| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Adult Polycystic kidney disease
Related Subjects: |Metabolic acidosis |Lactic acidosis |Acute Kidney Injury (AKI) / Acute Renal Failure |Renal/Kidney Physiology |Chronic Kidney Disease (CKD) |Anaemia in Chronic Kidney Disease |Analgesic Nephropathy |Medullary Sponge kidney |IgA Nephropathy (Berger's disease) |HIV associated nephropathy (HIVAN) |Balkan endemic nephropathy (BEN) |Autosomal Dominant Polycystic kidney disease
About 📖
- Adult Polycystic Kidney Disease (ADPKD): A genetic disorder causing multiple fluid-filled cysts 🫧 in both kidneys.
- Accounts for ~10% of all end-stage renal failure (ESRF) cases 🩺.
- ~45% of affected individuals develop ESRF by age 60, with faster progression in males ♂️.
- Prevalence: ~1 in 750–1,000 individuals globally 🌍.
Aetiology 🧬
- Inheritance: Autosomal dominant (only one defective gene copy required).
- Genes:
- PKD1 (Chr 16): 85% of cases – more aggressive, earlier ESRF ⏳.
- PKD2 (Chr 4): 15% – milder, slower progression 🕰️.
- Proteins: Polycystin-1 & Polycystin-2 regulate tubular architecture & calcium signalling. Dysfunction → uncontrolled tubular proliferation & cyst growth.
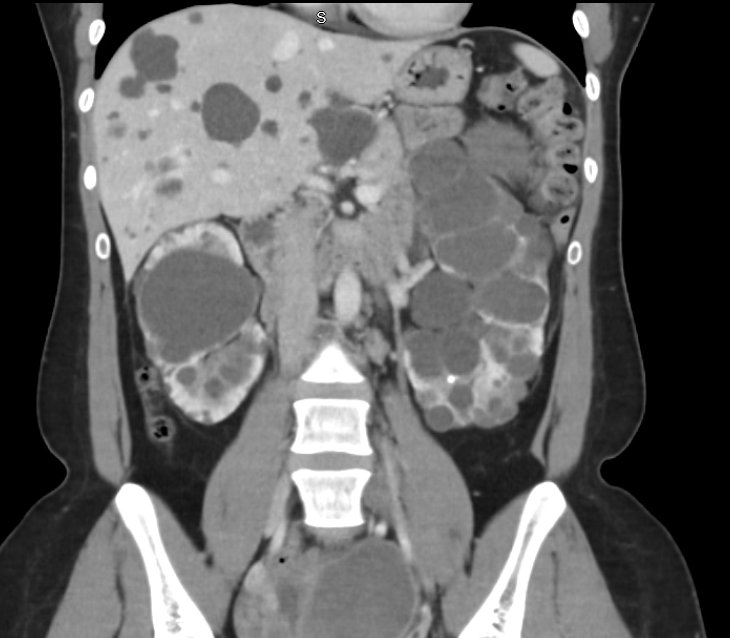
Pathology 🔬
- Proliferation of tubular epithelium → cyst formation → gradual compression of normal parenchyma.
- Cysts may also appear in the liver, pancreas, and spleen 🫀.
- Progressive loss of renal function → CKD and ESRF.
Clinical Features 🩺
- Family History: Key clue due to dominant inheritance 👨👩👧.
- Loin pain: Stretching of renal capsule or cyst haemorrhage.
- Haematuria: Frank or microscopic, often after cyst rupture 🚽.
- Hypertension: Severe, due to ↑ renin secretion 🩸.
- Renal stones: Especially urate or calcium oxalate 💎.
- Infections: Recurrent UTIs or cyst infections.
- Hepatic cysts: More common in women, usually asymptomatic.
- Berry aneurysms: Present in 5–10% → risk of subarachnoid haemorrhage 💥.
- Other associations: Diverticulosis, mitral valve prolapse, aortic root dilatation.
Screening 🔎
- Ultrasound from age >20 if family history is present 📡.
- MR angiography in those with family history of aneurysms 🧠.
Investigations 🧪
- Bloods: U&E (progressive ↑ creatinine), FBC (polycythaemia may occur from cyst erythropoietin production).
- Imaging: Renal USS (diagnostic if >3 cysts in each kidney after age 20). CT/MRI useful for complications.
- Screening for aneurysms: MR angiography if family history of SAH.
Management ⚕️
- No definitive cure – treatment targets complications & slowing progression.
- BP control: ACEIs/ARBs are first-line (slow CKD progression) 💊.
- ESRF: Dialysis or renal transplant (excellent outcomes in ADPKD).
- Pain: May require cyst decompression or nephrectomy if severe.
- Aneurysm risk: Screen and manage appropriately (e.g., neurosurgical referral).
- Genetic counselling: Essential for affected families 👨👩👦.
Key Clinical Pearls ✨
- Think ADPKD in young hypertensive patients with a family history of kidney disease 🩺.
- Loin pain + haematuria after minor trauma = possible cyst rupture.
- Berry aneurysms = most feared extra-renal complication 💥.
- ACEIs/ARBs slow progression – control BP aggressively 🫀.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
