| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Epilepsy - Idiopathic Generalised Epilepsy
Related Subjects: |Status Epilepticus (Epilepsy) |Coma management |Lorazepam |Phenytoin |Levetiracetam |Epilepsy - General Management |First Seizure |Epilepsy in Pregnancy |Febrile seizures
⚡ Idiopathic Generalised Epilepsy (IGE) is a group of epilepsy syndromes characterised by generalised seizures, normal neuroimaging, and a presumed genetic basis. It accounts for ~15–20% of all epilepsies and typically presents in childhood or adolescence.
🔎 About
- IGE is also called “genetic generalised epilepsy” (GGE) in newer classifications.
- Onset is usually in childhood or adolescence, often between ages 5–20.
- Patients have normal neurological examination and normal neuroimaging.
- There is often a family history of seizures or epilepsy.
🧬 Pathophysiology
- Thought to result from genetic predisposition affecting neuronal excitability and cortical network synchronisation.
- Involves abnormal thalamocortical oscillations → generalised 3 Hz spike-and-wave discharges.
- No structural brain abnormality on MRI (distinguishes it from focal epilepsies).
🩺 Clinical Syndromes under IGE
- Childhood Absence Epilepsy (CAE) – Onset: 4–10 years. – Frequent absence (“blank”) seizures, often unnoticed at first. – EEG: 3 Hz spike-and-wave discharges.
- Juvenile Absence Epilepsy (JAE) – Onset: 10–16 years. – Absences less frequent than CAE, but generalised tonic–clonic seizures common.
- Juvenile Myoclonic Epilepsy (JME) – Onset: adolescence (12–18 years). – Myoclonic jerks in the morning (“I keep dropping things at breakfast ☕”). – Often associated with tonic–clonic seizures.
- Generalised Tonic–Clonic Seizures Alone (GTCSa) – Onset: adolescence. – No absences/myoclonus, just generalised tonic–clonic seizures.
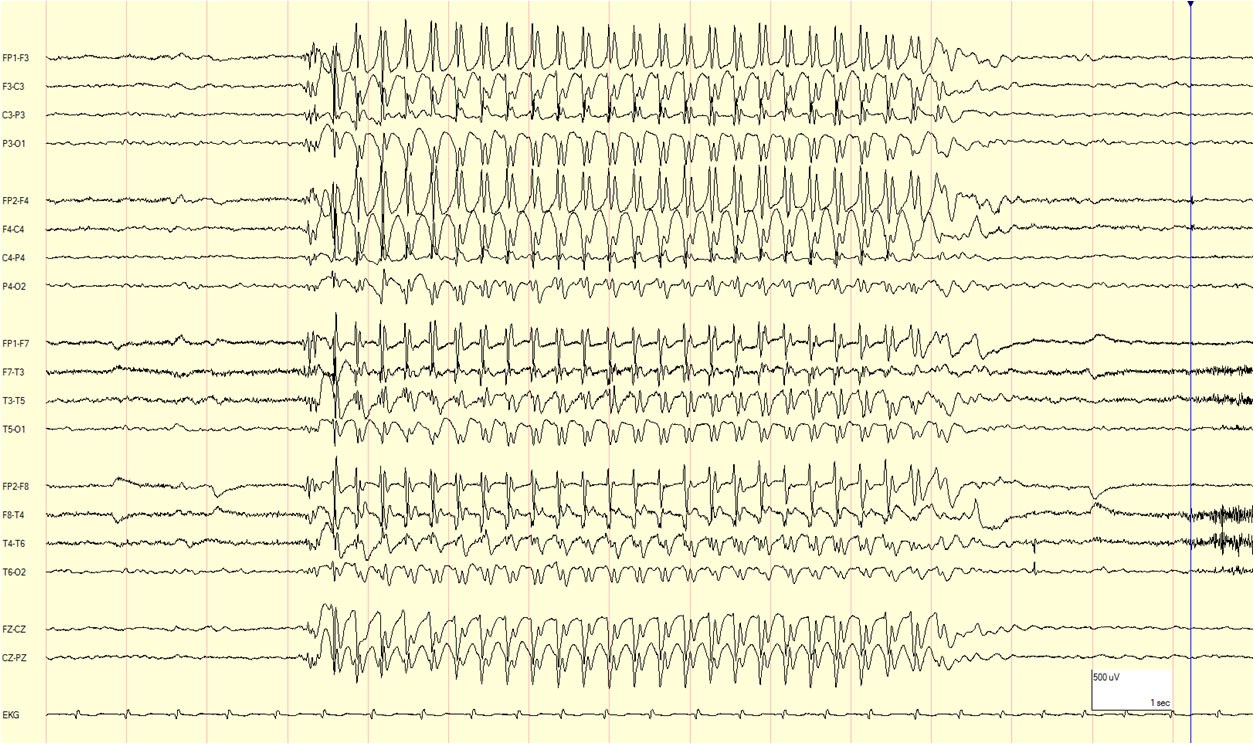
Example of 3Hz generalized spike-wave seen on the ictal EEG
📊 Risk Factors / Triggers
- Sleep deprivation 🛌.
- Alcohol, especially binge drinking 🍺.
- Photosensitivity (flashing lights, screens) 💡.
- Stress, illness, hormonal changes.
🧪 Investigations
- EEG: hallmark = generalised 3 Hz spike-and-wave (absences) or polyspike-and-wave (JME).
- Neuroimaging (MRI): Normal – helps exclude structural causes.
- Bloods: To rule out metabolic triggers (glucose, electrolytes, calcium, magnesium).
- History: Careful witness account; absence seizures often misdiagnosed as daydreaming.
💊 Management
- First-line AEDs: – Sodium valproate (⚠️ avoid in women of childbearing age due to teratogenicity, neurodevelopmental risk). – Alternatives: Levetiracetam, Lamotrigine (slightly less effective in JME but safer in women).
- Lifestyle: Sleep hygiene, avoid alcohol binges, stress management, photosensitivity precautions.
- Driving: Must be seizure-free for at least 12 months before driving (DVLA rules, UK).
- Counselling: Important to explain precipitating factors and need for adherence.
⚠️ Drugs to Avoid
- Carbamazepine and phenytoin may worsen generalised seizures in IGE.
- Gabapentin and tiagabine are not effective.
📚 Prognosis
- Generally good with treatment – many achieve remission, though some require lifelong AEDs.
- Absence epilepsy often resolves by adolescence.
- Juvenile myoclonic epilepsy tends to persist into adulthood (lifelong tendency).
📌 Exam Pearls
- IGE = normal neuro exam + normal MRI + abnormal EEG (generalised discharges).
- Morning myoclonus in a teenager = Juvenile Myoclonic Epilepsy.
- Child who “daydreams” with 3 Hz spike-wave = Childhood Absence Epilepsy.
- Avoid carbamazepine → may exacerbate seizures.
- Valproate most effective, but avoid in women of childbearing age 🚫🤰.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
