| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
AIDS Dementia Complex (HIV) ✅
Related Subjects: |Dementias |AIDS (HIV) Neurological Disease |AIDS (HIV) Respiratory disease |AIDS Dementia Complex (HIV) |AIDS HIV Infection |AIDS(HIV) Gastrointestinal Disease |Acute Retroviral Syndrome (HIV) |HIV and Post-Exposure Prophylaxis (PEP) |HIV and Pre-exposure prophylaxis |HIV associated nephropathy (HIVAN) |HIV disease Assessment
Early/subtle HIV-associated neurocognitive disorders (HAND) may contribute to reduced inhibition, impulsivity, and increased risk behaviours (e.g., unprotected sex), though evidence is limited and multifactorial. Effective ART usually prevents progression to severe forms.
ℹ️ About
- HIV-associated neurocognitive disorder (HAND) spectrum: from asymptomatic/subtle impairment to rare severe dementia (HAD).
- Rare in virally suppressed patients on effective ART (cART/HAART); prevalence of severe HAD <5% in treated cohorts.
- Risk highest with low CD4 (<200 cells/µL), high viral load, or delayed ART initiation.
🧬 Aetiology & Pathophysiology
- HIV enters CNS early via infected monocytes/macrophages; persistent low-level replication/inflammation despite systemic suppression.
- Damage to basal ganglia, subcortical white matter, frontal cortex → cognitive, motor, behavioural changes.
- Legacy effects (pre-ART damage) + comorbidities (ageing, vascular, substance use) contribute in modern era.
🩺 Clinical Features
- Gradual cognitive decline: memory, concentration, executive function, psychomotor slowing.
- Behavioural: apathy, irritability, reduced inhibition (may increase risk behaviours early).
- Mood: depression/anxiety common; psychosis rare/late.
- Motor: slowing, gait issues in advanced cases.
🔎 Differential Diagnosis
- Other causes of cognitive impairment: depression ("pseudodementia"), substance use, CNS lymphoma, PML, vascular dementia, Alzheimer's, B12 deficiency, hypothyroidism.
- Exclude delirium, opportunistic infections (e.g., toxoplasmosis, cryptococcal meningitis).
🔬 Investigations
