| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Sturge Weber syndrome
Related Subjects: |Subarachnoid Haemorrhage |Dural Arteriovenous Malformations |Pulmonary Arteriovenous malformation |Sturge Weber syndrome
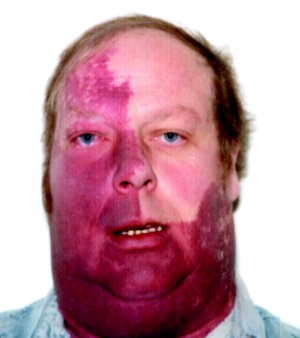
🍷🧠👁️ Sturge–Weber syndrome (SWS) is a sporadic neurocutaneous vascular disorder caused by a post-zygotic (mosaic) somatic mutation. It classically features a facial port-wine stain (capillary malformation), leptomeningeal angiomatosis (pial vascular malformation), and ocular disease (especially glaucoma). Neurological morbidity is mainly driven by chronic venous congestion → cortical ischaemia → seizures, stroke-like episodes and progressive atrophy.
📖 About
- Nature: Congenital, non-inherited (sporadic), due to somatic mosaicism.
- Core triad: 🍷 facial capillary malformation + 🧠 leptomeningeal angioma + 👁️ glaucoma (variable combination).
- Typical distribution: Port-wine stain often involves the ophthalmic (V1) region; risk of brain/eye involvement is higher with V1 (especially upper eyelid) involvement.
🧬 Genetics & Pathophysiology
- Cause: Somatic activating mutation in GNAQ (mosaic) → abnormal vascular development.
- Brain mechanism: Leptomeningeal venous malformation → impaired cortical venous drainage → chronic hypoperfusion and “vascular steal” → gliosis, calcification, and hemispheric atrophy.
- Why seizures? Irritable, hypoperfused cortex + gliosis → lower seizure threshold; early-onset seizures predict worse cognitive outcome.
- Why calcification? Chronic cortical injury → dystrophic gyriform (“tram-track”) calcifications, classically in parieto-occipital cortex.
🧾 Roach Classification (Types)
Most teaching uses the Roach classification (Types I–III), based on whether SWS involves the face (port-wine stain) 🍷, the leptomeninges (brain) 🧠, and/or the eye (glaucoma) 👁️.
- Type I (classic / most common) 🍷🧠 (±👁️)
- Facial port-wine stain + leptomeningeal angioma.
- Glaucoma may occur (often ipsilateral; can be early or later).
- Type II 🍷 (±👁️)
- Facial port-wine stain only (no leptomeningeal involvement).
- Glaucoma may occur.
- Type III 🧠
- Leptomeningeal angioma only (typically no facial port-wine stain).
- Often presents later with seizures/headache/neurological events; glaucoma is uncommon but assess eyes anyway 👁️.
🩺 Clinical Presentation
- Skin 🍷: facial port-wine stain present at birth; commonly V1/V2 distribution.
- Neurology 🧠:
- Seizures (often in infancy/early childhood; focal ± secondary generalisation).
- Stroke-like episodes or transient neurological deficits (weakness, visual symptoms) due to hypoperfusion/venous congestion.
- Hemiparesis (often contralateral to brain involvement), developmental delay, learning difficulties.
- Headache/migraine can be prominent.
- Visual field deficit (occipital involvement) e.g., homonymous hemianopia.
- Eye 👁️:
- Glaucoma (can be congenital/early-onset or develop later).
- Choroidal haemangioma → visual impairment, retinal complications.
🖼️ Imaging & hallmark findings
