| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
ECG - Heart Block
Related Subjects: |ECG Basics |ECG Axis |ECG Analysis |ECG LAD |ECG RAD |ECG Low voltage |ECG Pathological Q waves |ECG ST/T wave changes |ECG LBBB |ECG RBBB |ECG short PR |ECG Heart Block |ECG Asystole and P wave asystole |ECG QRS complex |ECG ST segment |ECG: QT interval |ECG: LVH |ECG RVH |ECG: Bundle branch blocks |ECG Dominant R wave in V1 |ECG Acute Coronary Syndrome |ECG Crib sheets
🧠 In all cases: look for the cause and clinical context
- 🔍 Always look for reversible causes such as:
- ischaemia / acute myocardial infarction
- drug effects (for example beta-blockers, digoxin, verapamil, diltiazem, amiodarone)
- electrolyte disturbance, especially hyperkalaemia
- hypothyroidism
- infection, hypothermia, raised vagal tone, or post-cardiac procedure conduction injury
- 💊 If drugs are contributing and the patient is symptomatic, reduce or stop them where appropriate.
- 🚑 If bradycardia is causing compromise, give atropine 500 micrograms IV; repeat if needed to a maximum of 3 mg.
- ⚠️ If there are life-threatening features or a high risk of asystole, seek urgent senior help and prepare for pacing and/or vasoactive support.
