| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Acute Liver Disease & Acute Liver Failure (NICE)
Related Subjects: |Chronic liver disease |Liver Function Tests |Ascites Assessment and Management |Budd-Chiari syndrome |Alcoholism and Alcoholic Liver Disease |Liver Transplantation
⚠️ Acute Liver Disease ≠ Acute Liver Failure
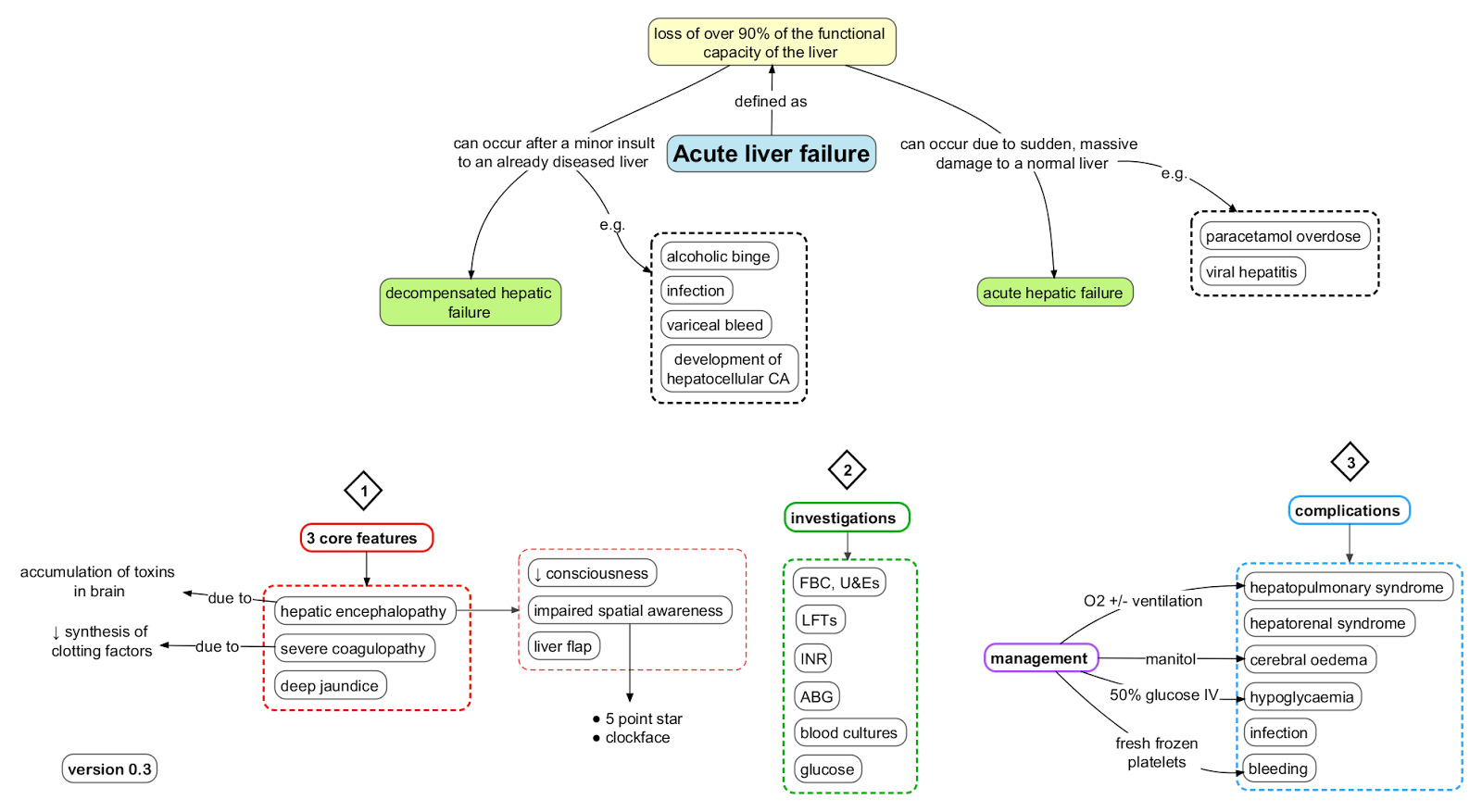
Acute liver disease can range from mild hepatocellular injury to life-threatening ALF. ALF is defined by impaired synthetic function (coagulopathy, encephalopathy) in a patient without pre-existing cirrhosis.
