| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Osteonecrosis of the jaw
Related Subjects: | Bisphosphonates | Osteoporosis | Osteonecrosis of the jaw
⚠️ Osteonecrosis of the Jaw (ONJ) is a rare but serious complication of drugs that inhibit bone resorption, notably bisphosphonates and denosumab. 🦷 It involves avascular necrosis of jawbone due to impaired osteoclastic activity and microvascular compromise, leading to exposed, non-healing bone and risk of secondary infection.
🧠 About
- First recognised in 2002 in patients receiving high-dose intravenous bisphosphonates for cancer-related bone disease.
- Occurs due to suppression of normal bone turnover and impaired healing after trauma or dental procedures.
- Incidence: up to 1–10% in oncology patients on IV bisphosphonates or denosumab, and <0.1% in osteoporosis treatment.
- Typically affects the mandible > maxilla (2:1 ratio), reflecting differences in vascularity.
⚙️ Pathophysiology
- Normal bone remodelling relies on osteoclast-mediated resorption and subsequent new bone formation.
- Bisphosphonates and denosumab inhibit osteoclasts → reduced bone turnover → accumulation of microdamage.
- Reduced angiogenesis and microcirculatory changes impair bone repair capacity.
- Local trauma, infection, or dental extraction then triggers exposure and necrosis of bone.
🧬 Aetiology
- Dental or surgical trauma (tooth extraction, implants, poorly fitting dentures).
- Suppression of osteoclasts by bisphosphonates or RANKL inhibitors (denosumab).
- Chemotherapy, corticosteroids, and poor oral hygiene further increase risk.
- Cancer patients, particularly with multiple myeloma or metastatic breast/prostate cancer, are at highest risk.
💊 Causes
- 💉 Drugs: Denosumab (RANKL inhibitors), IV or oral bisphosphonates, corticosteroids, antiangiogenic agents (bevacizumab, sunitinib).
- 🏥 Cancer-related: metastatic bone disease, myeloma, head and neck radiotherapy.
- 🦠 Infection or trauma: tooth extraction, ill-fitting dentures, periodontal disease.
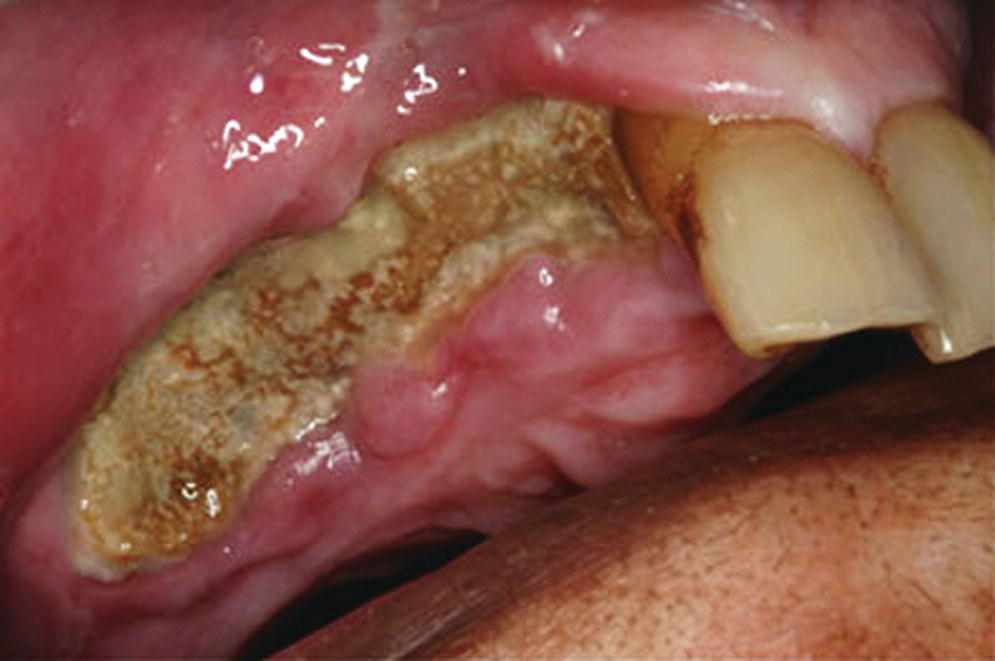
🦷 Clinical Features
- Exposed bone: hallmark sign - non-healing exposed bone in oral cavity persisting >8 weeks.
- Pain and swelling: due to secondary infection or exposed bone edges.
- Loose teeth: teeth in affected region may become mobile.
- Numbness or heaviness: due to inferior alveolar nerve involvement.
- Pus or discharge: may indicate secondary osteomyelitis.
🔍 Investigations
- Clinical examination: exposed necrotic bone, mucosal ulceration, purulent discharge.
- Imaging: OPG, CT or MRI to assess bony involvement and sequestra.
- Microbiology: swabs/cultures if infection suspected.
- Blood tests: renal function, calcium, vitamin D, inflammatory markers.
- Medication and dental history: crucial to identify bisphosphonate or denosumab exposure.
🧩 Differential Diagnosis
- Osteomyelitis of the jaw.
- Metastatic bone disease.
- Chronic periodontitis.
- Post-radiation osteonecrosis (distinct pathogenesis).
🦷 Prevention
- Comprehensive dental assessment before starting bisphosphonates or denosumab.
- Complete any required dental extractions or invasive work prior to therapy.
- Maintain excellent oral hygiene and schedule regular dental check-ups.
- Inform dentists about antiresorptive therapy before any procedure.
- Avoid elective dental extractions or implants during therapy where possible.
- Encourage smoking cessation and good nutrition to promote mucosal healing.
🩺 Management
- Conservative (early stage): Chlorhexidine mouth rinses, analgesia, antibiotics if secondary infection, and avoidance of further dental trauma.
- Medical: Consider temporary interruption of antiresorptive therapy (in consultation with specialist). Correct calcium and vitamin D deficiency.
- Surgical (advanced cases): Surgical debridement or resection of necrotic bone; reconstructive surgery if extensive involvement.
- Multidisciplinary care: Coordinate between dentist, maxillofacial surgeon, oncologist/endocrinologist.
⚠️ Key Risks and Monitoring
- Higher risk with IV bisphosphonates and high-dose denosumab (120 mg monthly for cancer).
- Lower risk with oral bisphosphonates and osteoporosis-dose denosumab (60 mg 6-monthly).
- Monitor for jaw pain, loose teeth, or non-healing ulcers.
- Reinforce patient education - early reporting prevents progression.
💡 Teaching Tip
- Explain to students that ONJ represents the “double hit” of impaired bone turnover and reduced vascularity.
- Compare with osteoradionecrosis - both cause devitalised bone, but via different mechanisms (radiation vs osteoclast suppression).
- Mnemonic: “BRONJ” = Bisphosphonate-Related OsteoNecrosis of the Jaw, though denosumab now adds “DRONJ”.
📚 References
- BNF: Denosumab and Bisphosphonates
- MHRA Drug Safety Update (2015): Osteonecrosis of the jaw with antiresorptive agents
- Ruggiero SL et al. J Oral Maxillofac Surg 2014;72(10):1938–1956 - AAOMS Position Paper on ONJ.
- NICE CKS: Osteoporosis, Bone Health (2024).
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
