| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Torsades de pointes TdP (Polymorphic VT)
Related Subjects: |ECG-QT interval |Brugada Syndrome |Long QT syndrome (LQTS) Acquired |Long QT syndrome (LQTS) Congenital |Torsades de Pointes |Ventricular Fibrillation |Ventricular Tachycardia |Resuscitation - Adult Tachycardia Algorithm |Automatic Implantable Cardioverter Defibrillator (AICD)
⚡ Torsades de Pointes (Polymorphic VT): Occurs in repetitive, non-sustained paroxysms but can degenerate into VF. 💉 First-line: IV magnesium 8 mmol (2 g) bolus over 10–15 mins in 50–100 ml 5% dextrose or saline. ❌ Avoid amiodarone. Correct K/Mg/Ca. Consider pacing, isoprenaline (except congenital LQTS), and defibrillation if unstable.
📖 About
- Coined by Dessertenne in 1966.
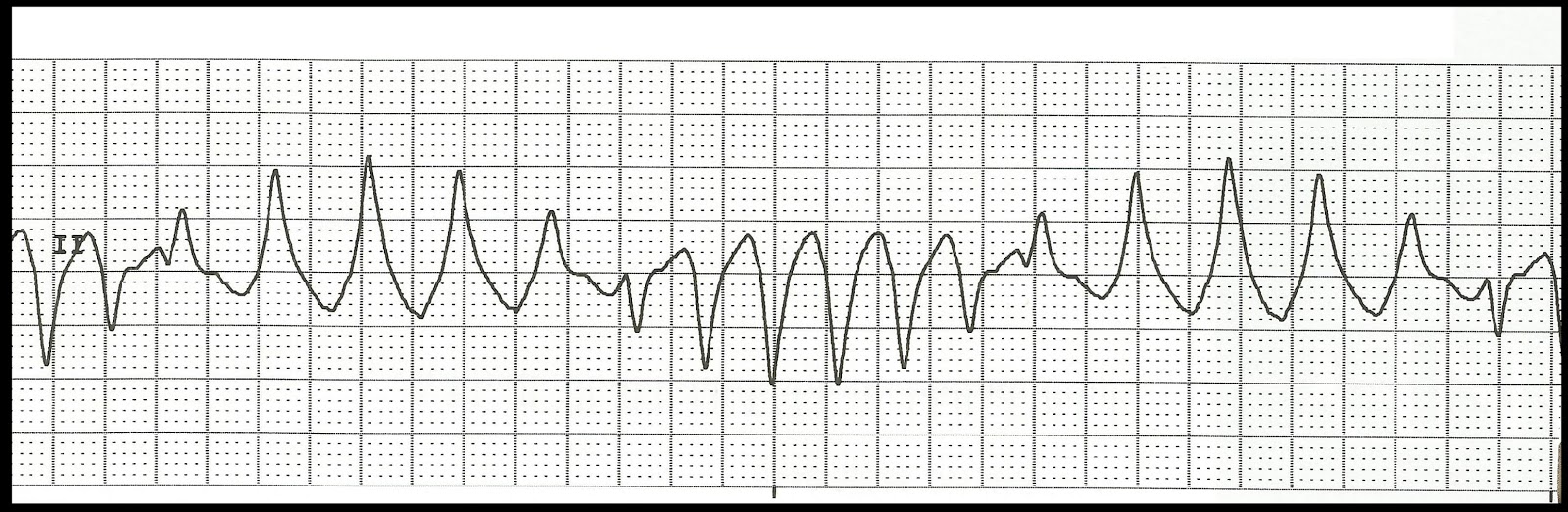
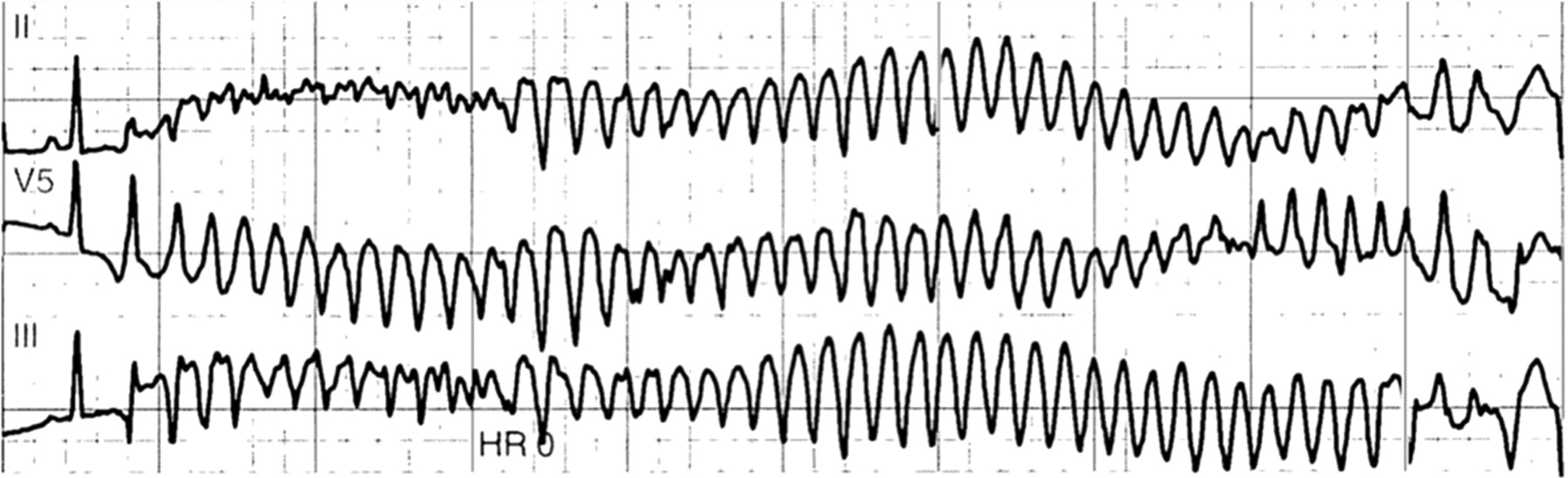
- A polymorphic ventricular tachycardia with the QRS axis “twisting around the baseline.”
- Commonly associated with prolonged QTc >460 ms.
- Drug-associated risk varies - see www.qtdrugs.org.
📌 Definition
- Polymorphic VT with continuously changing QRS axis.
- Seen in congenital or acquired Long QT syndrome.
- Often due to inhibition of the HERG potassium channel.
🖥️ Electrocardiogram
🧬 Genetics
- LQT1 & LQT2 → slow potassium channels.
- LQT3 → sodium channel defects.
- LQT4–12 → rarer subtypes.
- Congenital long QT: autosomal dominant, more pronounced in females.
📊 Epidemiology
- Females 2–3x more likely to develop TdP.
- Drug-induced QT prolongation more common in women.
🩺 Clinical
