| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Hyperacute Stroke Care Pathway
Related Subjects: |Acute Stroke Assessment (ROSIER&NIHSS) |Atrial Fibrillation |Atrial Myxoma |Causes of Stroke |Ischaemic Stroke |Cancer and Stroke |Cardioembolic stroke |CT Basics for Stroke |Endocarditis and Stroke |Haemorrhagic Stroke |Stroke Thrombolysis |Hyperacute Stroke Care
Introduction
- ⏱️ The overriding concept in hyperacute care is that "time is brain." Rapid assessment and intervention are crucial. There are two main patient streams:
- 🚀 Those suitable for urgent, active therapies.
- 🛏️ Those needing general physiological support and prevention of complications.
- Urgent therapies include:
- 💉 Stroke Thrombolysis and 🩻 Mechanical Thrombectomy.
- 🛑 Reversal of anticoagulation in intracerebral haemorrhage (ICH).
- 🧠 Decompression or external ventricular drainage (EVD) for malignant swelling or hydrocephalus.
⏱️ Time is Brain: Every minute of untreated large vessel stroke costs ~1.9 million neurons. Target: CT within 1 hour and thrombolysis within 30 minutes of arrival.
Hospital Care
- 👩⚕️ Stroke-trained staff should rapidly assess patients. Immediate CT is essential for management direction.
- 🎯 Aim for thrombolysis within 20 minutes of arrival by:
- 👋 Greeting patient and taking paramedic handover.
- 🕒 Establishing time of onset and contraindications (esp. anticoagulation).
- 💻 Booking on systems while history/exam done en route to CT.
- 📊 Post-CT: confirm BP, verify weight, and run quick checklist before Alteplase.
- 🔄 Continuous pathway improvement helps reduce door-to-needle times.
| Actions | Comments |
|---|---|
| 🫁 ABC | Airway, breathing, circulation first. Oxygen only if hypoxic. Consider ITU if GCS < 9. Record NIHSS score. |
| 🩸 Blood Glucose | Treat hypoglycaemia immediately (fingerstick test acceptable). |
| 💉 Assess for Thrombolysis | rt-PA within 3 h (>80y) or 4.5 h (<80y). Door-to-needle target: <30 min. |
| 🩻 Assess for Thrombectomy | Mechanical thrombectomy if CTA shows LVO. Best <6 h, can extend to 16–24 h in select cases. |
| 🧠 Haemorrhage / Raised ICP | Consult neurosurgery. Consider EVD, sub-occipital craniectomy (cerebellar bleed), or hemicraniectomy (malignant MCA). |
| 🧪 Haemorrhage with Coagulopathy | Reverse anticoagulation: PCC + Vit K (Warfarin), Praxbind (Dabigatran), platelets if thrombocytopenia. |
Key Information for Thrombolysis/Thrombectomy Referral
| Actions | Comments |
|---|---|
| 👶/👵 Age | <80y → 4.5h window; ≥80y → 3h window. |
| 🕒 Time Since Last Well | Use last well time if onset unclear. |
| 💊 Anticoagulation | Contraindicates thrombolysis ❌ but not thrombectomy ✔️. |
| 📊 NIHSS Score | Reperfusion rarely offered if NIHSS <4 (minor) or >25 (very severe). |
| 🏃 Premorbid State | Benefit less likely if already mRS 4–5 (high dependency). |
| 🩻 CT Report | Avoid referral if CT shows haemorrhage, tumour, or extensive infarction. |
| ⚕️ Comorbidities | Advanced malignancy / recent trauma may contraindicate treatment. |
| 🩺 Blood Pressure | Must be <185/110 mmHg before Alteplase. |
Managing and Preventing Early Complications
| Managing & Preventing Early Complications | |
|---|---|
| 🥤 Swallow Assessment | Screen within 4 h to prevent aspiration pneumonia. |
| 🍽️ Feeding | NG tube if swallow unsafe. |
| 🦵 VTE Prevention | IPC stockings first-line. Avoid LMWH until ICH excluded. |
| 💧 Hydration | IV fluids to prevent dehydration. |
| 🛏️ Skin Care | Regular turns to prevent pressure sores. |
| 🚽 Bowel Care | Prevent constipation. |
| 💪 Shoulder Protection | Support joint to avoid subluxation. |
| 🏃 Therapy | Early mobilisation & rehabilitation. |
| ⚡ Seizure Management | Treat promptly; seizures may indicate large infarct. |
| 🦠 Infection | Treat UTIs & chest infections early. |
| 💧 Bladder Care | Promote continence; avoid catheters if possible. |
📊 Exam pearls: - BP must be <185/110 before thrombolysis. - Hypo- or hyperglycaemia worsens outcome. - Seizures at onset → consider stroke mimic. - Swallow screen within 4 h is a national quality standard.
Schematic of a Pathway
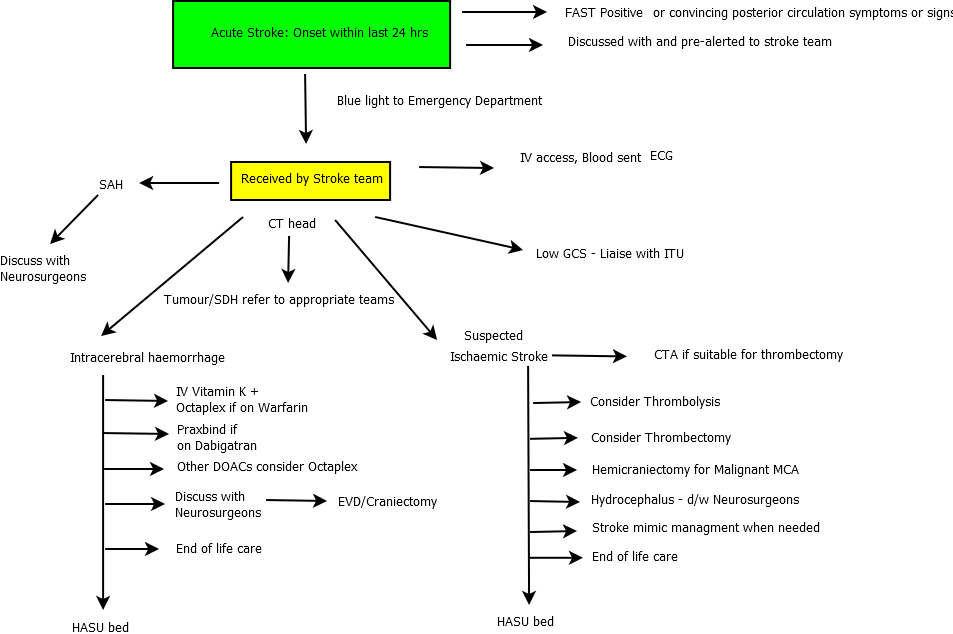
FAST positive → CT within 1 h → Thrombolysis if eligible (<4.5 h) → CTA for thrombectomy if LVO → Admit to HASU for monitoring & prevention.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
