| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Cerebral Venous Thrombosis (CVT)
Related Subjects: Thrombophilia testing |Antiphospholipid syndrome |Protein C Deficiency |Protein S Deficiency |Prothrombin 20210A mutation |Factor V Leiden Deficiency |Antithrombin III deficiency (AT3) |Cerebral Venous Sinus thrombosis |Budd-Chiari syndrome |Acute Hydrocephalus
🧠 Cerebral Venous Thrombosis (CVT) is an under-recognised cause of stroke, especially in young adults, postpartum women, and patients with prothrombotic conditions. ⚠️ Postpartum period is a major risk factor, and CVST has also been reported rarely in association with COVID-19 vaccination + thrombocytopenia. Clues: persistent headache, papilloedema, seizures, or infarcts not in arterial territories.
📖 About
- Likely underdiagnosed; many cases are missed or treated late.
- Headache + papilloedema + normal CT should raise suspicion.
- Think of CVST in pregnant/postpartum women or patients with prothrombotic risk factors.
⚙️ Aetiology (Causes)
- 💊 OCP use, pregnancy, postpartum period.
- 💉 Procoagulant states: Factor V Leiden, protein C/S deficiency, antithrombin deficiency, prothrombin mutation, hyperhomocysteinaemia.
- 🩸 Haematological: polycythaemia, thrombocythaemia, leukaemia, sickle cell disease.
- 🦠 Infections: mastoiditis, otitis media, sinusitis, bacterial meningitis.
- 🧬 Systemic conditions: Behçet’s, SLE, ulcerative colitis, Crohn’s, APS, Graves’ disease.
- ⚡ Drugs: Ecstasy (MDMA), chemotherapy.
- 🦴 Trauma/neurosurgery near venous sinuses.
- 🦠 Malignancy: adenocarcinomas, haematological cancers.
- 💉 Post-COVID-19 vaccine (rare): CVST with thrombocytopenia/VITT.
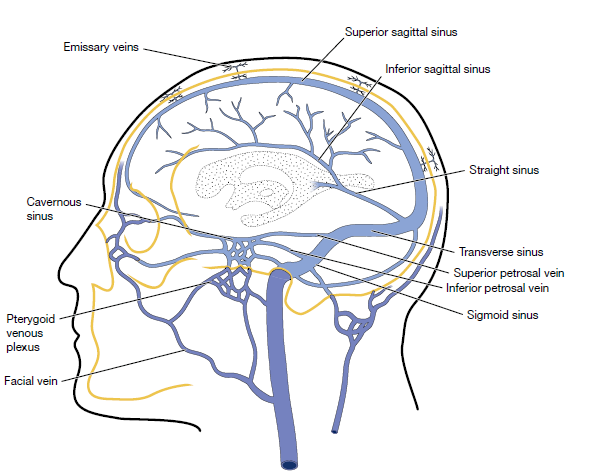
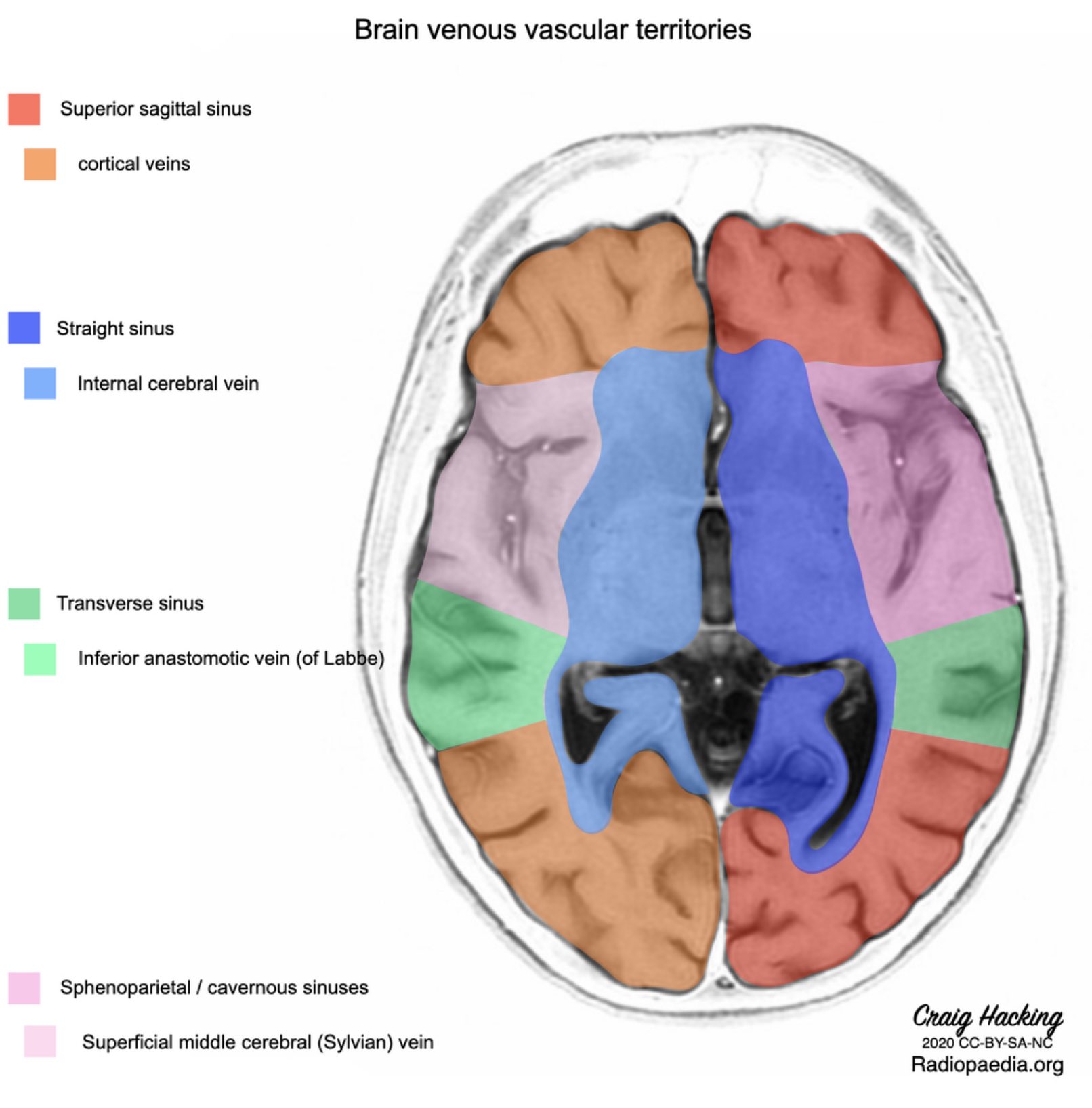
🧭 Venous Anatomy
CVST can affect any venous sinus or cortical vein, leading to raised ICP and venous infarction.
