| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Toxoplasmosis
Related Subjects: |Herpes Varicella-Zoster (Shingles) Infection |Chickenpox Varicella Infection |Varicella Cerebral Vasculopathy |Herpes Viruses |Herpes Zoster Ophthalmicus (HZO) Shingles |MonkeyPox |Mumps |Measles |Rubella (German Measles) |Epstein-Barr Virus infection |Cytomegalovirus (CMV) infections |CMV retinitis infections |Toxoplasmosis
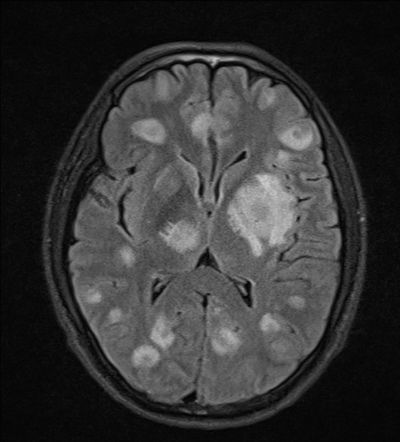
🧠 Causes focal CNS lesions and encephalopathy best seen on MRI, which improve with treatment.
📖 About
- 🦠 Toxoplasmosis is an intracellular protozoan infection caused by Toxoplasma gondii.
- 🇬🇧 About 22% of the UK population are seropositive; 🇫🇷 >90% of the French population are seropositive.
- 🔬 T. gondii was first discovered in 1908 by Charles Nicolle & L. Manceaux in a North African rodent (Ctenodactylus gondii).
🌍 Source
- Foodborne: 🍖 Raw or undercooked meat.
