| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Ankle-Brachial Pressure Index (OSCE focused)
Related Subjects: | Vascular Surgery: Introduction | Ankle-Brachial Pressure Index (ABPI) | Peripheral Arterial Disease (PAD) | Abdominal Aortic Aneurysm (AAA) | Carotid Endarterectomy | Buerger's disease (Thromboangiitis obliterans) | Leriche syndrome (aortoiliac occlusive disease)
🦵 Ankle–Brachial Pressure Index (ABPI) - OSCE + clinic-ready
🧠 What ABPI actually measures: ABPI is a pressure ratio (ankle systolic ÷ arm systolic). In healthy arteries, ankle systolic pressure is usually similar to (or slightly higher than) brachial pressure. With a haemodynamically significant stenosis, pressure drops distal to the lesion, so the ankle pressure falls and ABPI decreases. If arteries are calcified and incompressible (e.g., diabetes/CKD), the cuff can’t occlude the vessel properly and ABPI can be falsely high - that’s when you pivot to toe pressures/toe–brachial index (TBI). :contentReference[oaicite:0]{index=0}
✅ When to do ABPI (high-yield indications)
- 🚶 Suspected PAD: intermittent claudication, rest pain, cold/pale foot, absent pulses.
- 🩹 Leg ulcer assessment before compression (venous vs mixed vs arterial).
- 🧦 Deciding whether compression therapy is safe and what strength to use.
- 🧠 Cardiovascular risk flag: PAD = high systemic atherosclerotic risk (think heart + brain as well as legs).
⚠️ When ABPI is unreliable / use caution
- 🪨 ABPI ≥ 1.3–1.4: suggests calcified/incompressible arteries → consider TBI, toe pressures, duplex. :contentReference[oaicite:1]{index=1}
- 🩸 Marked oedema, very painful wounds, severe tremor → may distort readings (technique + cuff fit matter).
- 🫀 Arrhythmias (e.g., AF) → repeat measures and average; be extra careful with technique.
- 🧠 If critical limb ischaemia/acute limb ischaemia suspected: don’t let ABPI delay urgent vascular escalation.
🧰 Equipment
- 🩺 BP cuffs (correct size!) + manual sphygmomanometer
- 📣 Handheld Doppler (commonly 5–8 MHz)
- 🧴 Gel, paper, pen (and a calm helper if you’re teaching!)
📝 Step-by-step method (Doppler ABPI)
| Step | What you do (OSCE phrasing) | Why it matters |
|---|---|---|
| 1 🛏️ Rest | Ask the patient to lie supine and rest ~10 minutes. Legs flat, not dangling. | Standardises haemodynamics (posture changes ankle pressure). |
| 2 💪 Brachial pressures | Measure systolic pressure in both arms (Doppler or standard). Record both. Use the higher brachial systolic for calculations (unless subclavian stenosis suspected-see pitfalls). | Using the higher arm pressure avoids over-diagnosing PAD and improves accuracy. |
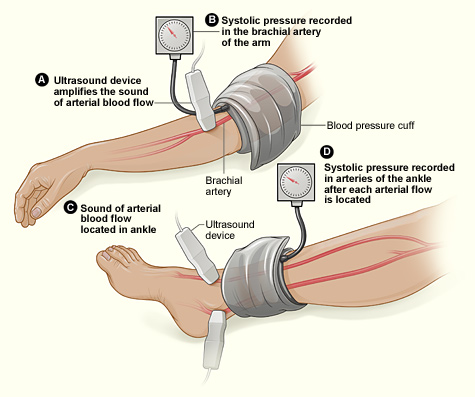
| 3 🦶 Locate ankle arteries | With Doppler + gel, find signals at dorsalis pedis and posterior tibial arteries. | You’ll measure both and use the higher ankle pressure (per leg). |
| 4 🎯 Measure ankle systolic | Place cuff just above malleoli. Inflate until Doppler signal disappears, then deflate slowly; record the pressure when signal returns = systolic. Repeat for DP and PT. | Detects the pressure distal to any stenosis; Doppler improves detection, especially in low-flow states. |
| 5 ➗ Calculate (each leg) | ABPI (Right) = highest ankle systolic (DP or PT) ÷ highest brachial systolic. Repeat for left. | This “highest ankle ÷ highest arm” method is widely recommended for accuracy. |
| 6 🧾 Document & interpret | Record: DP/PT pressures, brachials, ABPI both legs, symptoms, pulse findings, and what you’ll do next. | ABPI guides compression decisions and vascular referral urgency. |
🧮 Worked example:
Right ankle: DP 92 mmHg, PT 104 mmHg → highest ankle = 104
Brachials: R 128, L 136 mmHg → highest brachial = 136
✅ Right ABPI = 104 ÷ 136 = 0.76 → moderate PAD / mixed disease likely (compression decisions depend on ulcer context + local pathway).
