| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Chest drain Insertion
🫁 Chest drain insertion = life-saving procedure for draining air (pneumothorax) or fluid (haemothorax, effusion) from the pleural space. ⚠️ Wait for a chest X-ray in most cases, except when tension pneumothorax is strongly suspected → immediate decompression.
🛡️ Precautions
- Only competent staff (or trainees under direct supervision) should perform.
- Strict aseptic technique to minimise infection risk.
⛔ Contraindications
- Coagulopathy → correct if possible, but not an absolute contraindication (drains can be life-saving).
- Always weigh risk vs benefit in unstable patients.
📍 Absolute Indications
- 🚨 Tension pneumothorax
- 🩸 Haemothorax
- 💔 Traumatic arrest (bilateral drains)
📍 Relative Indications
- Pneumothorax with underlying lung disease or failing conservative management.
- Rib fractures + positive pressure ventilation.
- Profound hypoxia/hypotension + unilateral chest signs (esp. penetrating trauma).
- Large haemothorax detected on FAST ultrasound.
👨⚕️ Teaching pearl: In trauma, if in doubt and the patient is in extremis, insert the chest drain without waiting for imaging.
🧰 Equipment
- Sterile gown + gloves, antiseptic solution, drapes.
- 1% lidocaine for local anaesthesia.
- Scalpel, suture (1/0 or 2/0 silk), blunt dissection clamp/forceps.
- Appropriate size chest tube + underwater seal drainage system (or flutter valve).
- Guidewire + dilators if using Seldinger technique.
📏 Chest Drain Size
- 🌬️ Pneumothorax → small-bore (8–14 Fr) effective, even in ventilated patients.
- 🩸 Haemothorax / trauma → larger bore (24–32 Fr) to avoid clot blockage.
- 💊 Pleurodesis → ≥12 Fr for adequate slurry drainage.
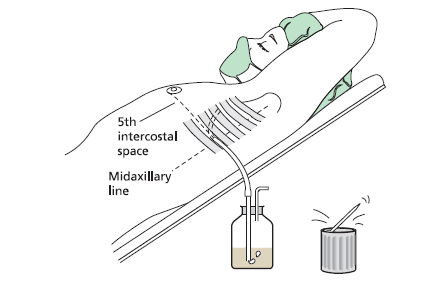
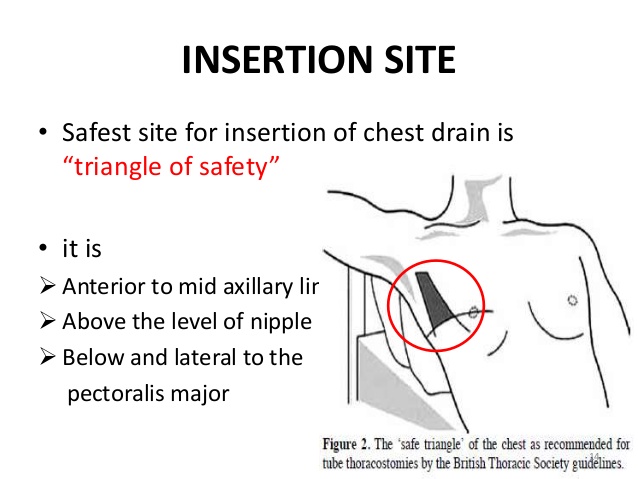
📍 Site of Insertion
- Safe triangle: bounded by anterior border of lat dorsi, lateral border of pec major, line above nipple (5th intercostal space).
- A practical tip: “last axillary hair” often overlies the safe site.
- ⚠️ Always incise just above a rib to avoid the neurovascular bundle.
🪛 Insertion Technique
- Consent, wash hands, gown, drape.
- Infiltrate local anaesthetic (10–20 ml lidocaine) down to pleura → aspirate to confirm position.
- Traditional blunt dissection:
- 2 cm incision above rib → blunt dissect with clamp → enter pleural space.
- Insert finger → confirm entry, break adhesions.
- Pass drain with clamp into pleural cavity → connect to underwater seal.
- Seldinger technique (less traumatic): needle → guidewire → dilator → drain over wire.
- Suture drain in place, U-stitch for removal, confirm with chest X-ray.
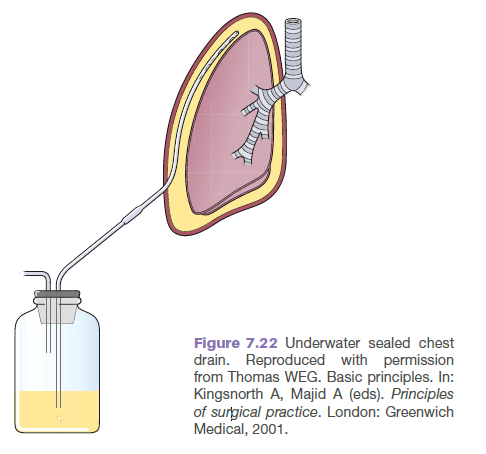
💧 Drainage Systems
- Simple underwater seal = one-way valve for air/fluid escape.
- Flutter valve (Heimlich) = alternative in some trauma/ambulatory cases.
📈 Monitoring
- Chest X-ray post-procedure to confirm placement.
- ⚠️ Large effusions → limit drainage (~1 L initially) to prevent re-expansion pulmonary oedema (clamp for 1 hr after 1 L).
- Suction (–10 to –20 cmH₂O) may be used if non-resolving pneumothorax or following pleurodesis.
- Non-swinging tube = consider blockage, misplacement, or completion of role.
🗑️ Removal
- Remove once indication resolved + no air leak/ongoing drainage.
- Controversial: clamping for 4–6 hrs pre-removal to check for air leak.
- Removal technique: cut suture, Valsalva manoeuvre, withdraw tube, close with mattress suture, apply gauze.
⚠️ Acute Complications
- Intercostal vessel laceration → haemothorax.
- Lung laceration (esp. adhesions).
- Diaphragm/abdominal penetration (too low).
- Stomach/colon injury (unrecognised hernia).
- Subcutaneous placement or too deep insertion.
- Tube dislodgement if poorly secured.
⚠️ Late Complications
- Blocked tube (clots, kinking).
- Retained haemothorax.
- Empyema.
- Recurrent pneumothorax post-removal (poor technique).
📚 References
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