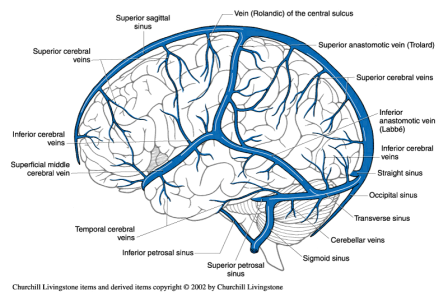
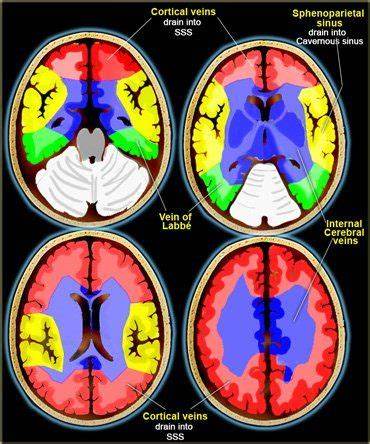
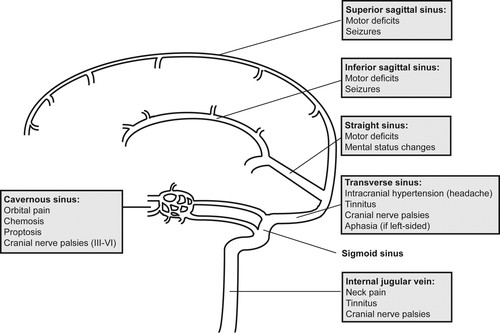
🩸 Common Sites & Clinical Patterns
- Superior sagittal sinus: raised ICP, headache, papilloedema.
- Lateral/straight sinus, vein of Galen: bilateral thalamic infarcts → akinetic mutism.
- Small cortical veins: focal cortical signs, seizures.
- Cavernous sinus: cranial neuropathies, proptosis, cavernous sinus syndrome.
🔬 Pathophysiology
- Obstruction of venous outflow → venous congestion, cytotoxic + vasogenic oedema.
- Haemorrhagic venous infarction due to capillary rupture.
- ↓ CSF absorption via arachnoid granulations → raised ICP.
- Subarachnoid haemorrhage may occasionally occur.
🩺 Clinical Presentation
- 💢 Headache in ~90% (often progressive, worse lying down).
- 🌡️ Raised ICP: papilloedema, nausea, vomiting, sixth nerve palsy.
- ⚡ Seizures: focal or generalised (much more common than in arterial stroke).
- 🧑⚕️ Focal neurology: hemiparesis, aphasia, cortical signs.