📊 ABPI interpretation
| Resting ABPI | Likely interpretation | Clinical correlation |
|---|---|---|
| > 1.3 | Suggests arterial calcification / incompressible vessels | Common in diabetes, CKD, RA/vasculitis → ABPI may be unreliable |
| 0.8 – 1.3 | No evidence of significant PAD | Compression stockings generally safe (if no other contraindications) |
| 0.5 – 0.8 | Moderate PAD | Often intermittent claudication; optimise risk factors + consider imaging if severe symptoms |
| < 0.5 | Severe ischaemia | Often critical ischaemia/rest pain or tissue loss → urgent vascular input |
🧦 ABPI and compression therapy (leg ulcer context)
⚠️ Never apply compression to a new/non-healing lower leg wound until ABPI + full lower limb assessment has been done. :contentReference[oaicite:8]{index=8}
| ABPI | Compression guidance (typical UK community pathways) | Notes |
|---|---|---|
| 0.8–1.3 | ✅ Often suitable for full compression (if venous ulcer pattern) | Still interpret in clinical context; mixed disease can exist. :contentReference[oaicite:9]{index=9} |
| 0.65–0.79 | 🟠 Often reduced compression (mixed aetiology likely) | Consider tissue viability/vascular input. :contentReference[oaicite:10]{index=10} |
| < 0.64 | 🚫 Avoid high compression; refer per pathway | Escalate-arterial component significant. :contentReference[oaicite:11]{index=11} |
| < 0.5 | 🚨 Urgent vascular referral | Severe PAD likely; compression risks ischaemic injury. :contentReference[oaicite:12]{index=12} |
🧠 Common pitfalls (things examiners love)
- 📏 Wrong cuff size → false readings (too small cuff overestimates pressure).
- 🧍 Not resting supine → ankle pressures can be artificially high/variable.
- 💪 Only measuring one arm: you can miss a higher brachial pressure (or miss subclavian disease).
- 🪨 Falsely high ABPI in diabetes/CKD/elderly due to calcification → use TBI. :contentReference[oaicite:13]{index=13}
- 🚶 Symptoms with normal resting ABPI: consider exercise ABPI for claudication work-up. :contentReference[oaicite:14]{index=14}
🗣️ OSCE mini-script (30–45 seconds)
- 👋 “I’m going to measure the ankle–brachial pressure index to assess arterial perfusion and help guide safe management (including whether compression is appropriate).”
- 🛏️ “I’ll ask you to lie flat and rest, then measure blood pressure in both arms, then measure ankle pressures using a Doppler over dorsalis pedis and posterior tibial arteries.”
- ➗ “ABPI is the highest ankle systolic pressure divided by the highest brachial systolic pressure, calculated for each leg.”
- 🧾 “I’ll document values, interpret them with the clinical picture, and escalate urgently if severe arterial disease is suspected.”
📚 References (UK + core)
- Wounds UK / Wound Essentials: ABPI measurement and interpretation; cautions for compression; calcification/high ABPI discussion. :contentReference[oaicite:15]{index=15}
- Remedy BNSSG ICB: community leg ulcer assessment and ABPI thresholds guiding compression/referral. :contentReference[oaicite:16]{index=16}
- American Heart Association / American College of Cardiology PAD guidance: ABI <0.90 for PAD; ABI >1.40 suggests incompressible arteries; exercise ABI and TBI use. :contentReference[oaicite:17]{index=17}
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
