| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Tinea Corporis and Tinea faciei(Ringworm) ✅
🦠 Tinea corporis (ringworm of the body) is a superficial dermatophyte infection affecting the glabrous skin of the trunk and limbs. It classically causes an annular, scaly, erythematous plaque with a more active advancing edge and partial central clearing. Although “ringworm” is often used loosely for fungal skin infection anywhere, infection of the face is more precisely termed tinea faciei, while infection of the beard area is tinea barbae and infection of the scalp is tinea capitis.
🔎 Aetiology
Caused by dermatophyte fungi that invade keratinised tissue (stratum corneum, hair, nails).
- Trichophyton rubrum – common worldwide 🌍.
- Trichophyton mentagrophytes / interdigitale complex – may be human or animal acquired.
- Microsporum canis – linked to cats and dogs 🐱🐶.
- Epidermophyton floccosum – less common, but a recognised dermatophyte cause.
⚡ Risk Factors
- 🌡️ Warm, humid conditions and occlusion (sport, sweating, tight clothing).
- 👨👩👧 Close contact with infected people, pets, or contaminated items.
- 🧦 Shared towels, clothing, gym mats, helmets, or sports equipment.
- 💦 Hyperhidrosis and macerated skin.
- 🛡️ Immunosuppression (for example diabetes, HIV, systemic steroids, chemotherapy).
- 💊 Topical steroid use, which may mask the rash and cause tinea incognito.
- 🦶 Autoinoculation from another fungal site, especially feet or nails.
🩺 Clinical Presentation
- Typical lesion:
- Annular or oval scaly erythematous plaque with a more active edge 🔴.
- Partial central clearing is common but not universal.
- Expands gradually outwards; multiple lesions may coalesce.
- Symptoms:
- Pruritus is common 🚨.
- Mild burning, irritation, or cosmetic concern may occur.
- Common sites: trunk, chest, back, arms, and legs.
- Face: dermatophyte infection of the face is usually called tinea faciei.
- Often presents as an asymmetrical, unilateral, scaly red patch with a leading edge.
- May be mistaken for eczema, seborrhoeic dermatitis, rosacea, contact dermatitis, or lupus.
- Often worsens or becomes less typical after steroid cream use.
- Beard/scalp involvement: think tinea barbae or tinea capitis rather than simple tinea corporis.
🧾 Diagnosis
Diagnosis is often clinical, but send skin scrapings for mycology if the diagnosis is uncertain, disease is extensive, recurrent, inflammatory, or not responding to initial treatment.
- 👀 Clinical examination: annular/scaly plaque with a more active edge.
- 🔬 Microscopy / KOH: fungal hyphae may be seen in skin scrapings.
- 🧫 Fungal culture (or PCR where available): useful in resistant, recurrent, or atypical cases.
- ✂️ Take scrapings from the advancing scaly edge of the lesion.
- 💡 Wood’s lamp: may help with some Microsporum infections, but is not routinely diagnostic for most cases.
🔀 Differential Diagnosis
- Atopic eczema 🤧
- Nummular eczema
- Psoriasis 🧴
- Pityriasis rosea 🌹
- Granuloma annulare
- Seborrhoeic dermatitis
- Rosacea
- Contact dermatitis
- Cutaneous lupus erythematosus
- Tinea incognito (steroid-modified fungal infection)
💊 Treatment
Management depends on site, extent, severity, and whether hair-bearing skin is involved.
- Topical antifungal (first-line for localised body infection):
- Terbinafine 1% cream/gel/spray – usually once or twice daily for 1–2 weeks.
- Alternative imidazole cream (for example clotrimazole or miconazole) – usually for 2–4 weeks.
- Oral antifungal if disease is extensive, recurrent, treatment-resistant, very inflammatory, or involves hair-bearing areas:
- Terbinafine 250 mg OD for 4 weeks is a common adult regimen for body infection.
- If facial infection is extensive or not responding to topical treatment, oral treatment may be needed.
- Tinea barbae and tinea capitis usually require systemic treatment.
