| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Hyponatraemia ✅
Related Subjects: | Sodium Physiology | Hyponatraemia | TURP Hyponatraemia syndrome | Hypernatraemia | Diabetes Insipidus | SIADH
⚠️ Hyponatraemia (Na⁺ <135 mmol/L): A clinical emergency when acute or severe. 🧠 Pathophysiology: Low extracellular sodium creates an osmotic gradient that drives water into brain cells, causing cerebral oedema and increased intracranial pressure. 📈 The "Rule of 8": Aim for a correction of 4–6 mmol/L/24h. Absolutely limit rise to <10 mmol/L in 24h to prevent irreversible brain damage (ODS).
| 🚨 Emergency Management (Severe Symptoms) |
|---|
|
Definition of Severe Symptoms: Seizures, GCS <8, status epilepticus, or respiratory arrest.
|
🔬 Deep Dive: Diagnostic Investigations
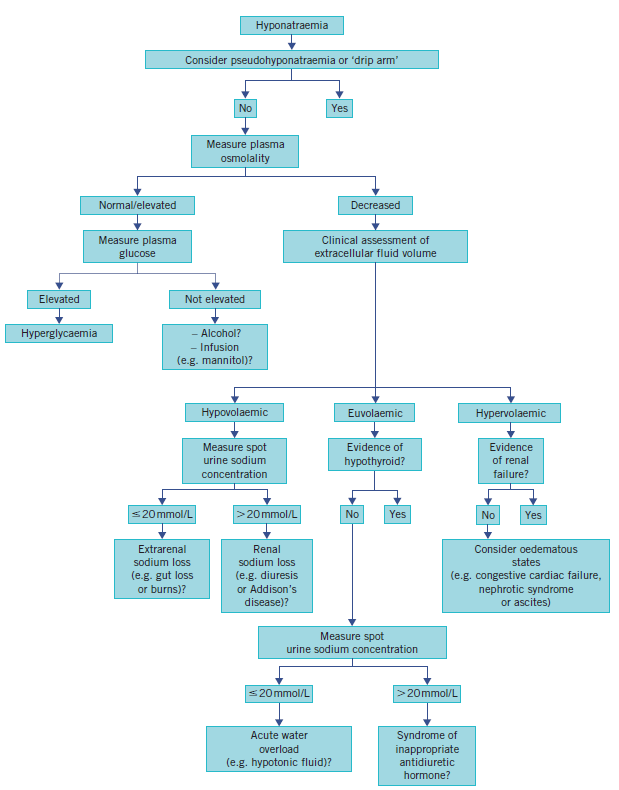
Diagnosis must follow a logical sequence to avoid incorrect treatment (e.g., giving saline to an SIADH patient, which worsens the drop).
- 1. Confirm True Hyponatraemia:
- Check Serum Osmolality. If >275 mOsm/kg, it is "secondary" (e.g., Hyperglycaemia). If normal, it is "Pseudohyponatraemia" (Hyperlipidaemia/Hyperproteinaemia).
- 2. Assess ADH Activity:
- Check Urine Osmolality. If <100 mOsm/kg, ADH is appropriately suppressed (e.g., Psychogenic Polydipsia or "Tea and Toast" diet). If >100 mOsm/kg, ADH is active and driving the hyponatraemia.
- 3. Differentiate SIADH vs. Hypovolaemia:
- Check Urine Sodium (UNa).
- UNa <30 mmol/L: The kidneys are desperately holding onto salt. This indicates effective volume depletion (Hypovolaemia, Heart Failure, or Cirrhosis).
- UNa >30 mmol/L: The kidneys are losing salt. This suggests SIADH, Diuretics, or Adrenal Insufficiency.
- Check Urine Sodium (UNa).
⚖️ SIADH: Formal Diagnostic Criteria
To diagnose SIADH (Syndrome of Inappropriate Antidiuretic Hormone), you must meet all the following:
- Hyponatraemia (Na⁺ <135).
- Low plasma osmolality (<275 mOsm/kg).
- Inappropriately concentrated urine (Urine Osm >100 mOsm/kg).
- Elevated Urine Sodium (>30 mmol/L) with normal salt/water intake.
- Exclusion of adrenal, thyroid, pituitary, or renal dysfunction.
- Exclusion of diuretic use.
⚠️ Osmotic Demyelination Syndrome (ODS) - The Danger Zone
ODS (formerly Central Pontine Myelinolysis) occurs when brain cells, having adapted to a low-sodium environment, are suddenly "shrunk" by rapid sodium replacement. This tears the myelin sheaths off neurons.
- High-Risk Patients (Limit rise to <8 mmol/L/24h):
- Chronic Alcoholism.
- Liver Disease / Malnutrition.
- Hypokalaemia (Low K⁺ increases ODS risk).
- Clinical Presentation: Initially, the patient improves. 2–6 days later, they develop:
- Dysphagia/Dysarthria (difficulty swallowing/speaking).
- Quadriparesis (weakness in all limbs).
- Locked-in Syndrome (total paralysis except for eye movement).
🩺 Management Strategies by Aetiology
| Type | Common Causes | NICE/Consensus Treatment |
|---|---|---|
| Hypovolaemic | Vomiting, diarrhoea, excessive sweating, Thiazide diuretics, Addison's disease. | 0.9% Sodium Chloride. Restore volume to stop the ADH "thirst" drive. |
| Euvolaemic | SIADH (Lung CA, SSRIs, Carbamazepine, Pneumonia), Hypothyroidism. | Fluid Restriction (1st line). 800mL–1L. Tolvaptan (V2 receptor antagonist) as 2nd line. |
| Hypervolaemic | Congestive Heart Failure, Liver Cirrhosis, Nephrotic Syndrome. | Fluid & Salt Restriction + Loop Diuretics. Treat the underlying organ failure. |
💡 Clinical Pearls & Advanced Tips
- The "Corrected Sodium" in Hyperglycaemia: Glucose is osmotically active.
Formula: Corrected Na⁺ = Measured Na⁺ + 2.4 × ([Glucose - 5.5] / 5.5). - The Danger of "Beer Potomania": Heavy beer drinkers have very low protein intake. They cannot excrete water because they lack the "solute" (urea) to take the water with it. They are at extreme risk of ODS.
- Thiazides vs. Loops: Thiazides block sodium reabsorption in the distal tubule but leave the "concentrating power" of the kidney intact, leading to profound hyponatraemia. Loop diuretics (Furosemide) actually help treat hyponatraemia by "washing out" the medullary gradient.
- Potassium Correction: Replacing K⁺ will actually raise your serum Na⁺. If you are correcting both, you must monitor sodium even more frequently to avoid over-correction.
📚 References
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
