Related Subjects:
|CEA
|ALP
|LDH
💡 With effective treatment, the overall five-year survival rate in testicular cancer is ~97%.
Orchidectomy is both diagnostic and therapeutic. Discuss sperm banking early for men wishing to preserve fertility.
📖 About
- 95% of testicular cancers are primordial germ cell tumours.
- Most common solid tumour in men aged 20–40.
- In men >50, always consider testicular lymphoma.
- Seminomas – best prognosis (>90% cure).
- Choriocarcinomas – most aggressive, worst prognosis.
🧬 Aetiology
- Split into Seminomas (≈50%) and Non-seminomatous germ cell tumours (NSGCTs).
- Lymphatic drainage:
- Right testis → interaortocaval nodes (just below right renal vein).
- Left testis → para-aortic nodes (just below left renal vein).
⚠️ Risk Factors
- Cryptorchidism (esp. abdominal testis; risk ↓ with early orchiopexy).
- Personal/family history of testicular cancer.
- Testicular feminisation, Klinefelter’s syndrome.
- Caucasian men at higher risk.
🆚 Quick Comparison: Seminoma vs Non-Seminoma
- Seminomas: Spread later, highly radiosensitive, better prognosis, typically affect older men (30–50).
- NSGCTs: Spread earlier (often haematogenous), less radiosensitive, worse prognosis, affect younger men (15–35).
👨⚕️ Clinical Features
- Painless, firm intratesticular lump (must always → testicular USS in 20–40 y/o men).
- Scrotal heaviness or dull ache.
- Gynaecomastia from ↑ β-hCG (esp. choriocarcinoma, seminoma with syncytiotrophoblasts).
- Metastatic features: back pain (retroperitoneal nodes), cough/haemoptysis (lung mets), neuro symptoms (brain mets).
🔍 Investigations
- FBC, U&E, LFTs, calcium, ALP.
- Urine pregnancy test (β-hCG positive in many cases).
- Tumour markers:
- LDH – elevated in bulk disease (prognostic marker).
- AFP – never raised in seminoma; ↑ in NSGCTs (esp. yolk sac, embryonal).
- β-hCG – raised in choriocarcinoma, some NSGCTs, and ~10% seminomas.
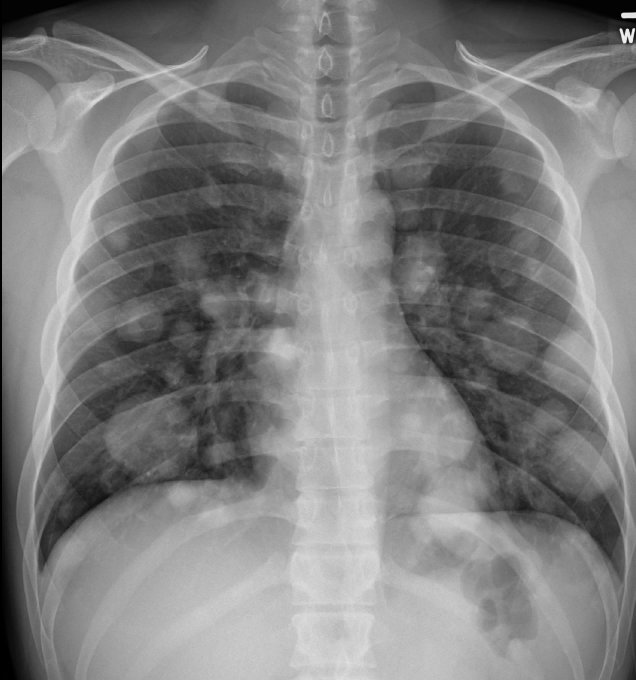
- Imaging: Scrotal USS (first-line), CXR (look for cannonball mets), CT chest/abdomen/pelvis (staging).
- ❌ Never biopsy percutaneously → risk of tumour seeding.
🧪 Histological Types
- Germ cell tumours (95%): Seminoma, Embryonal carcinoma, Yolk sac tumour, Choriocarcinoma, Teratoma, Mixed GCTs.
- Non–germ cell (rare): Leydig, Sertoli, granulosa, gonadoblastoma, stromal tumours, lymphoma.
📊 Staging
- Stage I: Confined to testis/cord.
- Stage II: Retroperitoneal node involvement (below diaphragm).
- Stage III: Distant metastases or supradiaphragmatic nodes.
💉 Treatment
- Urgent 2WW referral for any painless testicular enlargement or change in consistency.
- Radical inguinal orchidectomy (RIO): First-line in all suspected cases.
- Seminoma: Orchidectomy ± retroperitoneal radiotherapy (Stage I–II). Very radiosensitive. Chemotherapy (BEP) in advanced disease.
- Non-Seminoma: Orchidectomy + chemotherapy (BEP: Bleomycin, Etoposide, Cisplatin). Early RPLND in selected cases. Less radiosensitive.
- Prognostic factors (poor prognosis NSGCT): AFP >10,000, HCG >50,000, LDH >10× ULN, mediastinal primary, non-pulmonary visceral mets.
📑 Summary Table
| Feature | Seminoma | Non-Seminoma |
|---|
| Typical Age | 30–50 | 15–35 |
| Tumour Markers | β-hCG ↑ (10–20%), AFP normal | AFP ↑, β-hCG ↑, LDH ↑ |
| Spread | Lymphatic (late) | Early haematogenous (lung, liver) |
| Prognosis | Excellent (>90% cure) | Variable, depends on stage/type |
| Radiotherapy | Highly sensitive | Resistant |
📌 Less Common Tumours
| Type | Examples | Notes |
|---|
| Mixed GCT | Seminoma + NSGCT | Behaves like NSGCT → treat accordingly |
| Stromal | Leydig, Sertoli | May secrete hormones → gynaecomastia, precocious puberty |
| Secondary | Lymphoma, metastatic deposits | Commonest >60 y/o; bilateral possible |
📚 References