- Avoid steroid monotherapy ❌ – this can mask the rash and worsen fungal spread.
- Supportive advice: keep skin dry, treat other fungal sites (especially feet/nails), and check pets if zoonotic infection is suspected.
🛡️ Prevention
- Avoid sharing towels, clothing, razors, hats, helmets, or gym equipment.
- Keep skin clean and dry; change sweaty clothes promptly 👕.
- Treat concurrent tinea pedis or onychomycosis to reduce recurrence.
- Check household pets if recurrent infection suggests a zoonotic source.
⚠️ Complications / When to Think Again
- 📈 Spread to other skin sites or household contacts.
- 🦠 Secondary bacterial infection from scratching.
- 🎭 Tinea incognito after inappropriate steroid use.
- 🧔 Beard involvement → think tinea barbae.
- 💇 Scalp involvement, broken hairs, or kerion → think tinea capitis.
- 👶 Children with scalp disease, or adults with extensive/refractory disease, may need specialist input.
📊 Prognosis
✅ Most localised cases respond well to topical antifungals. ♻️ Recurrence is common if the source persists (for example infected feet, nails, contacts, or pets). More extensive disease or infection involving hair-bearing skin often needs longer or systemic treatment.
📌 Summary
Tinea corporis = annular, scaly dermatophyte infection of the body. Tinea faciei = the same process on the face. 🔑 Diagnosis: usually clinical, but send scrapings if uncertain or recurrent. 💊 Treatment: topical terbinafine first-line for localised disease; oral therapy if extensive, refractory, or involving beard/scalp. ⚠️ Do not use steroid cream alone.
🖼️ Typical annular lesions:
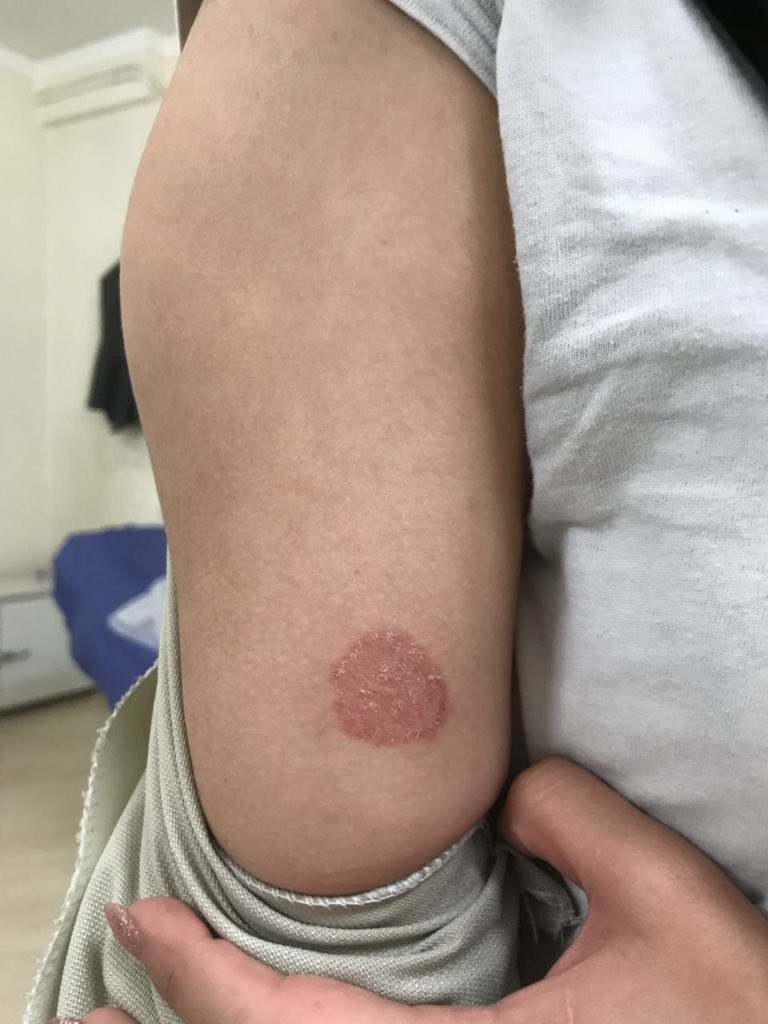
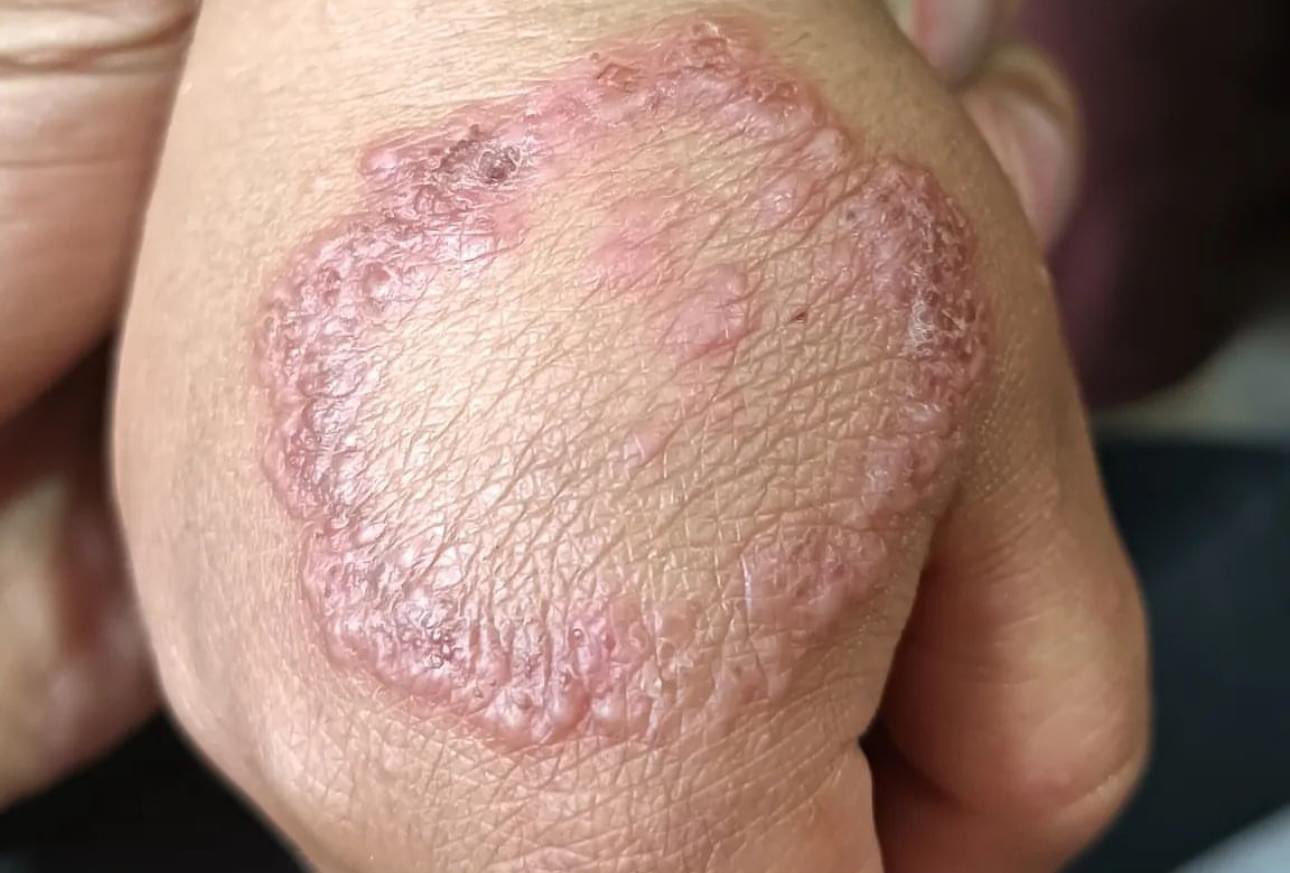
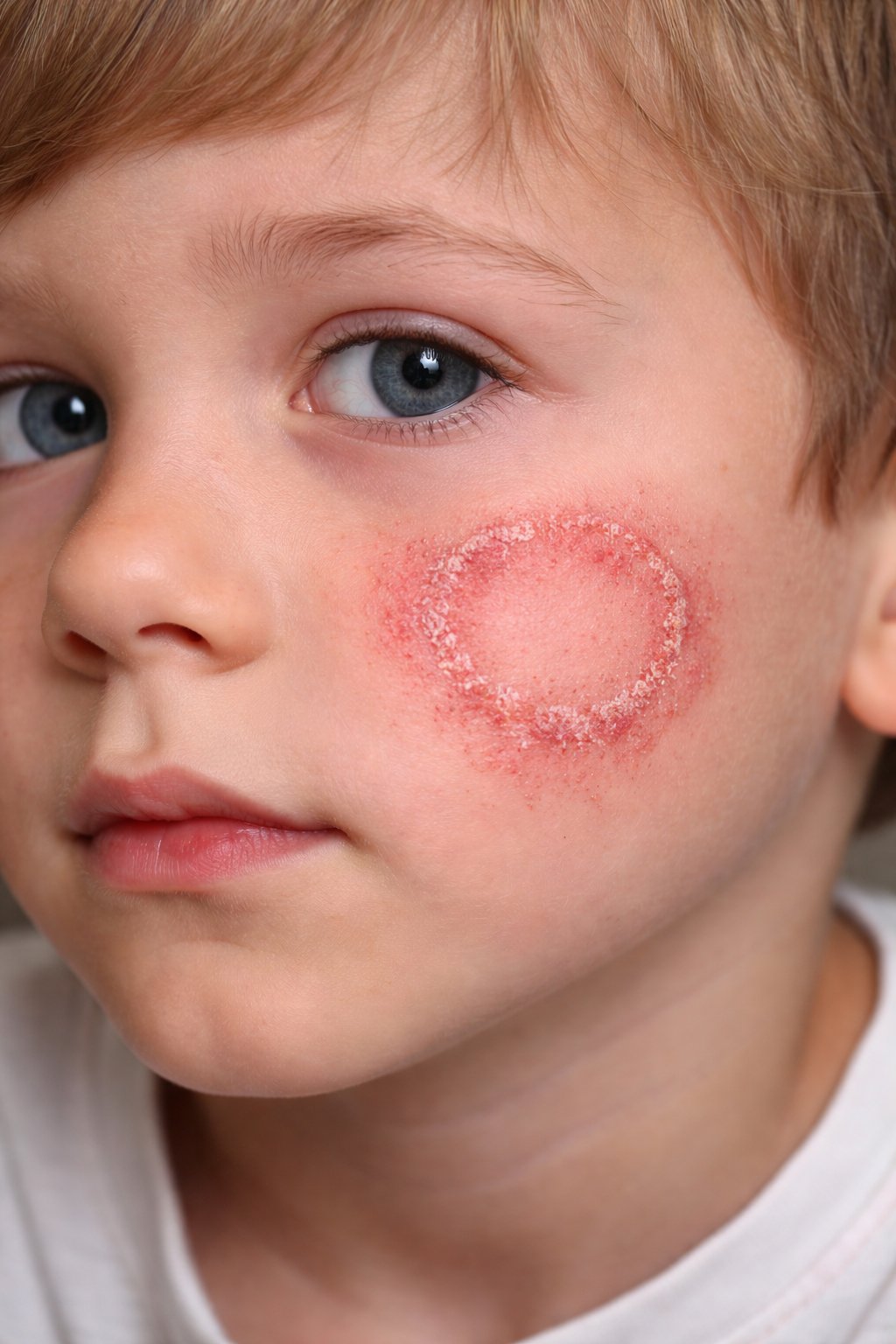
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