🩺 Acute Liver Disease & Acute Liver Failure – UK Guidelines
1. Classification of Acute Liver Failure
| Type | Jaundice → Encephalopathy | Common Causes | Key Features |
|---|---|---|---|
| Hyperacute | < 1 week | 💊 Paracetamol, viral hepatitis A/B/E | High risk of cerebral oedema, rapid deterioration |
| Acute | 1 week – 1 month | Drugs, viruses, autoimmune | Cerebral oedema possible, variable prognosis |
| Subacute | 1 – 3 months | Drugs, viruses, idiopathic | Lower cerebral oedema risk, slower progression |
2. Causes of Acute Liver Disease & ALF
- 🦠 Infectious: HAV–E, HBV, HCV, HDV, EBV, CMV, HSV, VZV, adenovirus, dengue, SARS-CoV-2
- 💊 Drugs/Toxins: Paracetamol (dose-dependent), antibiotics, anticonvulsants, NSAIDs, statins, herbal remedies; Amanita mushroom 🍄, carbon tetrachloride
- 🍷 Alcoholic hepatitis
- 🛡️ Autoimmune hepatitis
- 🧬 Metabolic: NAFLD, Wilson’s disease, haemochromatosis, alpha-1 antitrypsin deficiency
- ⚠️ Pregnancy-related: HELLP, acute fatty liver of pregnancy, preeclampsia
- 🩸 Vascular/Ischaemic: Budd–Chiari, cardiogenic shock, heatstroke, sinusoidal obstruction
- 🐀 Others: Leptospirosis, yellow fever, Reye’s syndrome, graft non-function post-transplant
3. Clinical Features: Jaundice Encephalopathy Coagulopathy
- 📖 History: Recent drug/toxin exposure, travel, infection
- 🤢 Symptoms: Jaundice, nausea, vomiting, bleeding, hypoglycaemia
- 🧠 Encephalopathy: Asterixis, confusion, fetor hepaticus, coma (Grades 1–4)
- RUQ pain, hepatomegaly, pale stools, dark urine
- Stigmata of chronic liver disease usually absent
🩺 Clinical Signs: Acute vs Chronic Liver Failure
| Feature | Acute Liver Failure ⚡ | Chronic Liver Disease 🕰️ |
|---|---|---|
| Onset ⏱️ | Rapid (days–weeks) | Insidious (months–years) |
| Encephalopathy 🧠 | Early, progresses quickly: confusion → coma (Grades 1–4) | Late; usually precipitated by infection, GI bleed, or medications |
| Jaundice 🟡 | Sudden, often marked, dark urine 💛 | Gradual, persistent, mild initially |
| Coagulopathy 🩸 | Severe, INR ↑ early; bleeding risk high | Variable; chronic compensated coagulopathy possible |
| Ascites 💧 | Rare at presentation, may develop later | Common, recurrent |
| Splenomegaly 🌳 | Usually absent | Common, due to portal hypertension |
| Spider Naevi / Palmar Erythema 🕷️ | Rare | Common, classic stigmata |
| Caput Medusae / Varices 🐍 | Rare | Common, may cause GI bleeding 🍽️ |
| Muscle Wasting 💪 | Usually absent | Common, due to chronic malnutrition and catabolism |
| Other Stigmata ⚕️ | Minimal; mainly jaundice-related features | Gynecomastia 👨🦰, testicular atrophy, nail changes 💅, palmar erythema ✋, asterixis ✋, bruising 🟣 |
💡 Clinical Tip: Acute liver failure ⚡ presents dramatically with early coagulopathy 🩸 and encephalopathy 🧠, often before stigmata of chronic disease develop. Chronic liver disease 🕰️ evolves slowly, with portal hypertension signs 🌳💧 and systemic manifestations 💪.
4. Investigations – Hepatocellular Injury vs Synthetic Function
| Parameter | Findings / Interpretation | Clinical Tip |
|---|---|---|
| AST / ALT | >1000 → paracetamol, viral, ischaemic hepatitis
100–500 → alcohol, NAFLD, chronic hepatitis |
High alone ≠ failure; check synthetic markers |
| ALP / GGT | Raised in cholestasis, drug-induced injury, obstruction, malignancy | Compare with bilirubin to assess cholestatic pattern |
| INR / Albumin | Prolonged INR or low albumin = impaired synthetic function → ALF risk | Essential for distinguishing simple injury from ALF |
| Other Labs | FBC, U&E, viral serology, autoimmune screen, copper/iron studies, pregnancy test, HIV | Tailor to history and suspected aetiology |
| Imaging | Ultrasound ± Doppler: obstruction, Budd–Chiari, steatosis, hepatomegaly | Rapid bedside imaging for vascular or obstructive causes |
5. Management
- 🛌 Admit to HDU/ICU; early hepatology involvement
- 🔄 ABC support: airway, oxygen, fluids
- 🍬 Hypoglycaemia: IV dextrose
- 🩸 Coagulopathy: Vitamin K ± FFP / platelets if bleeding or prior to invasive procedures
- 💩 Encephalopathy: Lactulose, maintain 2–3 soft stools/day
- 🧠 ICP precautions: head up 20°, avoid hypotension/hypoxia, mannitol if cerebral oedema
- 🚑 Early transplant referral for ALF with encephalopathy + coagulopathy (King’s College criteria)
6. Cause-Specific Therapy
- 💊 Paracetamol overdose → IV N-acetylcysteine (NAC)
- 🛡️ Autoimmune hepatitis → corticosteroids (infection excluded)
- 🍄 Amanita mushroom → IV Penicillin G ± silymarin; urgent transplant evaluation
- 🤰 Pregnancy-related → prompt delivery if HELLP or acute fatty liver
- 🧬 Wilson’s disease → chelation or urgent transplant
- 🦠 Viral hepatitis → supportive ± antivirals (HSV/HBV)
- 🩸 Budd–Chiari → anticoagulation, thrombolysis, shunt, or transplant
7. Complications
- ⚡ Hypoglycaemia
- 🩸 Coagulopathy & bleeding
- 🧠 Cerebral oedema → herniation risk
- 🧬 Infection / sepsis
- ⛑️ Hepatorenal syndrome
8. References
- NICE NG148 – Hepatitis B & C
- BNF – Drug management
- UKHSA – Viral hepatitis & acute liver disease alerts
- NCBI – Acute Liver Disease
- EASL Clinical Practice Guidelines (2017)
💡 Clinical Pearl: Always assess synthetic function (INR, albumin) to distinguish hepatocellular injury from life-threatening ALF. AST/ALT >1000? Consider paracetamol, viral hepatitis, or ischaemic causes. Early recognition + supportive care saves lives.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