- Zoonotic: 🐱 Cats, 🐦 birds, and contaminated soil.
- Congenital: 👶 Passed from mother to fetus.
- Other: 💉 Blood transfusion.
⚠️ Risks
- 🤰 Pregnancy → high risk to the fetus.
- 🧑⚕️ HIV/AIDS → ~10% of untreated AIDS patients (esp. CD4 <100/mm³).
- 💊 Immunosuppressive therapy → transplant & oncology patients at risk.
🩺 Clinical Presentation (varies with immune status & gestation)
- 🦠 Lymphadenopathy: Cervical nodes, glandular fever–like, often asymptomatic.
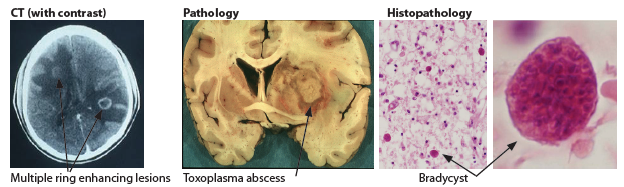
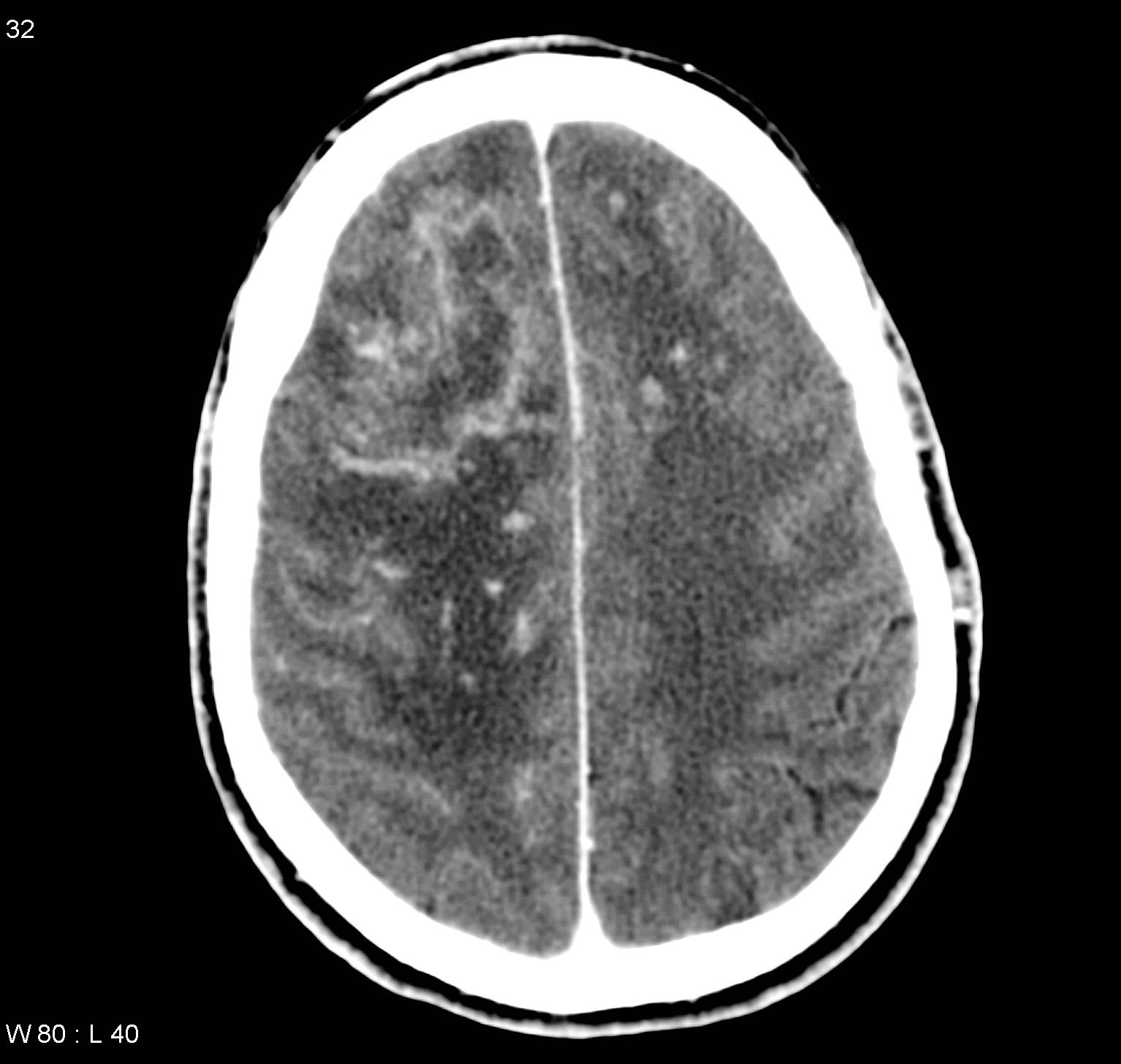
- 🧠 Toxoplasmic Encephalitis: Fever, headache, seizures, focal deficits (esp. HIV-positive).
- 👶 Congenital Toxoplasmosis: Microcephaly, hydrocephalus, chorioretinitis, intellectual disability.
- 🌡️ Systemic Toxoplasmosis: Pneumonia, myocarditis, hepatitis (rare if immunocompetent).
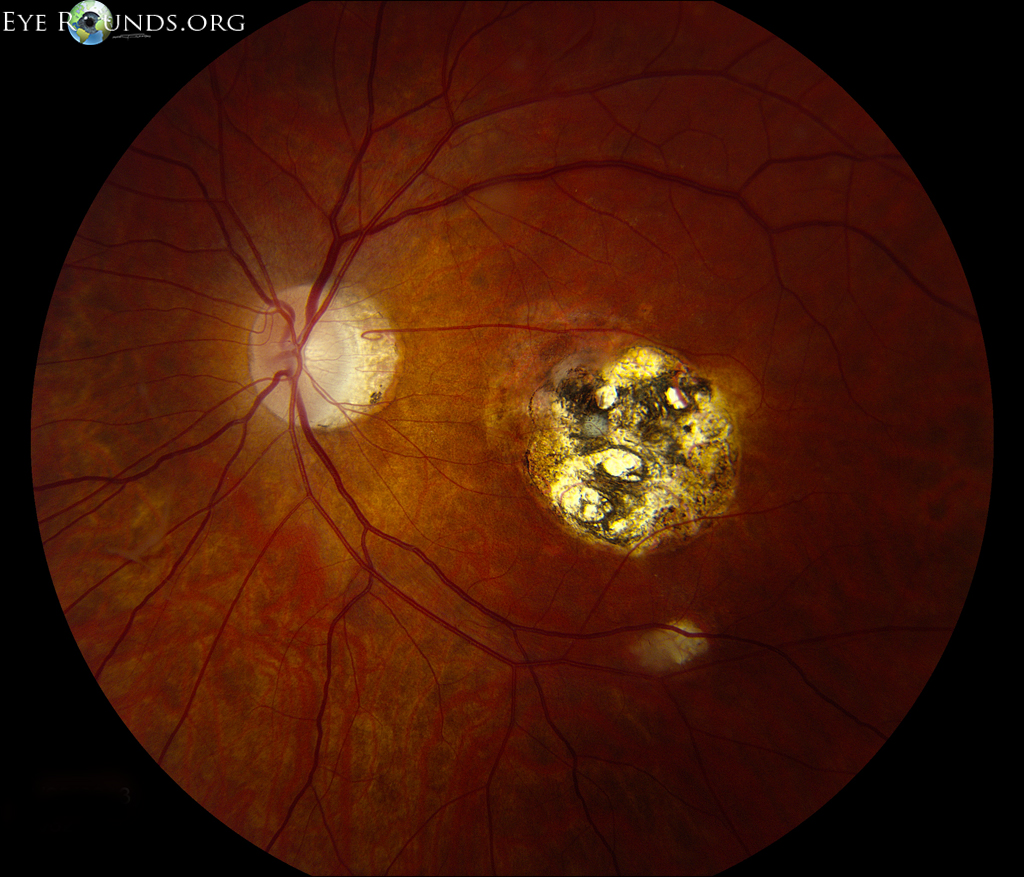
- 👁️ Ocular Toxoplasmosis: Retinochoroiditis → eye pain, visual loss.
