| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Acute Disc Prolapse
Related Subjects: |Transverse myelitis |Acute Disseminated Encephalomyelitis |Cervical spondylosis |Spinal Cord Anatomy |Acute Disc Prolapse |Spinal Cord Compression |Spinal Cord Haematoma |Foix-Alajouanine syndrome |Cauda Equina |Conus Medullaris syndrome |Anterior Spinal Cord syndrome |Central Spinal Cord syndrome |Brown-Sequard Spinal Cord syndrome |Internal Decapitation
🧾 About
- Acute Disc Disease: 💥 Often presents with partial spinal cord symptoms, particularly in older adults following trauma (e.g., a fall).
- Central disc herniation can compress the cauda equina (LMN signs 🦵), while lateral herniations usually impact specific nerve roots.
- Disc prolapse is more common in younger individuals due to higher water content in discs, but degeneration with age increases risk in older patients.
🧬 Aetiology
- The disc herniates backward through a tear in the annulus fibrosus, with the nucleus pulposus protruding into the spinal canal.
- This can compress:
- Spinal cord → producing UMN signs (spasticity, brisk reflexes, Babinski).
- Cauda equina → producing LMN signs (flaccid paralysis, areflexia, saddle anaesthesia).
- Nerve root → leading to radiculopathy with focal weakness, numbness, and dermatomal pain.
⚠️ Causes
- Acute trauma (falls, heavy lifting, twisting injuries).
- Chronic degeneration from age-related disc dehydration and narrowing of intervertebral spaces.
- Repetitive strain or poor lifting techniques in manual labour.
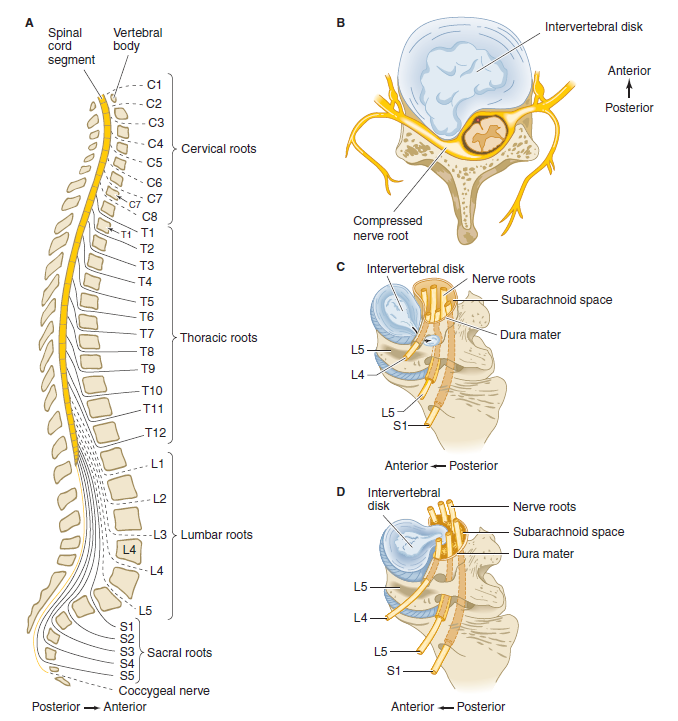
🩺 Clinical Presentation
- Sudden, severe lumbar back pain often after a specific movement (e.g., bending, coughing, sneezing).
- Protective muscle spasm causing a tilted posture or reduced mobility.
- Pain typically radiates down the leg (sciatica) and worsens with movement. Most commonly involves L4/5 or L5/S1 discs.
- Central lesions → risk of cauda equina syndrome (urinary retention, saddle anaesthesia, bilateral leg weakness 🚨).
- Lateral lesions → radicular pain and weakness in a dermatomal/myotomal pattern.
🧪 Neurological Findings by Nerve Root
- S1: Pain buttock → calf → sole of foot, sensory loss in sole/calf, weak plantar flexion, absent ankle jerk.
- L5: Pain buttock → lateral leg → dorsum of foot, weak dorsiflexion (foot drop), ↓ straight-leg raise.
- L4: Pain lateral thigh → medial calf, sensory loss calf, ↓ knee reflex, positive femoral stretch test.
🔍 Investigations
- Blood tests: FBC, U&E, ESR/CRP, ALP, phosphate, calcium → exclude infection/malignancy.
- MRI spine: Gold standard for confirming disc prolapse, nerve root compression, or cauda equina features.
- CT spine: Alternative if MRI is contraindicated, though less sensitive for soft tissue lesions.
💊 Management
- Conservative: Analgesia (NSAIDs, opioids if severe), firm mattress, stay active (bed rest discouraged).
- Physiotherapy: Once pain settles → restore mobility, improve core strength, correct posture.
- Corticosteroid injections: Can reduce inflammation in persistent radicular pain.
- Surgical referral 🚨: Urgent if red flag symptoms (bladder dysfunction, saddle anaesthesia, progressive motor weakness) → possible decompression/discectomy.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
