| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Malignant MCA syndrome ✅
Related Subjects: |Acute Stroke Assessment (ROSIER&NIHSS) |Causes of Stroke |Ischaemic Stroke |Cancer and Stroke |Cardioembolic stroke |CT Basics for Stroke |Acute Hydrocephalus
🧠 Introduction
- ⚡ Malignant MCA syndrome occurs after a large MCA territory infarct, leading to massive cerebral oedema and risk of herniation.
- 🕐 Typically presents 2–5 days post-stroke, but severe oedema can develop within 24h.
- 🔍 Pathophysiology: cytotoxic oedema → midline shift → raised ICP → risk of transtentorial herniation.
- 📊 Clinical trials demonstrate that early decompressive surgery reduces mortality; survivors often have significant disability (mRS 4–5).
🧬 Aetiology
- 🫀 Large vessel atheroembolism (MCA stem or ICA terminus).
- 💓 Cardioembolism (atrial fibrillation, valvular disease, LV thrombus).
- 🩸 Carotid or MCA dissection → embolism to MCA territory.
🩺 Clinical Presentation
- Contralateral hemiparesis, hemianopia, hemisensory loss ± aphasia/neglect (depends on dominant hemisphere involvement).
- Progressive decline in consciousness due to mass effect and raised ICP.
- Late signs: ipsilateral pupillary dilatation, Cheyne-Stokes respiration, signs of uncal or transtentorial herniation.
🖼️ Imaging
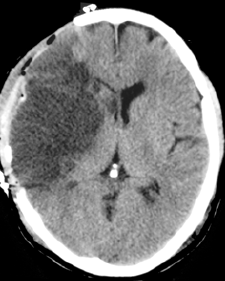
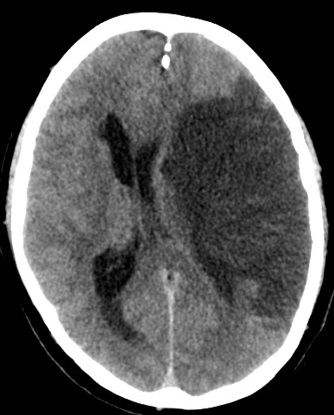
- CT Head: May be normal early; later shows hypodensity >50% MCA territory, mass effect, midline shift, sulcal effacement.
- MRI DWI: Accurate infarct volume measurement; >145 cm³ predicts poor outcome without intervention.
- CTA: Assess vessel patency, rule out tandem ICA/MCA occlusion.
📑 RCP / NICE Guidance
Consider decompressive hemicraniectomy in adults with malignant MCA infarction if:
- Pre-stroke mRS <2 (functionally independent).
- Clinical MCA syndrome with NIHSS >15.
- Reduced consciousness (NIHSS 1a ≥1).
- Imaging: infarct >50% MCA territory or DWI volume >145 cm³.
- Age <60 yrs generally; selected patients >60 yrs may benefit (DESTINY II).
💊 Management
- 🎯 Supportive ICP measures: intubation, sedation, osmotherapy (mannitol, hypertonic saline), controlled hyperventilation – not sufficient alone.
- 🔪 Decompressive hemicraniectomy + durotomy: Large bone flap & dural opening; allows brain expansion, prevents herniation, reduces mortality.
- 👥 Patient selection: consider age, comorbidities, baseline function, patient/family wishes.
- ⚠️ Poor prognostic features: infarct extends to ACA/PCA territories, very large infarct volume, refractory ICP.
- 📊 Evidence from trials:
- HAMLET – surgery <48h ↓ mortality; delayed >96h less effective.
- DESTINY I – younger patients had marked survival benefit.
- DESTINY II – ≥60 yrs, survival benefit, but most survivors dependent (mRS 4–5).
- 🧪 Medical adjuncts: maintain normothermia, normoglycaemia, normovolaemia; seizure prophylaxis if indicated; close ICU monitoring.
📝 Exam / Student Tips
- ⚡ Recognise early malignant MCA features: massive hemiplegia, dysphasia/neglect, declining consciousness, severe headache/ICP symptoms.
- 🧠 CT hypodensity >50% MCA territory or DWI volume >145 cm³ = classic red flag for neurosurgical referral.
- 📆 Timing is critical: surgery <48h gives best survival.
- 💭 Know trial names & outcomes (HAMLET, DESTINY I/II) – common OSCE/finals knowledge point.
- 👨⚕️ Always combine imaging findings with clinical status; early discussion with neurosurgery is key.
📚 References / Evidence
| 🧪 Trial | 👨⚕️ Authors | 📊 Key Outcome |
|---|---|---|
| HAMLET (Lancet Neurol. 2009) | HAMLET investigators | Hemicraniectomy within 48h ↓ mortality; late surgery (>96h) offers minimal benefit. |
| DESTINY I (Stroke 2007) | DESTINY Study Group | Surgery markedly ↓ mortality in younger adults; trial stopped early after meta-analysis with DECIMAL & HAMLET. |
| DESTINY II (NEJM 2014) | DESTINY II Investigators | Adults ≥60 yrs: surgery ↑ survival but most survivors had severe disability (mRS 4–5). |
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
