| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Cardiac Troponins
Related Subjects: |Cardiac Troponins |Coronary Artery AP
Cardiac troponins (cTnI and cTnT) are structural proteins within the cardiac sarcomere and the preferred biomarkers for myocardial injury. High-sensitivity assays can detect very small amounts of myocardial cell injury, but troponin ≠ myocardial infarction: MI requires a troponin rise/fall plus clinical evidence of acute myocardial ischaemia (symptoms, ECG, imaging, or coronary thrombus).
🔬 What troponin is (structure & physiology)
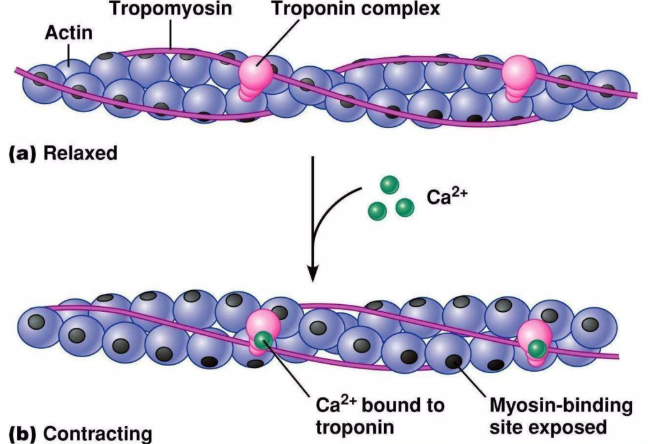
- Troponin complex sits on the thin filament (actin) with tropomyosin and regulates contraction.
- TnC binds calcium → conformational change → moves tropomyosin off actin’s myosin-binding sites → cross-bridge cycling starts.
- TnI is the inhibitory subunit (prevents actin–myosin interaction at rest).
- TnT anchors the complex to tropomyosin.
- Cardiac-specific isoforms of TnI/TnT allow blood tests to reflect cardiac myocyte injury rather than skeletal muscle damage.
🧪 High-sensitivity troponin (hs-cTn): why it changed practice
- hs-cTn assays detect low troponin concentrations with high analytical precision, enabling earlier rule-out/rule-in pathways in emergency care.
- Interpretation is assay-specific: always use your local lab’s reference ranges and pathway.
- Key concept: the clinically important threshold is the 99th percentile upper reference limit (URL) for that assay.
📌 Definitions you must get right
- Myocardial injury: any troponin value above the assay’s 99th percentile URL.
- Acute myocardial injury: myocardial injury with a rise and/or fall on serial testing (dynamic change).
- Myocardial infarction (MI): acute myocardial injury plus evidence of acute ischaemia (typical symptoms, new ischaemic ECG changes, imaging evidence, or coronary thrombus).
🩺 NICE / UK approach in practice (what you actually do in ED/AMU)
In the UK, NICE supports the use of high-sensitivity troponin testing within structured early rule-out/rule-in strategies for suspected ACS. Your hospital will implement an approved pathway (timings/cut-offs differ by assay), but the principles below stay the same.
- Always do an ECG early and treat STEMI as a time-critical emergency (troponin should not delay reperfusion).
- For possible NSTE-ACS, use hs-cTn with serial sampling when needed (especially if symptom onset is recent).
- If symptoms started very recently (e.g. within ~2 hours), a single troponin can be falsely low → repeat at an appropriate interval per local pathway.
- Discharge decisions should combine: symptoms (including ongoing pain), ECG, troponin pattern, and overall clinical risk (and safety-netting).
⏱️ Typical kinetics (teach the pattern, avoid overpromising)
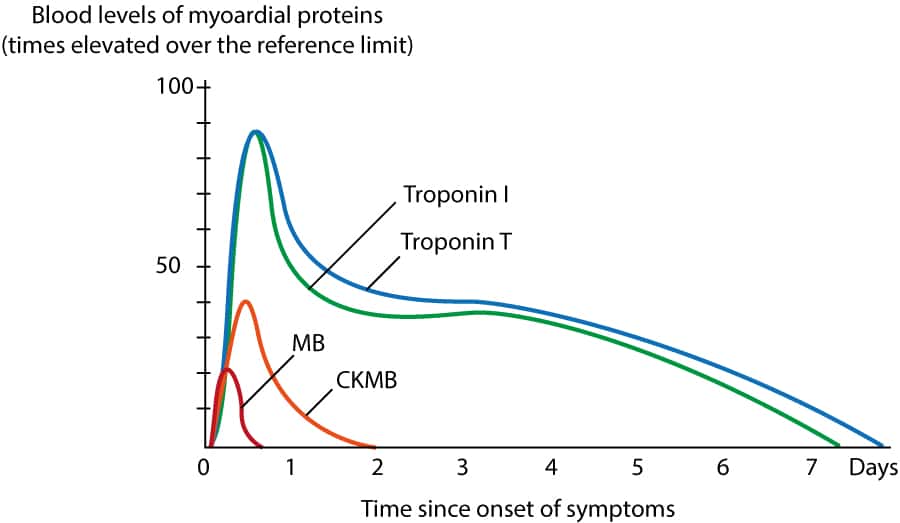
- With contemporary assays, troponin may rise within a few hours of injury; hs-cTn can detect injury earlier than older assays.
- Early presenters can have an initially normal troponin → serial testing is essential if clinical suspicion remains.
- Troponin can remain elevated for days after significant myocardial necrosis; the exact duration varies by infarct size and assay.
🧭 How to interpret a result (a practical framework)
- Step 1 — Is it above the 99th percentile URL?
- No: MI is unlikely, but not excluded in early presenters or ongoing ischaemia → repeat if indicated.
- Yes: myocardial injury is present → move to step 2.
- Step 2 — Is there a significant rise/fall on serial testing?
- Dynamic change: suggests acute injury (consider MI vs myocarditis vs tachyarrhythmia, etc.).
- Stable elevation: suggests chronic injury (e.g. structural heart disease, CKD) — still prognostically important.
- Step 3 — Is there evidence of acute ischaemia?
- If yes → MI (type 1 or type 2 depending on mechanism).
- If no → acute myocardial injury (non-MI) and treat the cause.
⚠️ Common causes of raised troponin (MI and non-MI)
- Type 1 MI (atherothrombosis): plaque rupture/erosion → coronary thrombosis.
- Type 2 MI (supply–demand mismatch): sepsis, tachyarrhythmia, severe anaemia, hypoxia, hypertensive crisis, coronary spasm, etc.
- Acute myocardial injury (non-ischaemic): myocarditis, acute heart failure, cardiotoxic drugs, post-procedure injury, cardiac contusion.
- Chronic myocardial injury: chronic heart failure, CKD, structural heart disease — often persistently elevated with little change.
🧠 Clinical “gotchas” (very exam- and ward-relevant)
- Renal impairment: baseline troponin may be chronically elevated; the trend and clinical picture are key.
- One troponin is rarely enough if the story suggests early ACS — use serial testing as per pathway.
- Troponin is prognostic even when it’s not MI — an elevated troponin flags higher risk and warrants careful assessment.
- STEMI: treat based on ECG/clinical picture; do not wait for troponin before activating the pathway.
✅ Summary
Troponin tells you “myocardial injury happened”. To diagnose myocardial infarction you need a rise/fall above the 99th percentile URL plus evidence of acute myocardial ischaemia. In UK practice, NICE supports hs-cTn within structured early rule-out strategies — always follow your local lab’s assay-specific cut-offs and timings, and interpret results in the clinical context.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