- 🔌 A pacemaker is the definitive treatment for many persistent or high-risk bradyarrhythmias, especially when the block is not readily reversible.
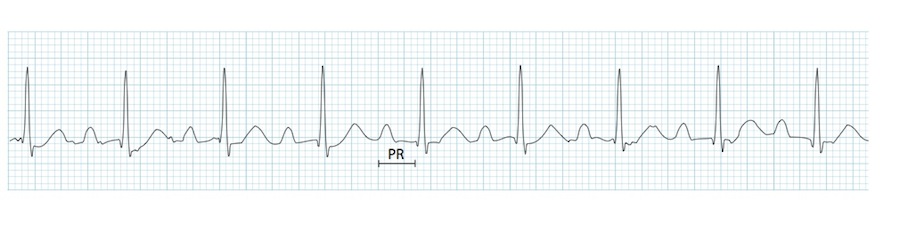
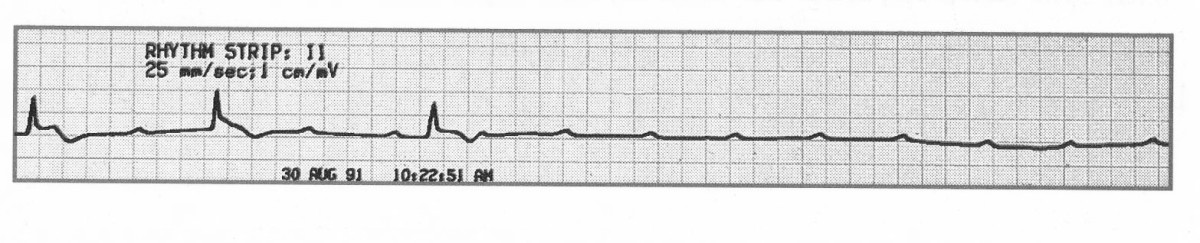
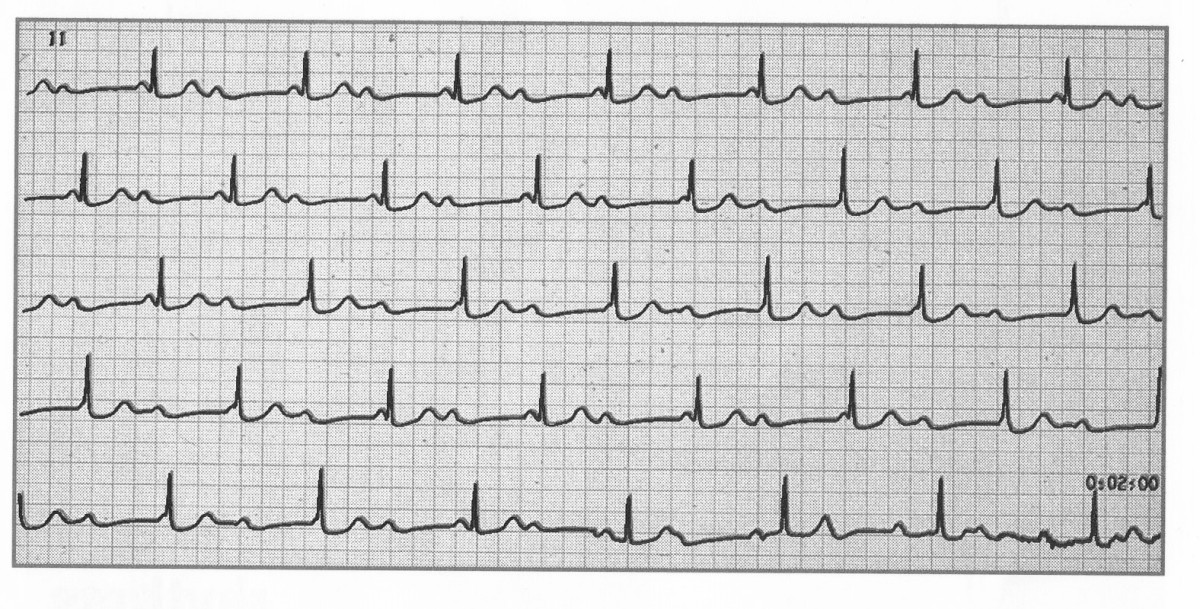
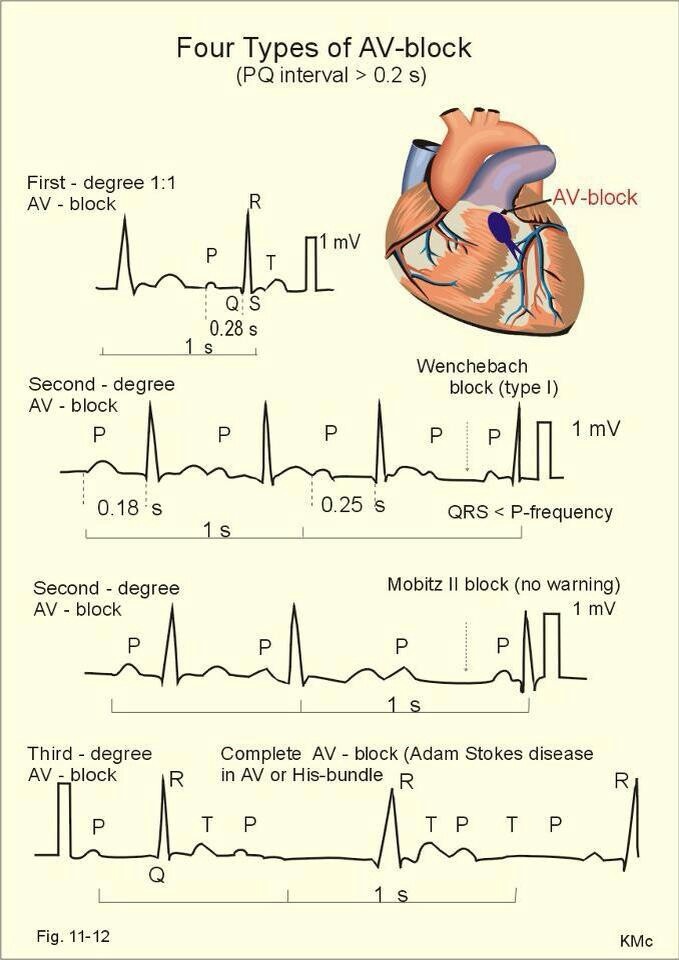
🟢 First-degree AV block
- Definition: delayed AV conduction with a PR interval > 0.20 seconds, but every P wave is still followed by a QRS complex.
- Rate: can occur with either sinus bradycardia or sinus tachycardia.
- Rhythm: sinus rhythm, regular.
- PR interval: prolonged and fixed.
- P waves: normal morphology; every P wave is followed by a QRS, and every QRS is preceded by a P wave.
- QRS: usually narrow unless there is additional intraventricular conduction disease.
- 😊 Usually not clinically significant and often requires no specific treatment.
- ⚠️ Important exception: progressive PR prolongation in infective endocarditis can suggest an aortic root abscess.
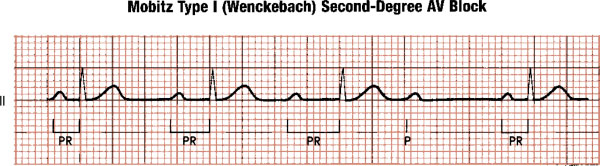
🟡 Mobitz type I (Wenckebach)
- Definition: progressive prolongation of the PR interval until a P wave is not followed by a QRS complex.
- Atrial rhythm: regular.
- Ventricular rhythm: irregular because of the dropped beats.
- PR interval: lengthens progressively from beat to beat, then one beat is dropped.