- 🤒 Cavernous sinus thrombosis: ophthalmoplegia, cranial nerve palsies, facial pain.
- 🌀 Atypical: psychosis, encephalopathy, TIA-like symptoms, migraine-like headache.
🧾 Differential Diagnosis
- Idiopathic intracranial hypertension (IIH): important mimic, especially in young obese women. ➡️ If male or non-obese, always exclude CVST.
🔍 Investigations
- 🩸 FBC: Look for thrombocytopenia (consider VITT, HIT, leukaemia).
- 🧪 D-dimer: Usually raised but not fully sensitive.
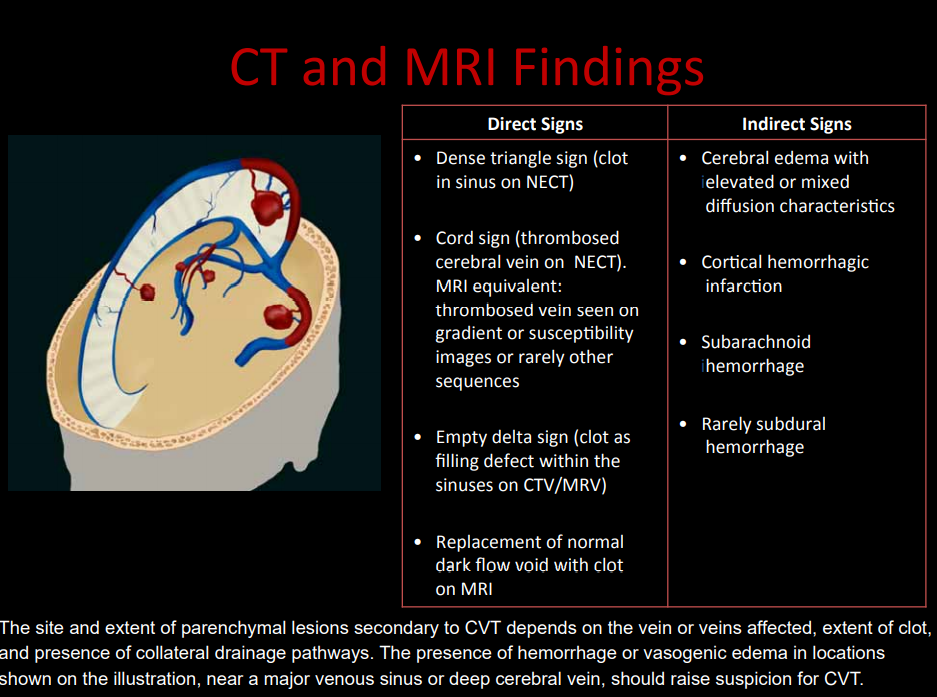
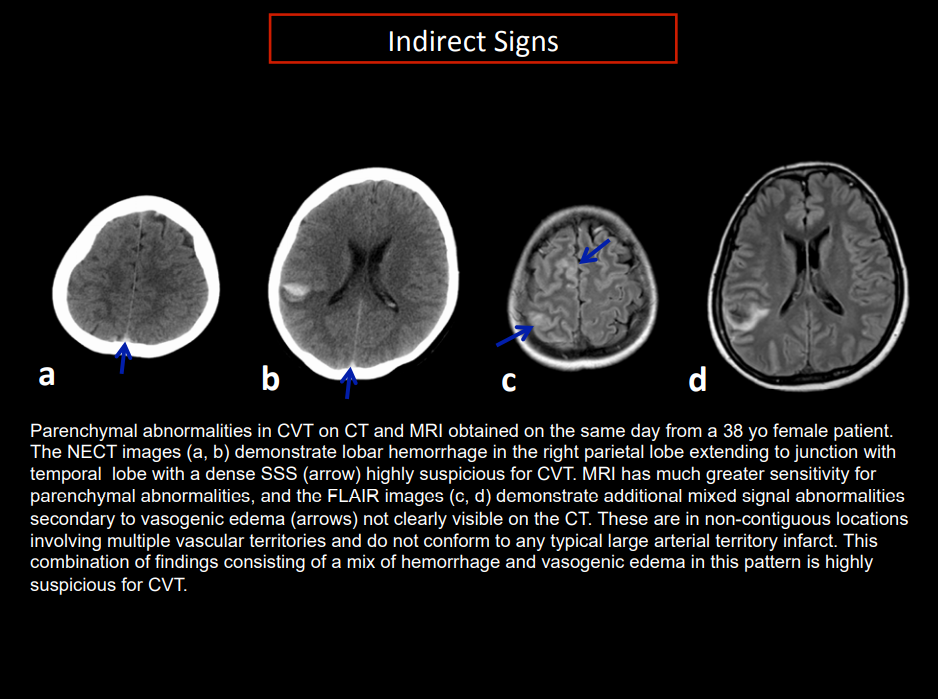
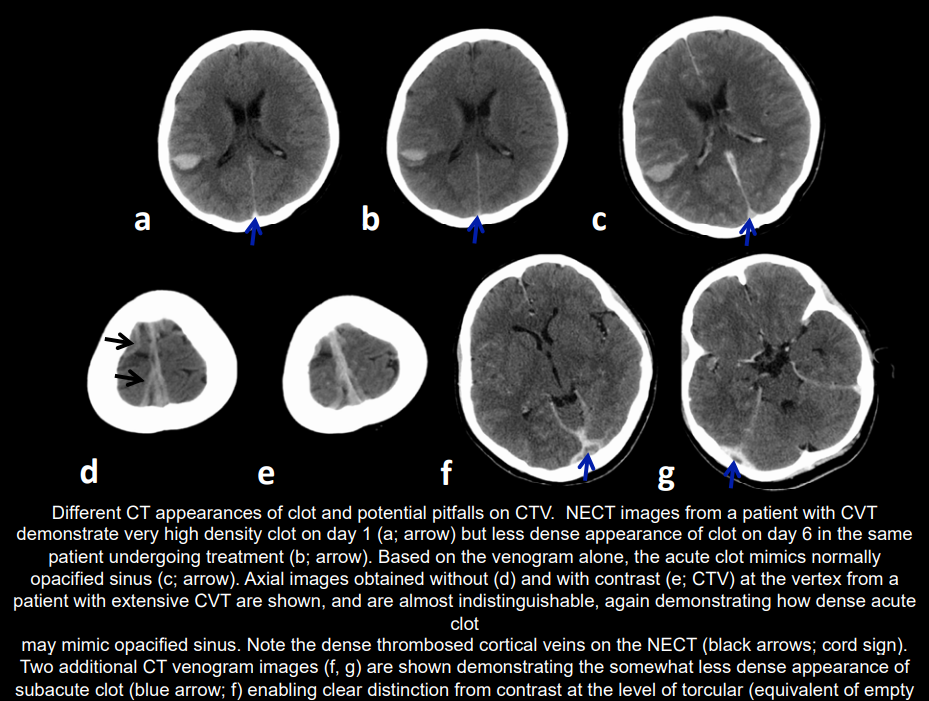
- 🖼️ CT (plain): May be normal; may show haemorrhagic infarcts not in arterial territories. "Cord sign" (fresh clot), SAH possible.
- 🩻 CT venography: "Empty delta sign" (contrast around clot in sagittal sinus).
- 🧲 MRI/MRV: Best modality. Detects venous clot, oedema, infarction, haemorrhage.
- 💉 CSF: ↑ opening pressure, ↑ protein; WCC mildly raised.
