| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Cytomegalovirus (CMV) Retinitis ✅
Related Subjects:
|Herpes Varicella-Zoster (Shingles) Infection
|Chickenpox Varicella Infection
|Varicella Cerebral Vasculopathy
|Herpes Viruses
|Herpes Zoster Ophthalmicus (HZO) Shingles
|MonkeyPox
|Mumps
|Measles
|Rubella (German Measles)
|Epstein-Barr Virus infection
|Cytomegalovirus (CMV) infections
|CMV retinitis infections
|Toxoplasmosis
🦠 Aetiology & Pathophysiology
- Caused by reactivation of latent CMV (a β-herpesvirus) in severely immunocompromised individuals.
- Viral replication in retinal vascular endothelium → haemorrhagic necrosis, perivascular inflammation, and exudation.
- May disseminate to involve optic nerve, brain (encephalitis), gastrointestinal tract, lungs, or other organs in disseminated CMV disease.
🧍♂️ Clinical Features
- Typically occurs at CD4 <50 cells/mm³ (rare above 100 cells/mm³ with effective ART).
- Symptoms: floaters, blurred vision, scotomas, photopsia (flashing lights), ocular pain (less common).
- Often unilateral at presentation but progresses to bilateral in ~50% without treatment.
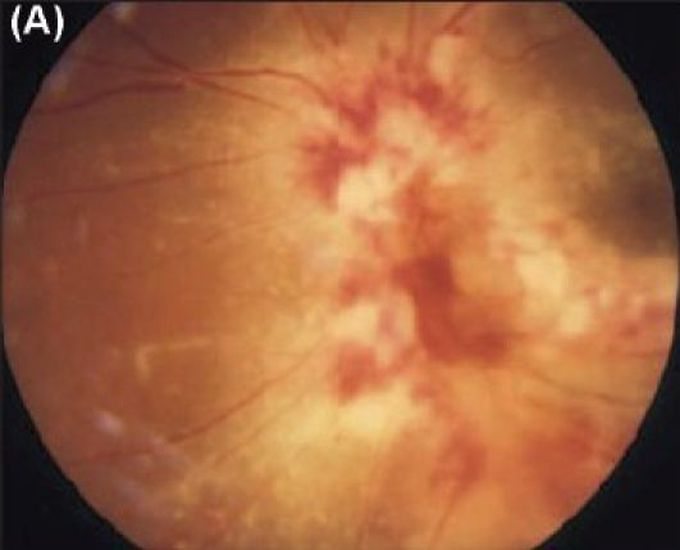
- Fundoscopy: Classic “pizza-pie” or “cottage cheese and ketchup” appearance — confluent yellow-white areas of retinal necrosis with overlying retinal haemorrhages.
Characteristic Fundus Appearance:
 >
>
Without therapy, rapid progression to retinal detachment, optic atrophy, and permanent blindness occurs.
🔍 Differential Diagnosis
- HIV-associated toxoplasma chorioretinitis (more focal, less haemorrhagic).
- Acute retinal necrosis (herpes simplex or varicella-zoster virus — peripheral, rapidly progressive).
- Progressive outer retinal necrosis (VZV in profound immunosuppression).
- Ischaemic or diabetic retinopathy.
- Syphilitic or tuberculous chorioretinitis.
🧪 Investigations & Diagnosis
- Clinical diagnosis: Characteristic fundoscopic findings are highly specific in the appropriate clinical context.
- Dilated fundoscopy by ophthalmologist (gold standard).
- Retinal photography and visual field testing for monitoring progression/response.
- CMV PCR on vitreous fluid or aqueous humour (if diagnostic uncertainty).
- Blood CMV PCR useful for systemic disease but poor predictor of retinitis relapse.
- Urgent ophthalmology referral essential.
💊 Management (2025–2026 Guidelines)
Prevention
- Routine dilated fundoscopic screening every 3–6 months in HIV patients with CD4 <100 cells/mm³ (or <50 in high-risk cases).
- Primary prophylaxis not routinely recommended (no proven benefit vs toxicity).
- Early initiation/optimisation of ART to maintain CD4 >100–200 cells/mm³ is most effective prevention.
Treatment
Preferred first-line (NIH Guidelines, July 2025; AI rating):
| Regimen | Dosing | Indications/Notes |
|---|---|---|
| Valganciclovir (oral, preferred) | Induction: 900 mg PO twice daily × 14–21 days
Maintenance: 900 mg PO once daily | Most cases; equivalent efficacy to IV; take with food. |
| Ganciclovir (IV) | Induction: 5 mg/kg IV every 12 hours × 14–21 days
Maintenance: 5 mg/kg IV daily or switch to oral valganciclovir | Severe/sight-threatening (macula/optic disc involvement) or poor oral absorption; transition to oral when stable. |
Sight-threatening lesions (within 1,500 microns of fovea or optic disc): Add intravitreal ganciclovir (2 mg/injection) or foscarnet (2.4 mg/injection) weekly during induction (BIII).
Alternatives (resistance, intolerance, or failure):
- Foscarnet IV (BI): 60–90 mg/kg every 8–12 hours induction, then maintenance.
- Cidofovir IV (CI): 5 mg/kg weekly × 2, then every 2 weeks (with probenecid; avoid if sulfonamide allergy).
- Intravitreal foscarnet (for local control).
ART timing: Initiate/optimise HAART after initial CMV control (typically 2 weeks delay if sight-threatening) to reduce risk of immune reconstitution uveitis (IRU/IRIS).
Immune Recovery Uveitis (IRU)
- Occurs post-ART with rising CD4; vitritis, macular oedema, even with inactive retinitis.
- Treat active inflammation with corticosteroids (oral prednisone 1 mg/kg/day tapered, periocular, or intravitreal) + continue anti-CMV if needed (CIII).
Discontinuing Maintenance Therapy
- After ≥3 months treatment, inactive lesions, and sustained CD4 ≥100 cells/mm³ on ART ≥3 months (AII).
- Continue ophthalmologic monitoring (every 3 months initially, then yearly) for relapse/IRU (AIII).
- Blood CMV PCR not recommended for relapse prediction (AII).
Monitoring & Follow-up
- Close collaboration: HIV specialist + ophthalmologist.
- Regular fundoscopy (weekly during induction if severe, then monthly).
- Monitor for drug toxicities (e.g., neutropenia with ganciclovir/valganciclovir, nephrotoxicity with foscarnet/cidofovir).
📚 Key References (2025–2026)
- NIH/CDC/HHS Opportunistic Infections Guidelines: Cytomegalovirus Disease (updated July 2025).
- Asia-Pacific Vitreo-retina Society (APVRS) Consensus on CMV Retinitis (2025).
- BHIVA Opportunistic Infection Guidelines (latest GI module 2024; aligns with valganciclovir preference).
- EyeWiki & UpToDate: CMV Retinitis (updated 2025–2026).
This summary provides a concise, evidence-based overview suitable for clinical reference, teaching, or patient education.
