| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Extradural haemorrhage
Related Subjects: |Brain Herniation syndromes |Epidural Haematoma |Subdural haematoma |Extradural haematoma🧠 The classic presentation of an Extradural Haematoma (EDH) is: ➡️ Head injury → brief loss of consciousness → lucid interval → rapid decline in GCS. 🚨 This is a neurosurgical emergency requiring urgent CT imaging and intervention.
💡 About
- EDH = bleeding between the dura mater and skull, confined by the skull’s periosteal suture lines.
- Classically arterial, most often from the middle meningeal artery.
- Rapidly progressive → may cause brain herniation if untreated.
- Accounts for ~2% of head injuries, typically in young adults (20–30 years), often after high-impact trauma.
🔎 Aetiology & Causes
- Rupture of the middle meningeal artery (or vein).
- Associated with temporal/parietal skull fractures.
- Common causes:
- Falls 🪂
- Road traffic collisions 🚗
- Assaults 🥊
- Sports injuries (e.g., skiing) ⛷️
- Rarely: birth trauma in neonates 👶
🩺 Clinical Features
- Initial head trauma ± scalp wound.
- Lucid interval → temporary recovery → rapid neurological deterioration.
- ↓ GCS, confusion, drowsiness, then coma.
- Focal neurology (e.g., hemiparesis, dilated ipsilateral pupil from CN III palsy).
- Raised ICP signs: Cheyne–Stokes respiration, bradycardia, hypertension (Cushing’s triad).
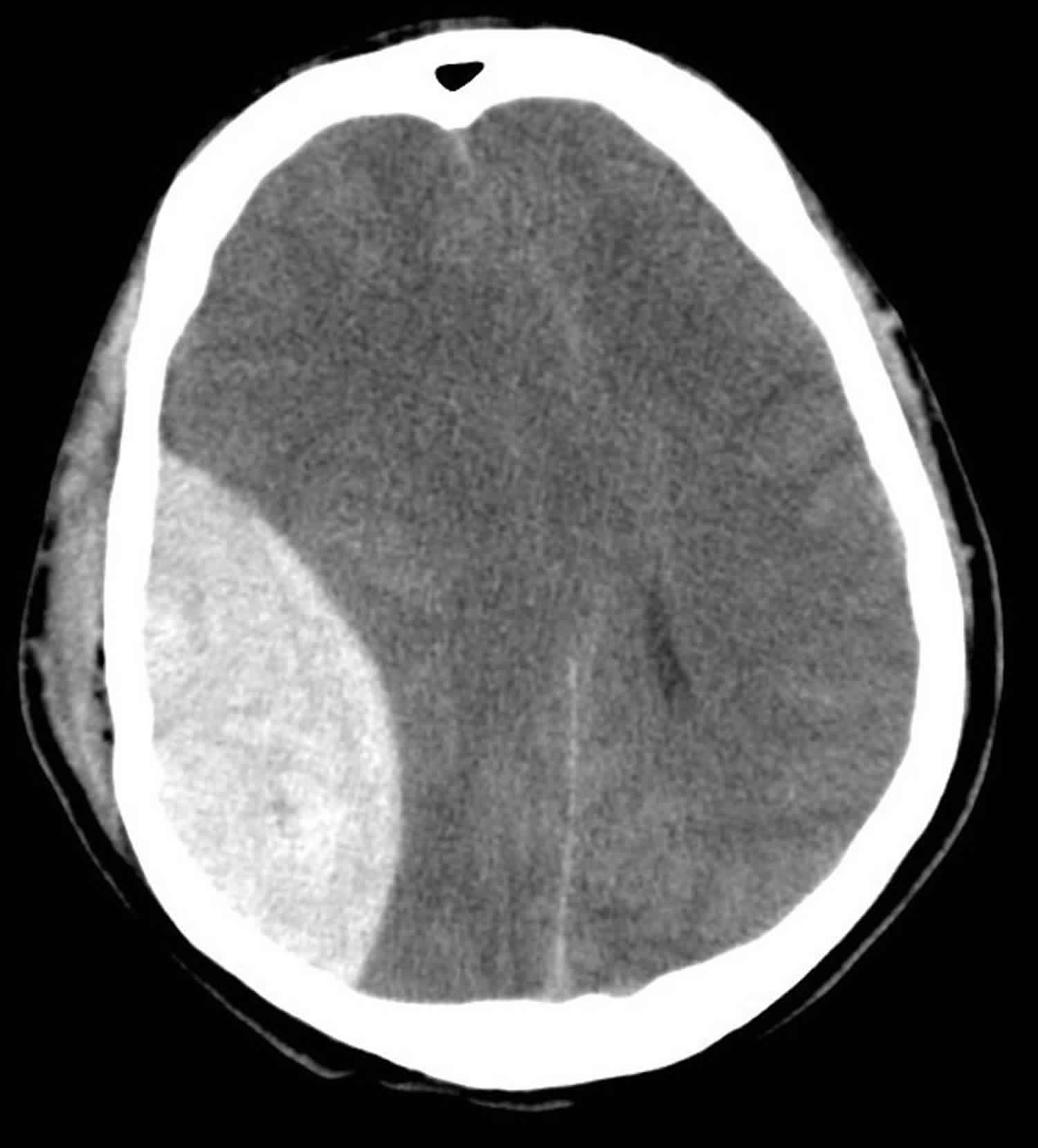
🧪 Investigations
- CT Head (Gold Standard):
- Biconvex (lens-shaped) hyperdense lesion.
- Confined by suture lines (unlike subdural haematoma).
- May show midline shift ± skull fracture.
- Bloods: FBC, U&E, LFTs, clotting screen (relevant if anticoagulated).
⚡ Management
- Initial ABC resuscitation: Secure airway, give O₂, IV fluids. Intubate if GCS < 8.
- Urgent neurosurgical referral in all suspected cases.
- Reverse coagulopathy (vitamin K, PCC if on warfarin; stop antiplatelets if safe).
- Surgery:
- Immediate evacuation indicated if clot >30 cm³, thickness >15 mm, midline shift >5 mm, or GCS ≤8 with focal deficit.
- Craniotomy = definitive treatment.
- Burr hole may be lifesaving if deterioration occurs before theatre access.
- Post-operative: ICU care with ICP monitoring, neuro-rehab as required.
📋 Key Exam Tips
✅ Lucid interval is the buzzword for EDH (but not always present).
✅ CT: biconvex/lens-shaped bleed, confined by sutures.
✅ Differentiate from Subdural Haematoma (crescent-shaped, not limited by sutures).
✅ Always think middle meningeal artery rupture in temporal fracture.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
