| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Cardiology Examination (OSCE)
Related Subjects: |Breast Anatomy and Examination (OSCE) |Shoulder examination(OSCE) |Testicular examination(OSCE) |Hernia Examination (OSCE) |Rectal examination (OSCE) |Liver Examination (OSCE) |Cerebellar Examination (OSCE) |Upper and Lower Limb Neurology (OSCE) |Gastroenterology Examination (OSCE) |Respiratory Examination (OSCE) |Cardiology Examination (OSCE) |OSCE Eye Exam |OSCE Ear Exam |OSCE Abdominal Exam |OSCE Ascites Exam |OSCE Jaundice Exam |OSCE Testicular Exam |OSCE Inguinal Exam |OSCE Upper limb Neurology |OSCE Lower limb Neurology |OSCE Face Neurology |OSCE Visual Fields
🔍 The cardiac exam is an active, hypothesis-driven process - look, think, correlate, and integrate findings systematically. Goal: Identify structural/functional abnormalities, assess severity, and formulate a differential diagnosis. Always verbalise steps, explain to the patient, and finish by stating how you’d complete the exam (BP both arms, fundoscopy, urine dip, ECG, echo, CXR).
🫀 Overall Structured Plan (High-Yield Sequence)
- 🧼 Wash hands, 👋 introduce yourself, ✅ confirm ID (name/DOB), 📝 explain exam, obtain consent, offer chaperone.
- 🛏️ Position: 45° semi-recumbent (adjust pillow for comfort), expose chest to waist (preserve dignity with towel/blanket).
- 👀 General inspection (end-of-bed): patient appearance, distress, cyanosis, pallor, cachexia, respiratory effort.
- Environment clues: O₂, GTN spray, IV fluids, ECG leads, drains, mobility aids, fluid charts, sputum pot.
- ✋ Hands & upper limbs → pulses → face & neck → chest inspection → palpation → auscultation → manoeuvres → peripheral signs → closure.
1️⃣ General Inspection (End of Bed) 👀
- Patient: dyspnoea at rest, orthopnoea (extra pillows), cyanosis (central/peripheral), pallor, cachexia, jaundice (congestive hepatopathy).
- Environment: oxygen (litres/min), nebulisers, GTN spray, ECG monitor, fluid balance chart, walking aids, drains (post-sternotomy).
- Bedside clues: urine pot (haematuria – IE), sputum (frothy pink – pulmonary oedema), temperature chart (fever – IE).
2️⃣ Hands & Arms ✋
- Inspection: clubbing (cyanotic CHD, IE), splinter haemorrhages (IE), Osler nodes (painful, IE), Janeway lesions (painless, IE), tendon xanthomata (familial hypercholesterolaemia), nicotine staining, arachnodactyly (Marfan), joint hypermobility (Ehlers-Danlos).
- Temperature/perfusion: warm/cold peripheries (high/low output HF), capillary refill (<2 s normal).
- Pulses:
- Rate: brady (<60), tachy (>100); count 15 s or full minute if irregular.
- Rhythm: regular / irregularly irregular (AF) / regularly irregular (ectopics, Mobitz II).
- Character: collapsing/water-hammer (AR, PDA, hyperdynamic states), slow-rising/parvus et tardus (AS), bisferiens (mixed AS/AR, HOCM), jerky (HOCM), pulsus alternans (severe LV failure), bigeminus (digoxin toxicity, ectopy).
- Comparisons: radio-radial delay (subclavian stenosis), radio-femoral delay (coarctation), pulse deficit (AF, frequent ectopy).
3️⃣ Face, Eyes, Mouth & Neck 🙂👁️🧣
- Eyes: xanthelasma (hyperlipidaemia), corneal arcus (familial hypercholesterolaemia), conjunctival pallor (anaemia), Roth spots (IE), hypertensive retinopathy (Keith-Wagener-Barker grades).
- Mouth: central cyanosis (lips/tongue), poor dentition (IE risk), high-arched palate (Marfan).
- Face: malar flush (mitral stenosis), Down/Turner/Marfan facies (syndromic associations).
- Neck:
- JVP at 45° (tangential light), measure vertical height above sternal angle + 5 cm (normal <3–4 cm).
- Waveform: giant a (pulmonary HTN, TS), cannon a (complete heart block), large v (TR).
- Hepatojugular reflux (sustained rise ≥3 cm → RV dysfunction).
- Carotid pulse: palpate one side, then auscultate for bruits (carotid stenosis, AS radiation).
4️⃣ Chest Inspection 👕
- Scars: median sternotomy (CABG, valve surgery), lateral thoracotomy (PDA, coarctation), infraclavicular (PPM/ICD), axillary (minimally invasive valve).
- Deformities: pectus excavatum/carinatum, scoliosis/kyphosis (Marfan, severe RVH).
- Visible pulsations: RV heave, suprasternal thrill (AS), apical impulse.
- Pacemaker/ICD bulge, port-a-cath scars (long-term antibiotics – IE).
5️⃣ Palpation 🤲
- Apex beat: normal 5th ICS, mid-clavicular line; displaced laterally/downward (LV dilatation), heaving (LVH), tapping (MS).
- Heaves: left parasternal (RVH, pulmonary HTN), apical (LVH).
- Thrills: palpable murmurs (e.g., grade 4+ AS at aortic area, MR at apex).
6️⃣ Auscultation 🎧 – Systematic & Targeted
- Areas (use diaphragm for high-pitched, bell for low-pitched; patient breathing normally then held expiration):
- 🔴 Aortic area – 2nd ICS right sternal border
- 🔵 Pulmonary area – 2nd ICS left sternal border
- 🟢 Tricuspid area – lower left sternal edge (4th–5th ICS)
- 🟣 Mitral area – apex (5th ICS mid-clavicular line)
- Axilla → radiation of MR
- Carotids → radiation of AS (after checking bruits)
- Heart sounds: S1 (mitral/tricuspid closure), S2 (aortic/pulmonary closure; physiological splitting on inspiration), loud/soft, fixed/reversed splitting.
