| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Cervical Cancer screening
Related Subjects: |Causes of abnormal Vaginal bleeding |Vaginal Carcinoma |Cervical cancer |Cervical cancer screening |Antepartum haemorrhage |Trauma: Traumatic Brain Head Injury (TBI) |Post Menopausal Bleeding |Postpartum haemorrhage
🧪 Cervical Cancer Screening helps detect precancerous changes early, allowing treatment before progression to invasive cancer. It involves sampling cells from the cervix and analysing them for abnormalities. Early detection → better outcomes ✅
📌 About
- Cells collected from the ectocervix using a spatula or brush.
- Sample placed on a glass slide or in liquid-based cytology medium → stained & examined in the lab.
- Goal: Detect precancerous lesions early → prevent progression to cervical cancer.
📅 Screening Guidelines (UK)
- 👩 Women aged 25–49 years: Invited every 3 years.
- 👩🦳 Women aged 50–64 years: Invited every 5 years.
- Women >65: Only screened if not tested since 50 or if recent abnormal results.
- Screening may be modified if high risk (e.g., HIV, immunosuppression).
🧾 Pap Smear Results
- Mild Dyskaryosis: Often due to transient HPV infection; usually low risk.
- Moderate Dyskaryosis: More significant abnormalities; likely CIN 2/3.
- Severe Dyskaryosis: High-grade abnormality → high risk of progression to cancer.
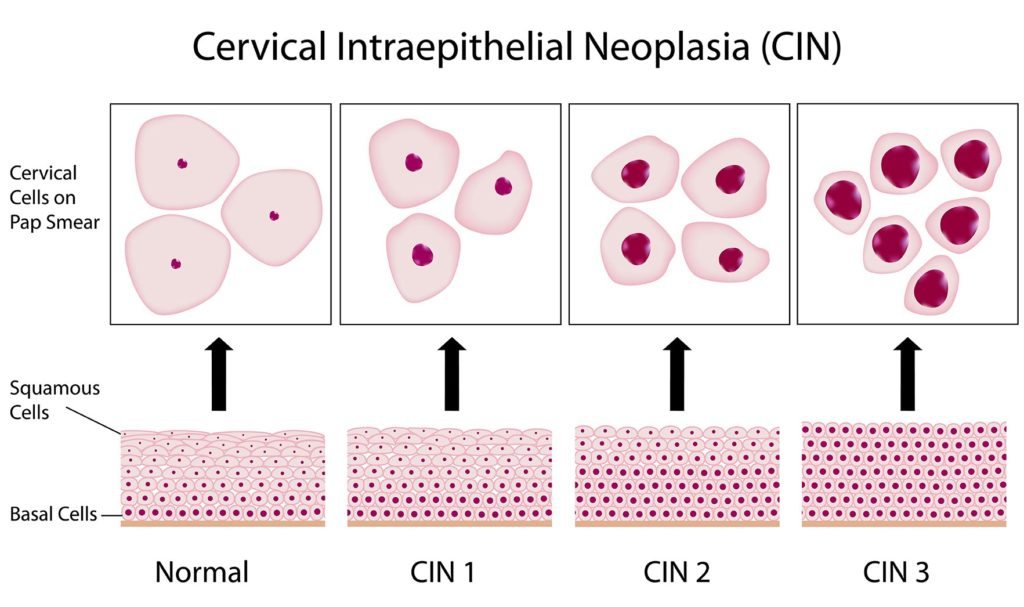
🔬 Cervical Intraepithelial Neoplasia (CIN)
- CIN 1: Abnormal cells in lower third of epithelium → low-grade; many regress spontaneously.
- CIN 2: Abnormal cells in two-thirds of epithelium → high-grade; usually needs treatment.
- CIN 3: Abnormal cells throughout full epithelial thickness → high risk; requires treatment.
⚡ Actions Based on Results
- Mild dyskaryosis / CIN 1: Repeat smear in 6–12 months or colposcopy referral.
- Moderate dyskaryosis / CIN 2: Refer for colposcopy + likely treatment.
- Severe dyskaryosis / CIN 3: Urgent colposcopy + excisional treatment (e.g. LLETZ).
🩺 Management of Precancerous Changes
- Colposcopy: Magnified cervix examination ± biopsy; treatment includes laser ablation, cold coagulation, or cryotherapy.
- LLETZ / Cone biopsy: Removes transformation zone containing abnormal cells. 🔑 Cone biopsy reserved for glandular disease or unclear margins.
- Follow-up: Repeat smear/HPV test at 6 months → ensure clearance.
ℹ️ General Management Notes
- Benign findings (e.g., metaplasia, atrophic smear) → no action.
- Inflammatory changes → test for infections (e.g., chlamydia, candida, bacterial vaginosis).
- Actinomyces on smear with IUCD → consider IUCD removal + gynae review.
- Glandular neoplasia: Always urgent referral (risk of adenocarcinoma).
📚 References
- NICE Cervical Cancer Screening Guidelines (2013)
- RCOG Green-top Guideline No. 31 (2016)
- BSCCP Colposcopy & Treatment Guidelines (2019)
- Smith JS et al. HPV and Cervical Cancer. Lancet 2007.
- Castle PE et al. Evidence Review of Screening. Int J Cancer 2013.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
