| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Carotid sinus massage
⚠️ Always assess stroke risk before CSM - exclude carotid stenosis with Doppler ultrasound first. Perform in a monitored setting with full resuscitation backup.
📖 About
- Requires a quiet, warm room 🌡️
- Attach ECG 📈 and BP monitoring equipment
- Resuscitation equipment at hand 🛟
🛠️ Technique
- Apply gentle pressure to the right carotid sinus for ~5 seconds
- Observe for HR and BP changes
- Repeat on the left carotid
- Repeat with patient tilted to 70° (upright) ↔️
📊 Monitoring
- Positive = pause ≥3 sec (cardioinhibitory) ⚡ OR systolic BP drop ≥50 mmHg (vasodepressor)
- Mixed type shows both responses
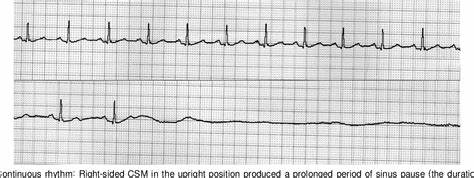
⚠️ Cautions
- Small risk of stroke/TIA → avoid if recent event or significant carotid stenosis 🚫
- Avoid in recent MI ❤️ or significant arrhythmias
- Drugs (digoxin, diltiazem, beta-blockers) may exaggerate sensitivity 💊
- Consider repeating test off drugs if safe
🛟 Immediate Management (if syncope)
- Lay patient flat 🛏️
- Raise legs 🦵 to improve cerebral perfusion
- Give oxygen if hypoxic
💡 Clinical Pearl:
CSM should only be done in a controlled setting.
A “positive” test (pause ≥3 sec or BP drop ≥50 mmHg) + reproduction of symptoms = diagnostic.
📚 Case Example
👴 An 82-year-old man with recurrent unexplained falls undergoes CSM under ECG/BP monitoring. On right-sided massage, he develops a 4-second sinus pause ⚡ with presyncope. ✅ Diagnosis: Carotid sinus hypersensitivity (cardioinhibitory). 🛠️ Plan: Lifestyle advice (avoid tight collars), review medications, pacemaker considered 💓.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