- Occurs in bursts, often self-terminating.
- Symptoms: presyncope, syncope, hypotension, pulmonary oedema.
- May deteriorate to sustained VT/VF → cardiac arrest.
⚠️ Risk Factors
- Congenital: Romano-Ward (AD), Jervell-Lange-Nielsen (AR + deafness).
- Acquired: electrolyte disorders (↓K, ↓Ca, ↓Mg), medications, bradycardia.
- Other: baseline ECG abnormalities, renal or liver impairment, female sex.
💊 Causes of Acquired Long QT
- Electrolyte/metabolic: hypokalaemia, hypocalcaemia, hypomagnesaemia, hypothyroidism, hypothermia.
- Drugs: amiodarone, disopyramide, flecainide, erythromycin, terfenadine, TCAs, quinidine, lithium, phenothiazines. 👉 Always check in BNF.
🔎 Investigations
- FBC, U&E, Mg, Ca, TFTs, troponin if ACS suspected.
- ECG: twisting QRS, prolonged QTc often >500 ms.
- Echocardiogram: rule out structural heart disease.
🛠️ Management
- Stop offending drugs (esp. amiodarone, class I/III antiarrhythmics).
- IV magnesium sulphate: 8 mmol (2 g) bolus → then 72 mmol (18 g) over 24 hrs.
- Pacing (atrial > ventricular) if bradycardia-dependent TdP.
- IV isoprenaline: useful for acquired TdP but contraindicated in congenital LQTS.
- Defibrillation if unstable.
- Congenital LQTS: beta-blockers mainstay; consider ICD or left stellate ganglion block for refractory cases.
- Acquired LQTS: beta-blockers contraindicated (bradycardia worsens risk).
📚 References
💡 Teaching Pearl: TdP is always a “red flag rhythm.” Think: correct electrolytes, stop QT-prolonging drugs, give magnesium, pace or shock if needed.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
