| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Idiopathic Intracranial hypertension ✅
Related Subjects: |Brain tumour s |Astrocytomas |Brain Metastases |Tuberous sclerosis |Turcot's syndrome |Lhermitte Duclos Disease |Oligodendroglioma |Acute Hydrocephalus |Intracranial Hypertension |Primary CNS Lymphoma (PCNSL)
Idiopathic Intracranial Hypertension (IIH), aka Pseudotumour Cerebri, is raised intracranial pressure (ICP) without structural cause. ⚠️ Despite “benign” terminology, untreated IIH may cause permanent visual loss due to papilloedema.
ℹ️ Key Points
- Most common in young, obese females 📈.
- Mimics a brain tumour clinically & radiologically.
- Visual field defects: early blind spot enlargement, inferonasal loss 👁️.
🧬 Aetiology & Associations
- Impaired CSF absorption at arachnoid granulations.
- Cerebral venous sinus thrombosis must be excluded 🚨.
- Associated factors: pregnancy, OCP, thrombophilia.
- Drugs 💊: Vitamin A/retinoids, tetracyclines, growth hormone, nitrofurantoin, danazol, lithium.
- Other substances: ketamine, nitrous oxide.
🩺 Clinical Presentation
- Headache: morning-predominant, worse lying down, eased by ICP reduction.
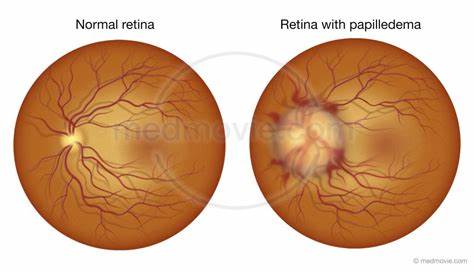
- Visual: transient obscurations, blurred vision, papilloedema, visual field loss.
- Other: diplopia (CN VI palsy), pulsatile tinnitus, neck/back pain.
- Often history of recent weight gain ⚖️ or new medication exposure.
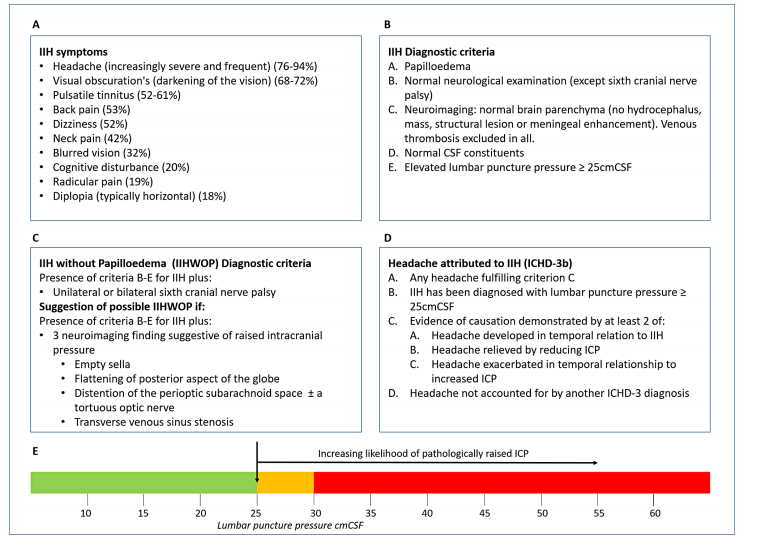
🔬 Investigations
- Bloods: FBC, U&E, LFT, ESR, CRP to exclude systemic causes.
- Visual field testing: blind spot enlargement, inferonasal defects.
- Imaging: MRI/MRV to exclude mass/venous thrombosis; may show empty sella, enlarged optic nerve sheath.
- LP: Elevated opening pressure (>25 cm H₂O) with normal CSF constituents.
📑 Diagnostic Criteria (Modified Dandy)
|
🧾 Differentials
- Cerebral venous sinus thrombosis
- Intracranial mass (tumour, abscess)
- Hydrocephalus
🎯 Management Goals
- Rule out venous sinus thrombosis.
- Preserve vision 👁️.
- Reduce ICP and control headache burden.
💊 Management
- Stop offending drugs (tetracyclines, retinoids, steroids, nitrofurantoin).
- Weight loss: 5–10% reduction lowers ICP; bariatric surgery if needed.
- Medical therapy:
- Acetazolamide – first-line, reduces CSF production.
- Topiramate – alternative, also promotes weight loss.
- Loop diuretics (e.g., furosemide) – selected cases.
- Steroids – rarely used; risk of rebound ICP on withdrawal.
- Surgical therapy:
- Optic nerve sheath fenestration – for threatened vision.
- CSF diversion (VP or LP shunt) – refractory cases.
- Venous sinus stenting – emerging therapy for stenosis-related IIH.
💡 Exam Pearls
Think “young obese woman with headache + papilloedema + raised LP opening pressure.” 👉 Always exclude venous sinus thrombosis first. 👉 First-line treatment = weight loss + acetazolamide.
📚 References & Guidelines
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
