| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Anatomy and Physiology of the Ovary
Related Subjects: |Causes of abnormal Vaginal bleeding |Vaginal Carcinoma |Cervical cancer |Endometrial (Uterine) Cancer |Post Menopausal Bleeding |AP of the Uterus and Fallopian Tubes |AP of the Ovary |Gynaecological History Taking |Colposcopy |Premature Menopause |Polycystic Ovary syndrome
🌸 Roles
- Endocrine function: Production of steroid hormones - oestrogen, progesterone, and androgens.
- Reproductive function: Gametogenesis (development and release of oocytes).
🔬 Gross Anatomy
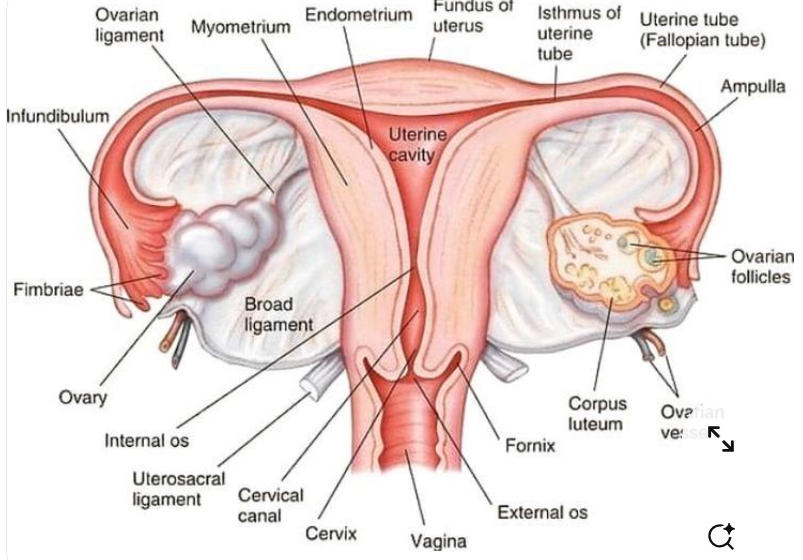
- Paired almond-shaped organs located on either side of the uterus in the lateral pelvic wall.
- Average size in reproductive years: 4 × 3 × 2 cm; weight approximately 8–10 g.
- Lie close to the fimbrial end of the fallopian tubes, facilitating oocyte capture at ovulation.
- Attached to the posterior layer of the broad ligament by the mesovarium, a peritoneal fold carrying vessels, lymphatics, and nerves.
- Suspended laterally by the suspensory ligament of the ovary (infundibulopelvic ligament), which contains the ovarian vessels.
- Medially attached to the uterus via the ovarian ligament.
🩸 Blood Supply and Drainage
- Arterial supply: Ovarian arteries arise directly from the abdominal aorta just below the renal arteries.
- Additional contribution from the uterine artery (anastomotic supply).
- Venous drainage: Ovarian veins form the pampiniform plexus; right drains into the IVC, left drains into the left renal vein.
- Lymphatic drainage: Para-aortic (lumbar) lymph nodes.
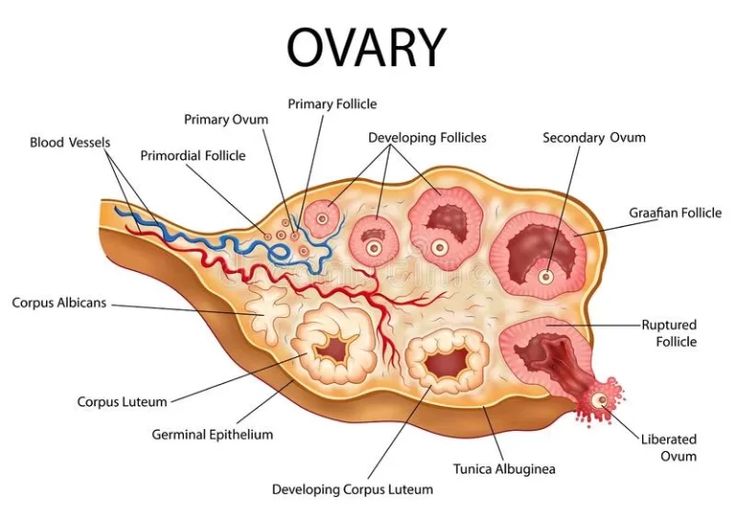
🏗️ Microscopic Structure
- Outer cortex: Contains follicles at various stages of development embedded in a dense stromal matrix.
- Inner medulla: Looser connective tissue containing blood vessels, lymphatics, and nerves.
- Surface covered by a single layer of cuboidal epithelium (historically termed “germinal epithelium”).
- Underlying dense fibrous capsule called the tunica albuginea.
- Primordial oocytes supported by stromal connective tissue and follicular cells.
🔄 Physiology: Follicular Development and Ovulation
- At menarche, approximately 400,000–500,000 primordial follicles remain in the ovarian cortex.
- Primordial follicles (~0.1 mm) consist of an oocyte surrounded by a single layer of granulosa cells.
- Granulosa cells produce oestradiol (via aromatisation of theca-derived androgens).
- Stromal cells differentiate into:
- Theca interna: Androgen-producing layer (LH-responsive).
- Theca externa: Structural layer with no endocrine function.
- During each menstrual cycle, multiple follicles are recruited under FSH influence, but usually one dominant follicle develops into a mature Graafian follicle.
- The mature follicle reaches ~20 mm in diameter before ovulation.
- The LH surge triggers completion of meiosis I:
- Primary oocyte (46 chromosomes) divides.
- Produces a secondary oocyte and first polar body (each haploid - 23 chromosomes).
- Ovulation releases the secondary oocyte into the peritoneal cavity, usually captured by the fimbriae of the fallopian tube.
🌕 Corpus Luteum Formation
- After ovulation, the ruptured follicle collapses.
- Granulosa cells become granulosa lutein cells.
- Theca interna becomes theca lutein cells.
- Forms the corpus luteum, visible as a yellow, crinkled structure.
- Secretes progesterone and oestrogen to support endometrial preparation.
- If no fertilisation:
- Degenerates after ~10–14 days.
- Forms a fibrotic scar - the corpus albicans.
- If pregnancy occurs:
- Corpus luteum enlarges (up to 3 cm).
- Persists for 8–12 weeks under hCG stimulation before placental takeover.
🥚 Oocyte Numbers Across the Lifespan
- ~7 million primordial germ cells at 15 weeks’ gestation.
- ~2 million at birth.
- ~400,000–500,000 at puberty.
- Approximately 400–500 ovulated during reproductive life.
- Remaining follicles undergo atresia.
🧠 Key Physiological Concepts
- Follicular development is regulated by the hypothalamic–pituitary–ovarian axis (GnRH → FSH/LH → ovarian hormones).
- Ovarian steroid production operates via the two-cell, two-gonadotropin model (LH stimulates theca → androgens; FSH stimulates granulosa → aromatisation to oestrogen).
- Menopause results from depletion of functional follicles, leading to reduced oestrogen and loss of negative feedback on FSH/LH.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
