| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Placenta praevia
Related Subjects: |Antepartum haemorrhage |Postpartum haemorrhage |Acute Haemorrhage |Placenta praevia |Placenta abruption |Anti-D immunoglobulin
⚠️ About
- Placenta praevia = placenta implanted in lower uterine segment, covering/reaching internal cervical os.
- Major cause of painless antepartum haemorrhage in 2nd–3rd trimester → usually requires Caesarean delivery.
- 🚨 Avoid digital vaginal examination if suspected → can trigger catastrophic bleeding.
📊 Aetiology
- Incidence ~1 in 200 pregnancies.
- Bleeding can be severe/rapid due to uterine blood flow (600–800 mL/min at term).
- USS in early pregnancy may show “low-lying placenta” → usually migrates upward with uterine growth, but persistent low position = praevia.
⚠️ Risk Factors
- Previous Caesarean section (scar tissue, abnormal placental implantation)
- Multiparity & multiple pregnancy → larger placental surface area
- Uterine abnormalities (fibroids, prior uterine surgery)
- Smoking, advanced maternal age
🩺 Clinical Features
- Painless vaginal bleeding (classically at 29–30 wks or later).
- Uterus soft, non-tender (contrast with abruption).
- Fetal heart rate usually normal (unless severe haemorrhage).
- Speculum exam may show blood, but digital VE contraindicated.
- Often abnormal lie/presentation (e.g. transverse/oblique) due to placental obstruction of lower segment.
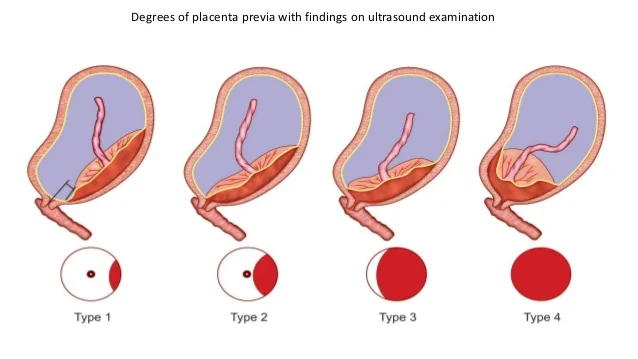
📑 Grades of Placenta Praevia
- Complete: placenta fully covers os
- Partial: placenta partially covers os
- Marginal: placenta reaches os edge but does not cover
- Low-lying: in lower segment but does not reach os
🔍 Differential Diagnosis
- Placental abruption: painful, tender uterus, often concealed bleeding
- Local genital causes: cervical polyp, infection, trauma
🧪 Investigations
- Transvaginal USS: gold standard (safer & more accurate than transabdominal).
- Bloods: FBC, group & cross-match, clotting screen, U&E.
- CTG: fetal monitoring.
🏥 Management
- Stabilise mother first: IV access, fluids, cross-match, transfuse as needed (Hb >10 g/dL).
- Hospital admission: if recurrent bleeding or major praevia; sometimes recommended from 35 weeks.
- Steroids: if <34 wks → promote fetal lung maturity.
- Definitive delivery: planned Caesarean section at 37–38 wks, earlier if bleeding or distress. Consultant-led care essential.
⚠️ Complications
- Maternal haemorrhage & shock
- Preterm labour or iatrogenic preterm delivery
- Placenta accreta spectrum (invasion into myometrium) → risk of massive PPH
- Malpresentation (breech, transverse)
📌 Exam Pearls
- Placenta praevia = painless bleeding, soft uterus, normal FHR
- Placental abruption = painful, tense uterus, fetal distress
- Always confirm with USS before VE
- Low-lying placenta at 20 wks often resolves; persistence into 3rd trimester = praevia
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
