| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Uveitis ✅
Related Subjects: |Episcleritis |Scleritis |Assessing a Red eye |Acute Angle Closure Glaucoma |Allergic and Infective Conjunctivitis |Anterior and Posterior Uveitis |Atropine Sulfate |Herpes simplex keratitis (HSK) |Acute Blepharitis |Chalazion
“Uveitis” comes from the Latin word uva, meaning grape.
If there is recent intraocular surgery (e.g. cataract or intravitreal injections), always consider endophthalmitis as the cause of pain and photophobia — arrange **same-day** ophthalmology referral.
About
- Inflammation of the uveal tract: iris, ciliary body, and choroid.
- Causes include trauma, iatrogenic sources, infection, drugs, systemic autoimmune disease, or idiopathic.
- Anterior uveitis often affects young adults and can cause long-term, sight-threatening complications.
Epidemiology
- ~50% of cases are idiopathic.
- Can occur at any age, but peak ~40 years.
- Anterior uveitis = ~90% of cases.
Types
- Anterior uveitis: Iritis, cyclitis, or iridocyclitis.
- Posterior uveitis: Choroiditis, retinitis, chorioretinitis, or retinal vasculitis.
- Intermediate uveitis: Involves vitreous and peripheral retina.
- Panuveitis: Inflammation of the entire uveal tract.
Aetiology (50% idiopathic)
- Idiopathic anterior uveitis (often HLA-B27 positive).
- Trauma or ophthalmic surgery.
- Ocular syndromes: Fuchs’ heterochromic cyclitis, Posner–Schlossman syndrome.
- Rheumatology: Ankylosing spondylitis, Psoriatic arthritis, Reactive arthritis, JIA, Behçet’s, PAN, GPA (Wegener’s).
- Infective: HSV, VZV, CMV, TB, syphilis, toxoplasmosis, brucellosis, Lyme, leptospirosis.
- Systemic: Sarcoidosis, MS, Crohn’s, ulcerative colitis, Whipple’s disease.
- Rare: Primary CNS lymphoma.
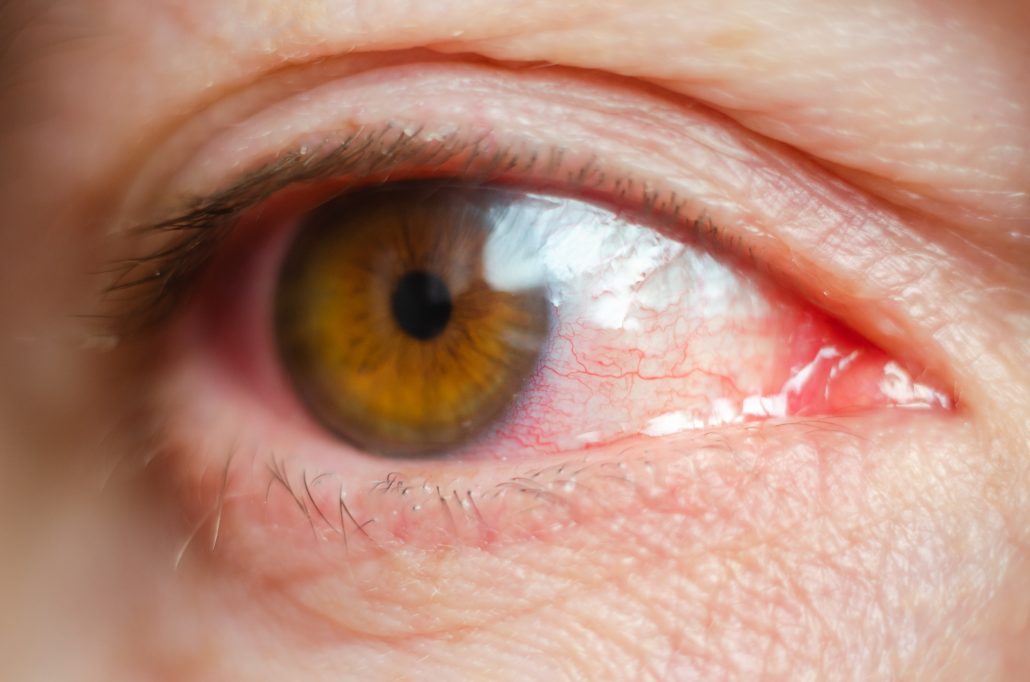
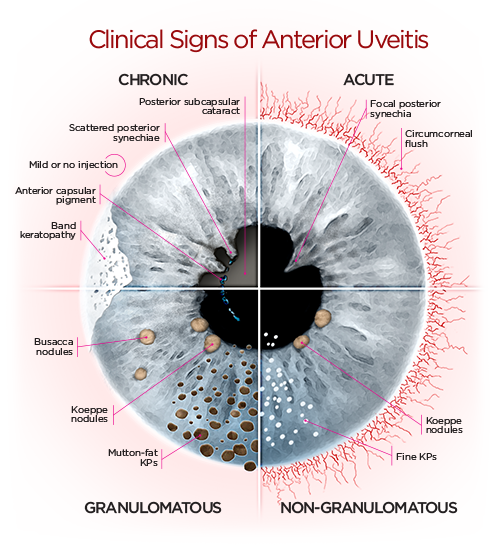
Clinical Features
- Severe ocular pain, tearing, and photophobia.
- Small pupil (miosis) due to iris spasm.
- Diffuse redness, often worse at limbus (ciliary flush).
- Cloudy anterior chamber from WBCs/protein (“cells and flare”).
- Visual acuity may be reduced; look for hypopyon.
- Posterior synechiae, keratic precipitates, corneal infiltrates may be seen.
- Always check IOP and corneal staining (exclude keratitis/trauma).
Investigations
- Slit lamp: anterior chamber cells, flare, keratic precipitates (fine = nongranulomatous; “mutton-fat” = granulomatous).
- PCR useful in herpetic uveitis/acute retinal necrosis.
- Systemic work-up: FBC, ESR/CRP, ANA, HLA-B27, syphilis serology, TB screen, chest X-ray (sarcoid/TB).
- Ocular imaging (OCT, B-scan) for posterior disease.
Differentials
- Endophthalmitis (post-surgery/injection).
- Keratitis (bacterial, viral, chemical burn).
- Acute angle-closure glaucoma.
- Intraocular foreign body.
Complications
- Glaucoma (raised IOP).
- Cataracts (from disease or steroid treatment).
- Corneal scarring or band keratopathy.
- Cystoid macular oedema.
- Steroid-related systemic side effects.
Management (Ophthalmology referral essential)
- Urgent / same-day ophthalmology referral if suspected endophthalmitis, severe pain, vision loss, hypopyon or corneal involvement (NICE CKS recommendation).
- Management is led by ophthalmologist; do not initiate treatment in primary care unless specifically advised.
- Idiopathic anterior uveitis (once assessed by ophthalmologist):
- Topical corticosteroids (prednisolone acetate) tapered over 4–6 weeks.
- Cycloplegics (homatropine 5%, scopolamine 0.25%, or atropine) → relieve spasm & prevent synechiae.
- Mydriatics (phenylephrine) sometimes used in-office to break synechiae.
- Sun protection: sunglasses, brimmed hat, dimmed lighting during acute flare.
- Herpetic anterior uveitis: topical steroids + oral aciclovir 400 mg BD (long-term prophylaxis if recurrent).
- Severe or posterior uveitis: systemic steroids, immunosuppressants (methotrexate, azathioprine, biologics).
References
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