- P waves: normal in shape; occasional P wave not conducted.
- QRS: usually narrow, suggesting nodal-level block.
- 📍 This is often an AV nodal block and can be seen in healthy people, athletes, or with high vagal tone.
- 😊 It often does not require pacing unless it causes significant symptoms or occurs in a concerning clinical context.
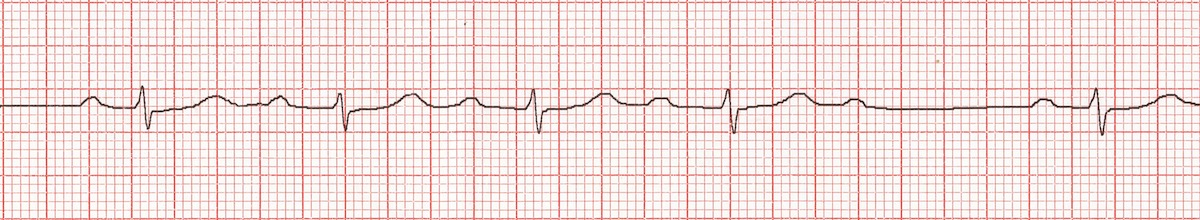
🟠 Mobitz type II
- Definition: intermittent non-conducted P waves without progressive PR prolongation.
- Atrial rate: usually regular.
- Ventricular rate: slower than the atrial rate because some impulses are blocked.
- Rhythm: atrial rhythm regular; ventricular rhythm may be irregular because of dropped beats.
- PR interval: constant in conducted beats.
- P waves: normal morphology, but some are not followed by QRS complexes.
- QRS: may be narrow or wide; a wide QRS suggests more distal conduction system disease and higher risk.
- ⚠️ More serious than Mobitz I because it can progress to complete heart block or asystole.
- 🔌 Management usually involves urgent specialist review and often pacing, unless there is a clearly reversible cause.
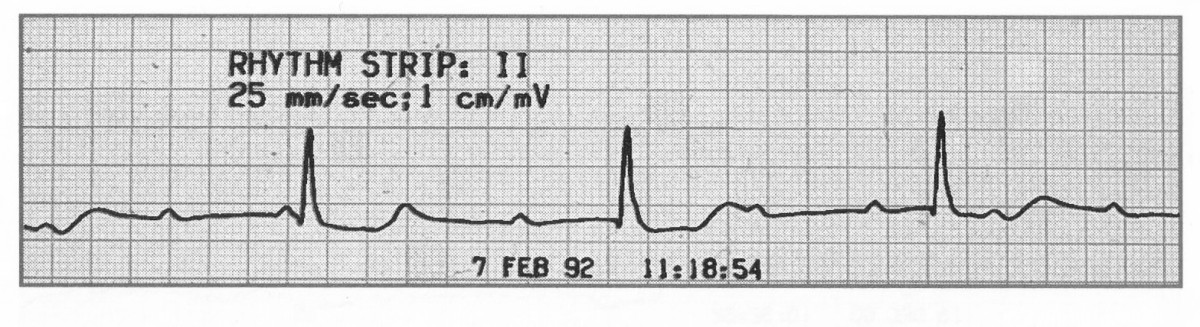
🔴 Third-degree (complete) heart block
- Definition: complete failure of AV conduction, so the atria and ventricles beat independently (AV dissociation).
- Atrial rate: usually determined by the sinus node and often 60–100 bpm.
- Ventricular rate: maintained by an escape rhythm and is usually slower.
- Rhythm: atrial rhythm and ventricular rhythm are both regular, but there is no relationship between them.
- PR interval: variable, because P waves and QRS complexes are dissociated.
- P waves: normal and regular.
- QRS: narrow if the escape rhythm is junctional; broad if ventricular, which is generally more unstable.
- 🚨 This may occur acutely, for example after myocardial infarction, and can sometimes be reversible depending on the cause and site of block.
- ⚠️ In symptomatic patients, this is a medical emergency and usually requires temporary pacing followed by assessment for a permanent pacemaker if the cause is not reversible.
💡 Practical clinical pearls
- 🩺 Not all AV block needs pacing, but Mobitz II and complete heart block should always be taken seriously.
- 📉 A broad-QRS complete heart block is especially high risk because it implies more distal conduction system disease.
- 💉 Atropine may help nodal bradycardia, but is often less effective in distal infranodal block.
- 🔍 Always ask: Is there a reversible cause?
- 🚑 If the patient is shocked, syncopal, ischaemic, or in heart failure, escalate early for pacing support.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
