| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
OSCE Examination of Visual Fields
Related Subjects: |OSCE Eye Exam |OSCE Ear Exam |OSCE Abdominal Exam |OSCE Ascites Exam |OSCE Jaundice Exam |OSCE Testicular Exam |OSCE Inguinal Exam |OSCE Upper limb Neurology |OSCE Lower limb Neurology |OSCE Face Neurology |OSCE Visual Fields
👋 Introduction
- 🧼 Hand Hygiene: Wash your hands thoroughly before starting.
- 🙂 Patient Introduction: Introduce yourself, confirm name and DOB, and explain the procedure.
- 📝 Consent & Explanation: Gain consent and explain you will test their side vision (peripheral vision).
🧰 Equipment Needed
- 📏 Snellen chart (mainly for central vision, if needed).
- ✏️ A pen, finger, or small target for confrontation testing.
- 💡 A well-lit room with plain background.
- 🎯 A fixation target (usually the examiner’s nose).
⚠️ Common OSCE errors:
– Not testing each eye separately (always occlude one eye 👁️).
– Homonymous hemianopia 👉 usually stroke affecting opposite hemisphere.
– Bitemporal hemianopia 👉 usually pituitary macroadenoma compressing the chiasm.
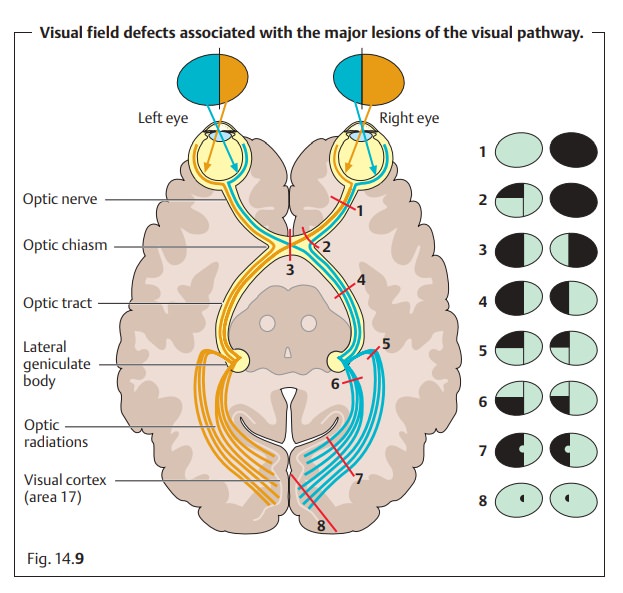
👀 Visual Field Defects
-
👓 Bitemporal Hemianopia
- Description: Loss of outer (temporal) fields in both eyes.
- Common Cause: Pituitary adenoma compressing the optic chiasm.
-
↔️ Homonymous Hemianopia
- Description: Loss of the same half of the visual field in both eyes.
- Common Causes: Stroke, tumour, or lesion in optic tract, optic radiations, or occipital cortex.
-
⬆️ Homonymous Superior Quadrantanopia
- Description: “Pie in the sky” – loss of the upper quadrant of the visual field.
- Common Cause: Temporal lobe lesion (Meyer’s loop involvement).
-
⬇️ Homonymous Inferior Quadrantanopia
- Description: “Pie on the floor” – loss of the lower quadrant of the visual field.
- Common Cause: Parietal lobe lesion.
-
🎯 Central Scotoma
- Description: Loss of central vision, blind spot in the middle of vision.
- Common Causes: Optic neuritis (MS), Leber’s optic neuropathy.
🪜 Step-by-Step Examination
- 👥 Preparation & Positioning:
- Sit patient at eye level in good light.
- Ask them to fixate on your nose (do not look at your fingers).
- Explain: “Tell me as soon as you see my finger coming into view.”
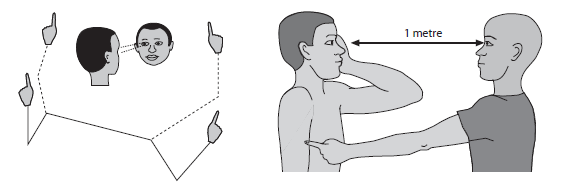
- 👁️ Testing Each Eye (Confrontation):
- Ask patient to cover one eye with hand/occluder.
- You close your opposite eye (to mirror them).
- Bring a finger/pen from periphery → centre in 4 quadrants.
- Ask patient to say “now” when they first see it.
- Note any areas missed → possible visual field defect.
- 🔄 Repeat on the Other Eye:
- Switch occlusion and repeat exactly.
- Compare fields between both eyes.
- 🧐 Additional Observations:
- Check response consistency and reaction time.
- If available, confirm with automated perimetry for precision.
🗒️ Documentation & Communication
- Record method used (confrontation test) and findings (e.g., “Right superior quadrantanopia”).
- Explain results sensitively to the patient.
- Recommend formal perimetry if defect detected.
⭐ Key OSCE Points
- Systematic: Preparation → Test Each Eye → Compare → Document.
- Clear communication keeps patient comfortable.
- Check fixation carefully → ensures accuracy.
- Always compare both eyes → asymmetry is key.
🚫 Common Pitfalls
- Not explaining → confused patient, poor cooperation.
- Poor fixation → unreliable results.
- Skipping quadrants → missed defects.
- Not comparing both eyes.
📚 References & Further Reading
- Geeky Medics: Visual Field OSCE Guide
- Clinical Methods – Walker et al.
- OSCEstop – Practice stations and notes.
