Osteochondroma
🦴 Osteochondroma is the most common benign bone tumour, arising as a cartilage-capped bony projection from the metaphysis of long bones.
🔎 Often found near growth plates (especially knee & proximal humerus), it is usually asymptomatic but can occasionally cause pain, mechanical problems, or-rarely-malignant transformation.
📖 About
- Definition: A benign bone tumour composed of bone & cartilage, projecting from the metaphysis.
- Types:
- Solitary Osteochondroma: Single lesion, usually incidental & asymptomatic.
- Multiple Osteochondromas (Hereditary Multiple Exostoses, HME): Autosomal dominant, multiple lesions, limb deformities, higher malignancy risk.
📊 Classification
| Type |
Description |
| Solitary Osteochondroma |
Single benign bony outgrowth, often found incidentally on imaging. |
| Multiple Osteochondromas (HME) |
Inherited condition with multiple lesions; associated with deformities and ↑ risk of malignant transformation. |
📈 Epidemiology
- Accounts for 20–50% of benign bone tumours.
- Most cases diagnosed in childhood/adolescence (linked with growth spurts).
- More common in males.
- HME prevalence: ~1 in 50,000.
🧬 Pathophysiology
- Originates from growth plate (physis), growing outward as a stalk capped with cartilage.
- In HME: mutations in EXT1/EXT2 genes (heparan sulfate synthesis).
- Malignant change (rare): usually to secondary chondrosarcoma.
🩺 Clinical Features
- Asymptomatic: Incidental finding on X-ray.
- Symptomatic:
- Local pain/discomfort.
- Mechanical restriction of joint movement.
- Neurovascular compression → numbness, tingling, weakness, or ischaemia.
- Visible or palpable hard bony lump.
🔬 Diagnosis
- Clinical: Hard, painless mass near a joint.
- Imaging:
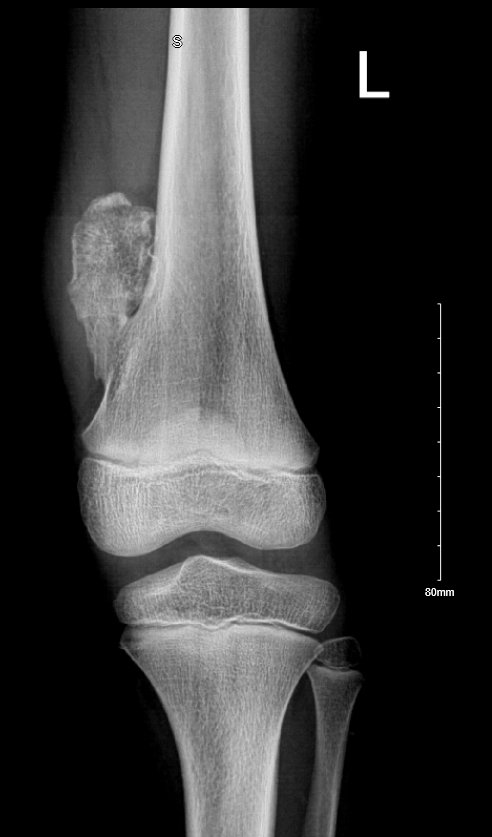
- 📸 X-ray: Bony outgrowth with cortex & medulla continuous with parent bone.
- 🖥️ CT: Defines bony architecture.
- 🧲 MRI: Key for measuring cartilage cap (>1.5–2 cm in adults → suspicious for malignancy).
- Biopsy: Rare, reserved for suspicious cases.
- Genetics: EXT1/EXT2 testing in HME.
💊 Management
- Observation: Asymptomatic cases → regular follow-up.
- Surgical Excision:
- Indicated if pain, deformity, restricted motion, or neurovascular compression.
- Complete removal of bony stalk + cartilage cap prevents recurrence.
- Malignant Transformation:
- Red flags: rapid growth, worsening pain, cap thickening >2 cm.
- Requires wide resection ± oncology input.
- Genetic Counselling: For HME families.
📉 Prognosis
- Excellent for solitary lesions.
- HME: ↑ risk of deformity & ~1–5% chance of malignant change.
⚠️ Complications
- Chondrosarcoma transformation.
- Limb length discrepancies or angular deformities.
- Nerve/vascular compression.
📚 References