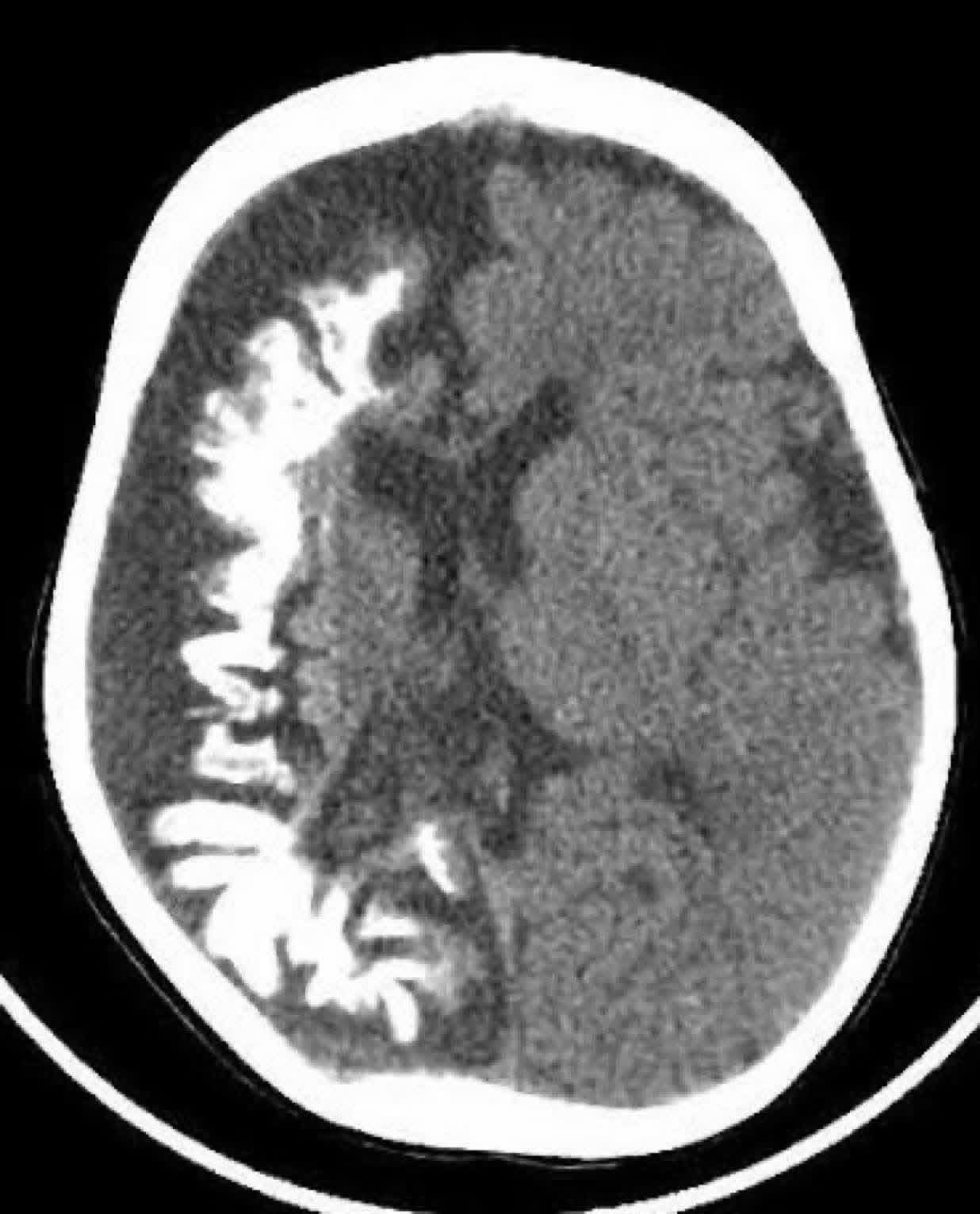
🧠 “Tram-track” calcifications are the classic imaging hallmark of SWS. They represent gyriform cortical/subcortical calcification, often parieto-occipital, with associated hemispheric atrophy and sometimes calvarial thickening.
🧪 Investigations
- 🩻 CT brain: can show gyriform (“tram-track”) calcification and hemispheric volume loss (often later in disease).
- 🧲 MRI brain with contrast (key test): leptomeningeal enhancement, pial angioma, cortical atrophy; consider SWI for venous abnormalities.
- 🩸 MRV/MRA (where available): evaluates venous drainage anomalies and associated vascular features.
- ⚡ EEG: for seizure classification, lateralisation, and presurgical work-up if refractory epilepsy.
- 👁️ Ophthalmology assessment: urgent baseline + ongoing monitoring (IOP, optic nerve, choroidal haemangioma).
⚠️ Complications
- ⚡ Epilepsy (including refractory focal epilepsy; status epilepticus risk).
- 🧠 Progressive neurological impairment: hemiparesis, cognitive decline, developmental delay.
- 🧩 Stroke-like episodes / transient deficits (hypoperfusion/venous congestion).
- 👁️ Glaucoma → optic nerve damage and vision loss if untreated.
- 🩸 Intracranial haemorrhage is less central than in AVMs, but vascular fragility/venous hypertension can contribute to complications.
⚖️ Management (practical, multidisciplinary)
- Seizure control ⚡:
- Early recognition and treatment of focal seizures; optimise anti-seizure medication and adherence.
- Refractory epilepsy → refer to tertiary epilepsy service for presurgical evaluation (EEG + MRI ± PET/SPECT).
- Stroke-like episodes / neurological decline 🧠:
- Supportive management, avoid dehydration and hypotension; treat triggers (infection, poor sleep, missed meds).
- Consider specialist advice regarding antiplatelet use in recurrent stroke-like episodes (practice varies; individualised risk/benefit).
- Ophthalmology 👁️:
- Urgent assessment for glaucoma at diagnosis, then ongoing monitoring.
- Manage glaucoma with drops and/or surgery per ophthalmology; treat choroidal haemangioma complications if present.
- Dermatology / laser therapy 🍷:
- Pulsed dye laser can improve port-wine stain appearance (cosmetic + psychosocial benefit).
- Neurodevelopment & rehab 🧑🏫:
- Early developmental assessment; physiotherapy/OT/speech and language support as needed.
- Education planning and family support are central to long-term outcomes.
📉 Prognosis
- Earlier seizure onset, frequent seizures, and extensive unilateral leptomeningeal involvement are associated with worse neurodevelopmental outcomes.
- Good seizure control and early multidisciplinary care improve function and quality of life.
- Ocular prognosis depends on early detection and control of glaucoma.
💡 Exam Pearls
- 🍷 Port-wine stain in V1 distribution → think SWS and check brain + eyes.
- 🧠 Tram-track calcifications + seizures + hemiparesis → classic triad.
- 👁️ Glaucoma can be early or late → needs ongoing surveillance.
📖 References
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