🔎 Investigations
- Serology: 🧪 Sabin–Feldman test, rising IgG or IgM.
- HIV Testing: Check if immunocompromised.
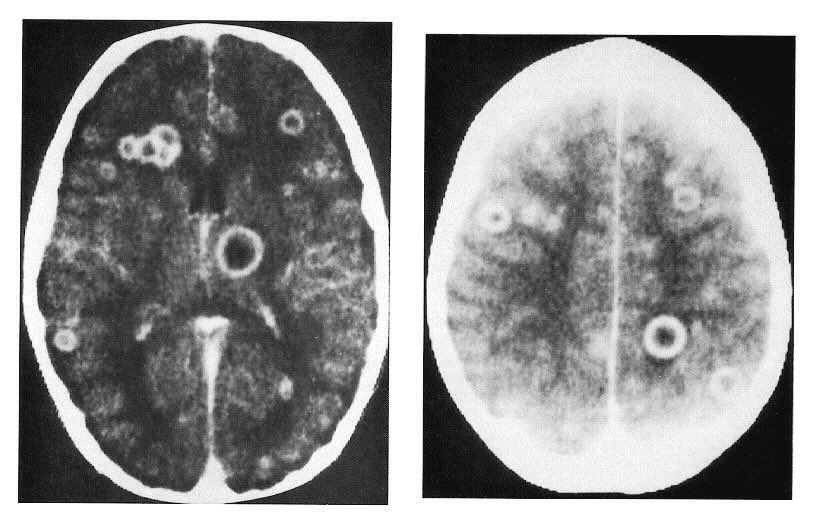
- Imaging: MRI/CT → multiple ring-enhancing brain lesions (vs single lesion in CNS lymphoma).
- Pulmonary Assessment: CXR/CT for PCP-like pneumonitis.
📑 Diagnostic Criteria
- 🔄 Positive IgG seroconversion.
- 🧪 Specific IgA/IgM + low-avidity IgG (<20%).
- 🧬 Histology: epithelioid cells, follicular hyperplasia.
- 🧫 Parasite detection via PCR or culture.
💊 Management
- 🙂 Asymptomatic (immunocompetent, nonpregnant): No treatment needed.
- 🤒 Symptomatic or Immunocompromised: Sulfadiazine + Pyrimethamine × 6 weeks + MRI monitoring.
- 🧑⚕️ HIV Patients: Start HAART once stable (watch for IRIS).
- 🔍 If no improvement within 3 weeks → reconsider Dx (e.g., CNS lymphoma, tuberculoma).
📚 References
Cases - Toxoplasmosis
- Case 1 - Congenital toxoplasmosis 👶: A 26-year-old woman with cats at home eats undercooked lamb during pregnancy. At 22 weeks, ultrasound shows ventriculomegaly and intracranial calcifications. The newborn has chorioretinitis, hydrocephalus, and seizures. Diagnosis: classic triad of congenital toxoplasmosis. Managed with maternal spiramycin in pregnancy, and pyrimethamine–sulfadiazine plus folinic acid after birth.
- Case 2 - Immunocompromised host 🧬: A 42-year-old man with advanced HIV (CD4 <100) presents with fever, confusion, and focal seizures. MRI brain: multiple ring-enhancing lesions with surrounding oedema. Toxoplasma IgG positive. Diagnosis: cerebral toxoplasmosis. Managed with high-dose pyrimethamine, sulfadiazine, and folinic acid, plus ART optimisation.
- Case 3 - Acquired infection in immunocompetent adult 🥩: A 30-year-old woman presents with low-grade fever, malaise, and cervical lymphadenopathy 2 weeks after eating rare steak. Serology: Toxoplasma IgM positive, IgG rising on repeat. Diagnosis: acquired toxoplasmosis (self-limiting in immunocompetent). Managed with supportive care only.
Teaching Point 🩺: Toxoplasmosis is caused by *Toxoplasma gondii* (cats = definitive host). - In pregnancy: risk of congenital infection → hydrocephalus, intracranial calcifications, chorioretinitis. - In immunocompromised patients: reactivation causes cerebral abscesses. - In healthy adults: often mild, with flu-like illness and lymphadenopathy. Prevention: avoid undercooked meat, wash vegetables, and avoid cat litter in pregnancy.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
