| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Cerebral Amyloid angiopathy (CAA) ✅
Related Subjects: |Acute Stroke Assessment (ROSIER&NIHSS) |Atrial Fibrillation |Atrial Myxoma |Causes of Stroke |Ischaemic Stroke |Cancer and Stroke |Cardioembolic stroke |CT Basics for Stroke |Endocarditis and Stroke |Haemorrhagic Stroke |Stroke Thrombolysis |Hyperacute Stroke Care
🧠 Cerebral Amyloid Angiopathy (CAA) = amyloid-β deposition in walls of small/medium cerebral vessels → fragility → recurrent lobar ICH. 💡 Suspect in age >70, lobar haemorrhage, normotensive, often with cognitive decline or “amyloid spells” (TIA-like).
📖 Introduction
- CAA is a common cause of spontaneous lobar intracerebral haemorrhage in elderly.
- Deposition occurs in leptomeningeal & cortical vessels, distinct from systemic amyloidosis (Pantoni 2010).
- Inflammatory variant (CAA-RI) can cause subacute deficits and is steroid-responsive (Moussaddy 2015).
⚙️ Aetiology & Genetics
- Amyloid-β fibril deposition in small cortical/leptomeningeal arteries.
- Often coexists with Alzheimer’s, but not all CAA patients have dementia.
- Genetics: ApoE ε2/ε4 alleles; rare familial forms – Dutch type (APP mutation, midlife lobar ICH ± dementia), Icelandic type (Cystatin C mutation, brainstem/cerebellar involvement).
🔬 Pathology
- Lobar haemorrhage (temporal/occipital > frontal/parietal), sparing deep nuclei (contrast with hypertensive bleeds).
- Microscopy: β-amyloid in media & adventitia; Congo red +ve.
- CAA-RI: inflammatory infiltrates, oedema on MRI, steroid-responsive.
🩺 Clinical Features
- Acute lobar ICH → headache, focal neurological deficits, seizures, coma in severe cases.
- “Amyloid spells” = transient, TIA-like deficits from small cortical bleeds.
- Recurrent micro/macrobleeds, sometimes provoked by minor trauma or antithrombotic therapy.
- Progressive cognitive decline if multiple haemorrhages.
🖼️ Imaging & Investigations
- CT: Acute lobar ICH; may recur in different lobes; deep nuclei spared.
- MRI T2*/GRE/SWI: Microbleeds (<10 mm), cortical superficial siderosis, white matter changes.
- CAA-RI: T2 MRI shows oedema; often steroid-responsive.
- CTA/MRA: Exclude vascular malformations or venous sinus thrombosis.
- PET: Research only; amyloid imaging.
- Genetics: ApoE typing or APP/Cystatin C for suspected familial cases.
- Histology: Congo red staining post-mortem or biopsy confirms amyloid.
🧾 Boston Criteria (Revised)
| Category | Definition |
|---|---|
| Definite | Post-mortem: lobar haemorrhage + severe CAA, no other cause. |
| Probable with pathology | Lobar haemorrhage + biopsy/haematoma specimen showing amyloid, no other cause. |
| Probable | Age >60, multiple lobar bleeds on imaging, no other cause. |
| Possible | Age >60, single lobar bleed, no other cause. |
🚩 Differentials
- Hypertensive deep bleed
- Lobar extension from putaminal ICH
- Haemorrhagic infarct transformation
- AVM or haemorrhagic tumour
- Venous sinus thrombosis
📉 Complications
- Recurrent ICH
- Seizures
- Hydrocephalus (rare)
- Dementia (stepwise or progressive)
- Inflammation
💊 Management (Guideline-Aligned)
- ⚠️ Avoid antiplatelets, anticoagulants, thrombolysis if possible – high risk of recurrent lobar ICH (AHA/ASA 2022; NICE NG128).
- Standard acute haemorrhagic stroke care:
- BP control: target SBP ~130–150 mmHg acutely; long-term <140/90 mmHg.
- ICP management and supportive care.
- Seizure prophylaxis if indicated.
- Multidisciplinary stroke unit care.
- Falls prevention and trauma reduction.
- Surgery only for life-threatening haematoma or hydrocephalus.
- CAA-RI: steroids for inflammatory variant.
- Long-term: cognitive support, seizure management, lifestyle optimisation (BP, diet, exercise, limit alcohol, avoid smoking).
📖 Guideline Evidence
- International CAA/WORLD STROKE ORGANIZATION (2025): Diagnosis, risk stratification, antithrombotic avoidance, CAA-RI management.
- AHA/ASA 2022 Spontaneous ICH Guideline: Acute BP lowering, imaging-based risk assessment, stroke unit care.
- UK NICE Stroke Guidance NG128: Acute ICH care, BP control, stroke unit admission, MDT management.