- HIV-specific: CD4 count, plasma viral load; CSF HIV RNA if CNS escape suspected.
- Screen: FBC, U&E, LFT, TFT, B12/folate, glucose, syphilis serology.
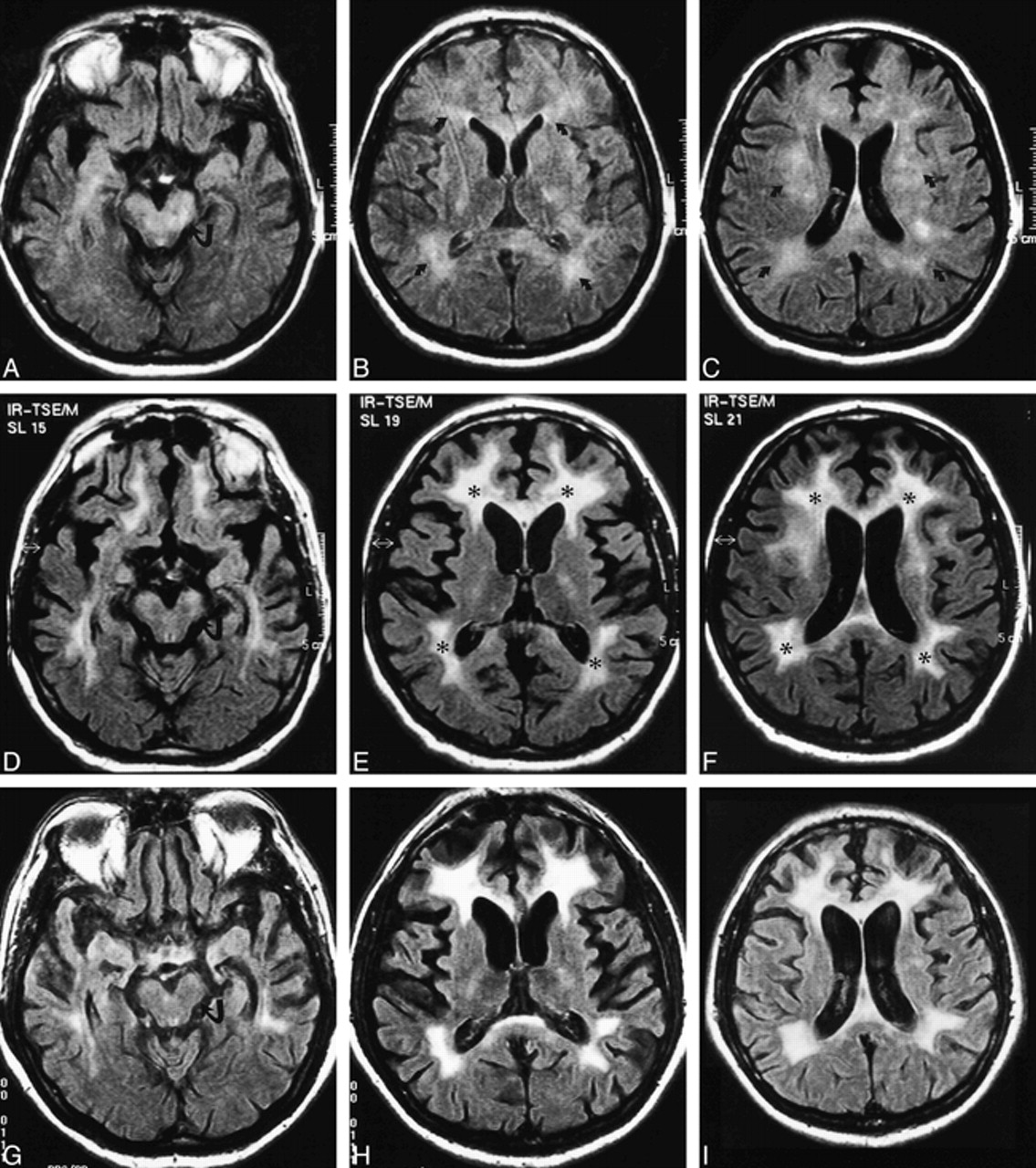
- Neuroimaging: MRI preferred (subcortical white matter changes, atrophy); CT if MRI unavailable.
- CSF: mild pleocytosis/protein elevation, elevated beta-2 microglobulin/IgG; rule out opportunistic infections.
- Neuropsychological testing: assess ≥5 domains (e.g., MoCA/HAND screen for initial; full battery if indicated).
📊 Classification (Frascati Criteria – Current Standard)
| Category | Criteria | Functional Impact |
|---|---|---|
| Asymptomatic Neurocognitive Impairment (ANI) | ≥1 SD below mean in ≥2 cognitive domains on testing | No interference in daily functioning |
| Mild Neurocognitive Disorder (MND) | ≥1 SD below mean in ≥2 domains | Mild interference in daily activities |
| HIV-associated Dementia (HAD) | ≥2 SD below mean in ≥2 domains (often multiple) | Marked interference; inability to work/perform complex tasks |
MSK staging (0–4) is historical; focus on functional impact now.
💊 Management
- ART optimisation: Immediate/effective cART (BHIVA 2025) to achieve/maintain viral suppression in plasma ± CSF; preferred regimens with good CNS penetration (e.g., integrase inhibitors + tenofovir/emtricitabine or doravirine-based).
- Screen/treat comorbidities: depression, substance use, vascular risk factors.
- Supportive: cognitive rehabilitation, psychoeducation, social support; monitor annually (BHIVA recommends screening for cognitive concerns).
- Referral: HIV specialist + neurology/ neuropsychology if progressive or severe.
References (Current as of March 2026)
- BHIVA antiretroviral guidelines 2025 interim update (focus on CNS penetration/monitoring).
- Frascati criteria (2007) with proposed revisions (2021–2023 consensus: emphasise functional impact over asymptomatic testing alone).
- NICE NG97 Dementia (2018) & NG222 Mental health (2022) – exclude reversible causes like HIV.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
