculosis (recommendations) 🇬🇧
- BHIVA non-tuberculous mycobacteria guideline (2024) 🧪
- BNF/NICE treatment summary: Pneumocystis pneumonia (PCP) 💊
- UKHSA/NHS flu programme information 💉
- BNF/NICE immunisation schedule summary 📅
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