- Radiopaedia – Imaging pearls
🖼️ Example Imaging
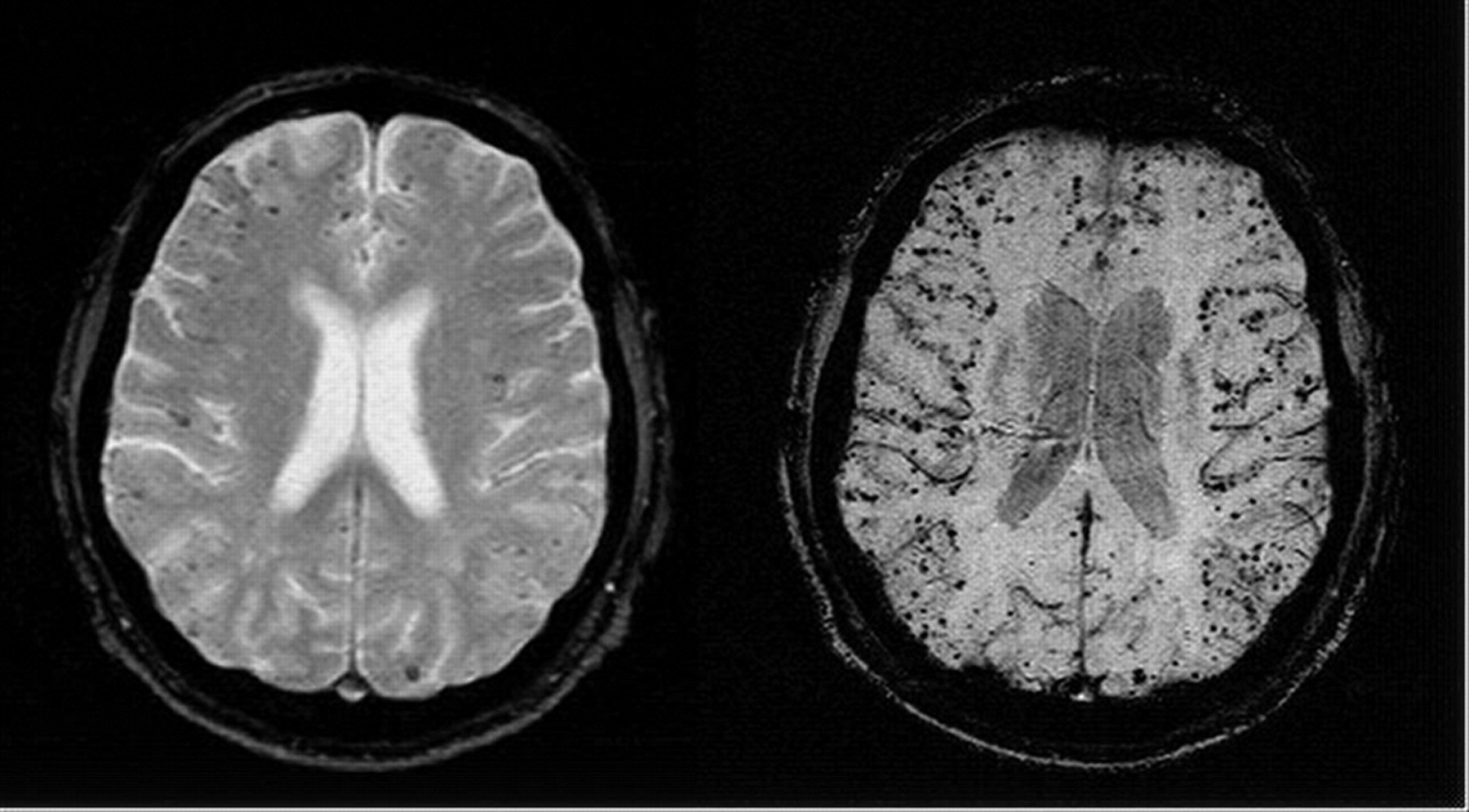
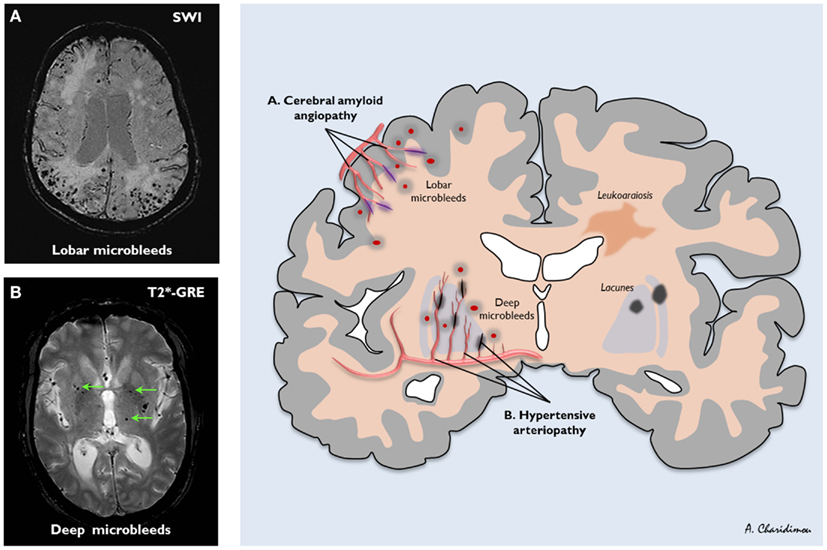
💡 Exam Pearls
– Age >70 + lobar ICH + normotension → think CAA.
– MRI T2*/GRE/SWI → detect microbleeds (“pepper pot cortex”).
– Avoid anticoagulation unless absolutely necessary; consider specialist review.
– CAA-RI variant → steroid-responsive; acute BP control crucial.
– Recurrent lobar bleeds and stepwise cognitive decline suggest advanced disease.
📚 References
- Knudsen KA, Rosand J, Karluk D. Clinical diagnosis of CAA: Boston criteria. Neurology. 2001;56(4):537–9.
- CAA Systematic Review. J Clin Neurol 2011;7:1–9
- Cordonnier C, et al. International CAA Association/World Stroke Organization Scientific Statement 2025.
- AHA/ASA 2022 Spontaneous ICH Guideline
- NICE Guidance: Stroke and TIA, NG128
- Radiopaedia – CAA Imaging
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
