| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Constipation (Adults) ✅
💡 Constipation is common, usually benign, but always rule out bowel obstruction first 🚨 (Look for distension, vomiting, absent bowel sounds, hernial orifices, AXR findings). ⚠️ Avoid stimulant laxatives until obstruction excluded.
🌿 Introduction
- Rome IV criteria exist for academic diagnosis [Rome IV link], but most clinical practice is pragmatic.
- Diet: encourage hydration 🥛, mobility 🚶, and fibre (aim 30 g/day). Sorbitol-rich fruits (apples, pears, plums, grapes, raspberries, prunes) are especially helpful.
- Normal variation: stool frequency ranges from twice daily to twice weekly.
🧠 Anatomy & Physiology of Defaecation
- Colon: absorbs water, compacts stool.
- Rectum: storage; stretch receptors trigger defaecation reflex.
- Anus:
- Internal sphincter: involuntary (smooth muscle)
- External sphincter: voluntary (skeletal muscle)
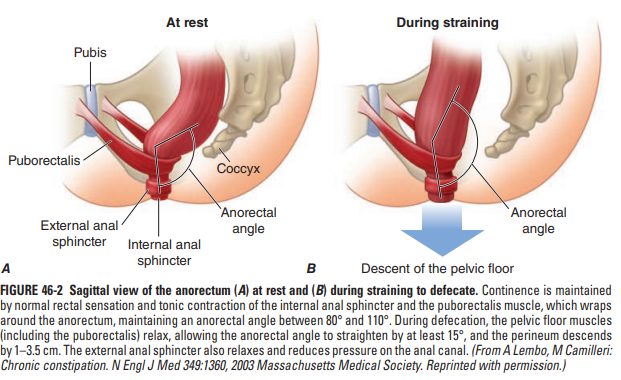
- Puborectalis muscle: maintains anorectal angle for continence; relaxes during defaecation 💩.
🧾 Common Associations
- Childhood: Hirschsprung’s, cystic fibrosis
- Endocrine/metabolic: hypothyroidism, diabetes, hypercalcaemia, pregnancy
- Neurological: Parkinson’s, MS, spinal cord disease
- Structural: colon cancer, diverticulitis, haemorrhoids
- Medications 💊: opiates, antidepressants, diuretics, CCBs, iron, anticholinergics, NSAIDs, aluminium antacids
- Acute illness: immobility, dehydration
🚩 Red Flags (Investigate)
- PR bleeding, weight loss, family history of colorectal cancer
- Tenesmus, anorexia, night sweats, fever, ↑ inflammatory markers
- Abdominal mass, distension, or pain on PR exam
💊 Laxative Classes
- Bulk-forming: Ispaghula husk (Fybogel) – first-line, needs hydration; avoid in obstruction
- Osmotic: Macrogol (Movicol), Lactulose – for hard stools or opioid-induced constipation; may cause bloating/flatulence
- Stimulant: Senna, Bisacodyl, Sodium Picosulfate – poor propulsion; hydrolysed in colon; avoid if obstruction
- Stool softener: Docusate – adjunct, mild stimulant effect; useful in opioid constipation
- Prokinetic: Prucalopride – severe chronic constipation; 5HT4 agonist; caution in ischaemic heart disease
- Rectal: Phosphate/Microlax/Arachis oil enemas – disimpaction, rapid relief; avoid arachis oil in peanut allergy
🏥 In-Hospital Pearls
- Common triggers: immobility, dehydration, opiates/codeine
- Always examine rectum for hard stool
- Stop causative drugs if possible
- Escalation for disimpaction: Microlax → Phosphate → Arachis oil → Manual removal
💡 Toileting & Lifestyle Advice
- Encourage unhurried, regular routine ⏰
- Respond promptly to urge
- Support mobility and privacy
- Ensure supported seating for frail patients
⚠️ Laxative Cautions
- Avoid in suspected obstruction, perforation, paralytic ileus, toxic megacolon, active IBD flare
- Specific cautions:
- Lactulose: galactosaemia
- Bisacodyl: severe dehydration
- Arachis oil enemas: peanut allergy
- Prolonged overuse → electrolyte imbalance (esp. hypokalaemia)
Cases - Constipation in Adults 🚽
- Case 1 - Functional Constipation 🥖: 45-year-old man, hard stools every 4–5 days, bloating, no red flags. Diet low in fibre. Management: Lifestyle modification (increase fibre, fluids, exercise); bulk-forming laxatives if required.
- Case 2 - Opioid-Induced Constipation 💊: 62-year-old woman on morphine, painful hard stools. Management: Regular stimulant + osmotic laxatives; consider peripherally acting opioid antagonist (e.g., naloxegol) if refractory.
- Case 3 - IBS-C 🌿: 35-year-old woman, alternating constipation and bloating, colonoscopy normal. Management: Dietary advice (low FODMAP), osmotic laxatives (PEG), linaclotide if refractory.
- Case 4 - Secondary Constipation (Hypothyroidism) 🦋: 70-year-old man, lethargy, weight gain, constipation. TFTs: TSH ↑, T4 ↓. Management: Thyroxine replacement; short-term laxatives if symptomatic.
Teaching Commentary 🧠
Constipation in adults is usually functional, but always consider: - Primary/functional (diet, IBS, slow transit) - Secondary (drugs, endocrine, metabolic, neurological) - Obstructive (colorectal cancer, strictures) ⚠️ Red flags: weight loss, anaemia, rectal bleeding, new onset >50 yrs → urgent colonoscopy Stepwise management: lifestyle → bulk-forming → osmotic → stimulant → specialist referral if refractory.

Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