- Extra sounds: S3 (ventricular gallop – HF), S4 (atrial kick – stiff LV), opening snap (MS), ejection click (bicuspid aortic valve), mid-systolic click (MVP).
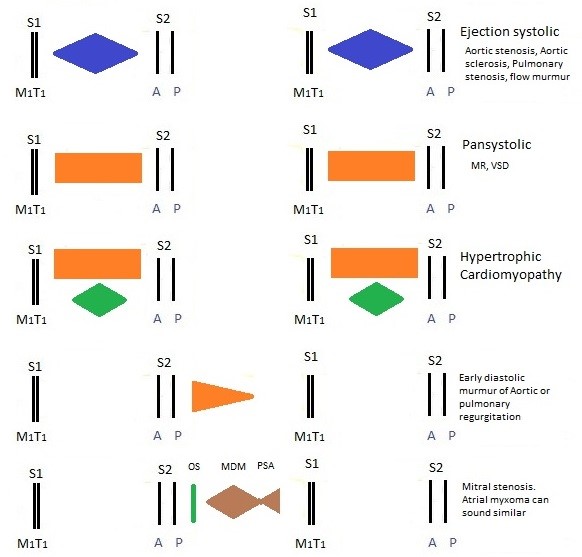
- Murmurs: timing (systolic/diastolic/continuous), grade (1–6), character (harsh/blowing), radiation, response to manoeuvres.
- Pericardial rub: scratchy, triphasic, best leaning forward.
7️⃣ Special Manoeuvres (Increase Diagnostic Yield) ⚡
- Valsalva (strain phase) → ↑ HOCM murmur, ↓ AS/MR.
- Handgrip (isometric) → ↑ MR/AR/VSD, ↓ AS/HOCM.
- Left lateral decubitus + bell → accentuates MS rumble, S3/S4.
- Sit forward + breath held in expiration → accentuates AR (high-pitched decrescendo).
- Standing/squatting → dynamic changes in HOCM (↑ on standing, ↓ on squatting).
8️⃣ Peripheral Signs & Systemic Clues 👣🫁
- Lung bases: bilateral crackles (pulmonary oedema in HF).
- Sacral/ankle oedema: pitting (RHF, constrictive pericarditis, nephrotic syndrome).
- Legs: saphenous vein harvest scars (CABG), varicose veins, DVT signs.
- Abdomen: hepatomegaly (RHF), ascites (shifting dullness), pulsatile liver (TR).
- Other: sacral oedema, pleural effusion (HF), splenomegaly (IE).
9️⃣ Closure & Completion 🙏
- Thank patient, cover up, help redress.
- Wash hands.
- Present findings clearly & succinctly (e.g., “This patient has an ejection systolic murmur loudest in the aortic area, radiating to carotids, slow-rising pulse, narrow pulse pressure – consistent with severe aortic stenosis”).
- State: “To complete my examination, I would like to measure BP in both arms, perform fundoscopy, dip urine for protein/haematuria, and arrange ECG and transthoracic echo.”
OSCE Examiner Tips & High-Yield Phrases • Verbalise everything: “I’m now palpating for the apex beat in the 5th intercostal space, mid-clavicular line...” • If you miss something: “I would also check for...” – still scores points. • JVP: “I’m assessing JVP at 45° with tangential light; hepatojugular reflux is negative.” • Murmurs: describe timing, site, grade, radiation, character, manoeuvres. • Always integrate: “The collapsing pulse and wide pulse pressure support aortic regurgitation.” • Do-not-miss: new murmur + fever + embolic signs = infective endocarditis → urgent echo + blood cultures.
📊 High-Yield Cardiac Examination Findings Table
| Finding | Key Features | Associated Conditions | Technique / Clue |
|---|---|---|---|
| Collapsing pulse | Bounding upstroke, rapid collapse | Aortic regurgitation, PDA, AV fistula, thyrotoxicosis | Raise arm above head |
| Slow-rising pulse | Parvus et tardus | Severe aortic stenosis | Carotid palpation |
| Displaced apex beat | Lateral/downward | LV dilatation (MR, AR, DCM) | 5th ICS, anterior axillary line |
| Heaving apex | Sustained thrust | LV hypertrophy (AS, HTN) | Palpation |
| Parasternal heave | RV lift | Pulmonary hypertension, RVH | Left sternal edge |
| S3 | Early diastolic gallop | Heart failure, volume overload | Bell at apex, left lateral |
| S4 | Late diastolic | Stiff LV (HTN, AS) | Bell at apex |
| Opening snap | Sharp sound after S2 | Mitral stenosis | Left lateral, bell |
| Pericardial rub | Scratchy, triphasic | Acute pericarditis | Lean forward, breath hold |
🚩 Do-Not-Miss Red Flags in OSCE
- Fever + new murmur + embolic signs → infective endocarditis
- Syncope + ejection systolic murmur in elderly → severe AS
- Diastolic murmur → always pathological (AR/MS)
- Discrepant arm BP + radio-femoral delay → coarctation/aortic dissection
- Raised JVP + Kussmaul sign → constrictive pericarditis
📚 References & Resources (Feb 2026)
- Talley & O’Connor – Clinical Examination (9th ed., 2025 update).
- Geeky Medics Cardiovascular Examination OSCE Guide (2026 revision).
- OSCEstop & PassMedicine cardiology sections.
- ESC Guidelines: Valvular Heart Disease (2025 update).
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