- 🧬 Thrombophilia screen: Factor V Leiden, prothrombin G20210, protein C/S deficiency, antithrombin deficiency, homocystinuria.
 alt="CT Venous Image 1"
style="display:block; width:100%; max-width:100%; height:auto; margin:10px auto; border-radius:8px;">
alt="CT Venous Image 1"
style="display:block; width:100%; max-width:100%; height:auto; margin:10px auto; border-radius:8px;">
📉 Prognosis Factors
- Deep venous involvement → poor prognosis (bilateral thalamic infarcts).
- Male sex associated with worse outcomes.
- Right lateral sinus thrombosis carries higher risk.
🧬 Inherited Procoagulant Conditions (approx. prevalence)
- Factor V Leiden: 3–7%.
- Prothrombin G20210 mutation: 1–2%.
- Protein C deficiency: 0.3%.
- Protein S deficiency: 0.1%.
- Antithrombin deficiency: 0.02%.
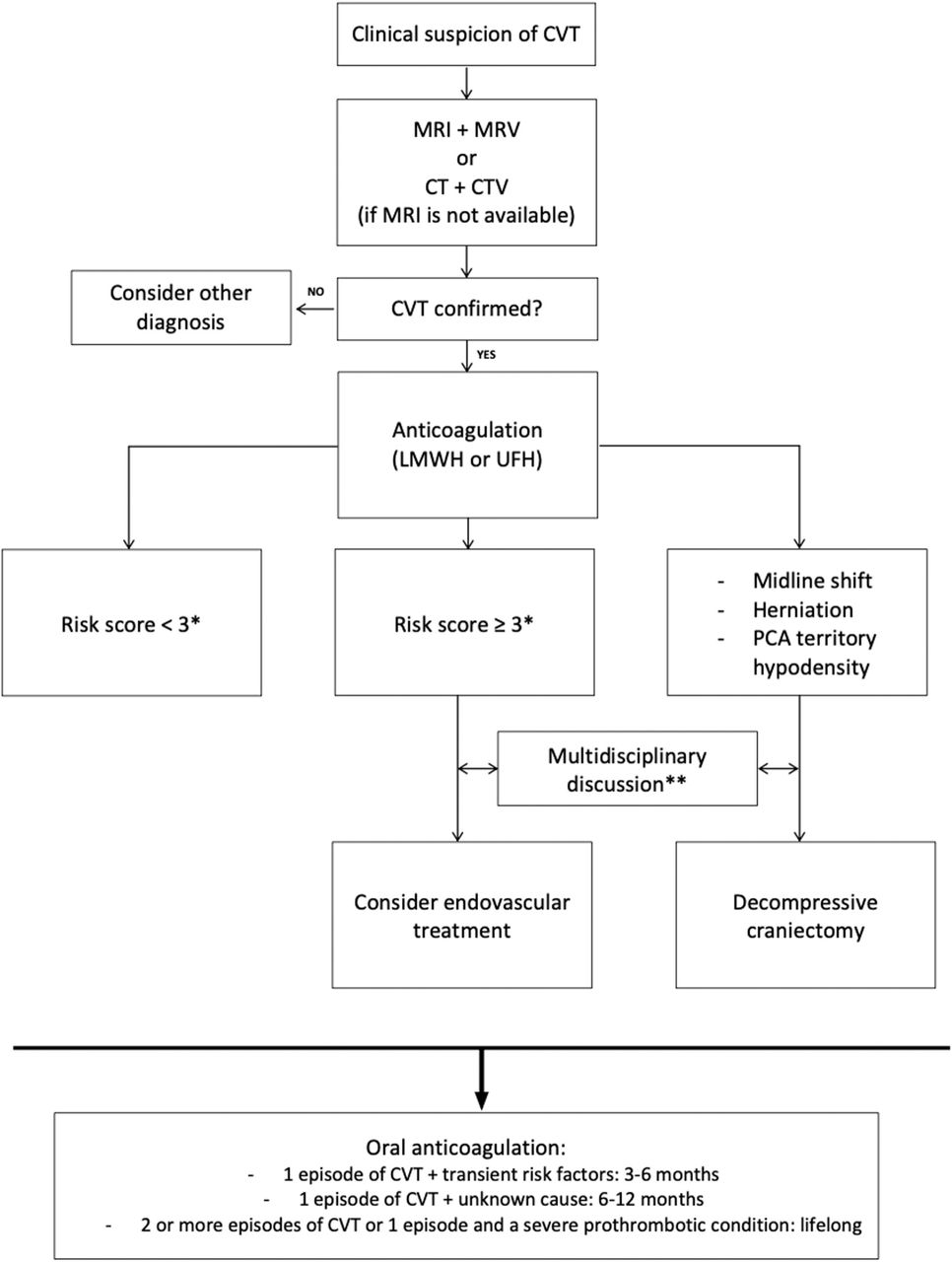
⚖️ Management
- 💉 Anticoagulation is the cornerstone: LMWH preferred (BID dosing). UFH if renal failure or rapid reversal required.
- 🩸 Even with haemorrhagic venous infarcts, anticoagulation is not contraindicated.
- 🔄 Oral anticoagulation (warfarin, INR 2–3) for 3–12 months; longer if recurrent or idiopathic.
- ⚡ Endovascular thrombolysis/thrombectomy: for severe/refractory cases in expert centres.
- 📉 COVID-19 related (VITT): avoid heparin, use IVIG + non-heparin anticoagulants (e.g., argatroban, fondaparinux) per guidelines.
- 🧑⚕️ Supportive: ICP management (acetazolamide, CSF drainage if needed), seizure prophylaxis if recurrent.

📚 References
- Cerebral venous thrombosis: a practical guide. Pract Neurol 2020.
- Imaging Approach to CVST – CAR.
- Piazza G. Circulation 2012;125:1704–1709.
- ACC: CVST with Vaccine-Induced Thrombocytopenia.
💡 Exam Pearls:
– CVST = young woman + headache + seizures + haemorrhagic infarct not in arterial territory.
– Always request CT/MR venography if suspicion is high.
– Anticoagulation is safe, even with haemorrhage.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
