| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Cerebral Vasculitis
⚠️ Cerebral vasculitis is frequently overdiagnosed due to over-interpretation of angiographic “beading”. Catheter angiography is neither sensitive nor specific. Immunosuppressive treatments are toxic - establish diagnosis carefully before treatment.
🩺 Introduction
- Inflammation of cerebral blood vessels leading to stenosis, occlusion, thrombosis, or haemorrhage.
- May be primary (PACNS) or secondary to systemic vasculitis, infection, malignancy, or autoimmune disease.
- No single clinical, blood, or imaging test is diagnostic.
- Diagnosis is clinicoradiological and often requires biopsy.
🧬 Aetiology
- Immune-mediated endothelial injury.
- Immune complex deposition in vessel walls.
- ANCA-associated mechanisms.
- Genetic and environmental triggers.
- Secondary causes: infection (TB, HIV, syphilis), malignancy, drugs, connective tissue disease.
📊 Size-Based Classification (Systemic Context)
| Vessel Size | Examples |
|---|---|
| Large Vessel | Giant Cell Arteritis, Takayasu arteritis |
| Medium Vessel | Polyarteritis nodosa, Kawasaki disease |
| Small Vessel |
|
🧠 Primary Angiitis of the CNS (PACNS)
- Inflammatory vasculitis confined to CNS.
- Any age; typically subacute headache, cognitive decline, focal deficits.
- CSF abnormal in ~80% (raised protein, lymphocytosis).
- Angiography may show segmental narrowing (“beading”) but not diagnostic.
- Brain/leptomeningeal biopsy is gold standard (may be false negative in segmental disease).
🔎 Clinical Features
- Headache (commonest symptom).
- Ischaemic stroke (single or multiple territories).
- Intracerebral haemorrhage.
- Seizures.
- Encephalopathy.
- Systemic features if secondary vasculitis (rash, renal impairment, arthritis).
🔬 Investigations
- Bloods: ESR, CRP, FBC, U&E, LFTs.
- Autoimmune screen: ANA, dsDNA, ANCA (PR3/MPO), complement, RF.
- Infection screen: HIV, Hep B/C, syphilis, TB.
- Urinalysis for glomerulonephritis.
- CSF: Raised protein ± lymphocytes (PACNS often inflammatory).
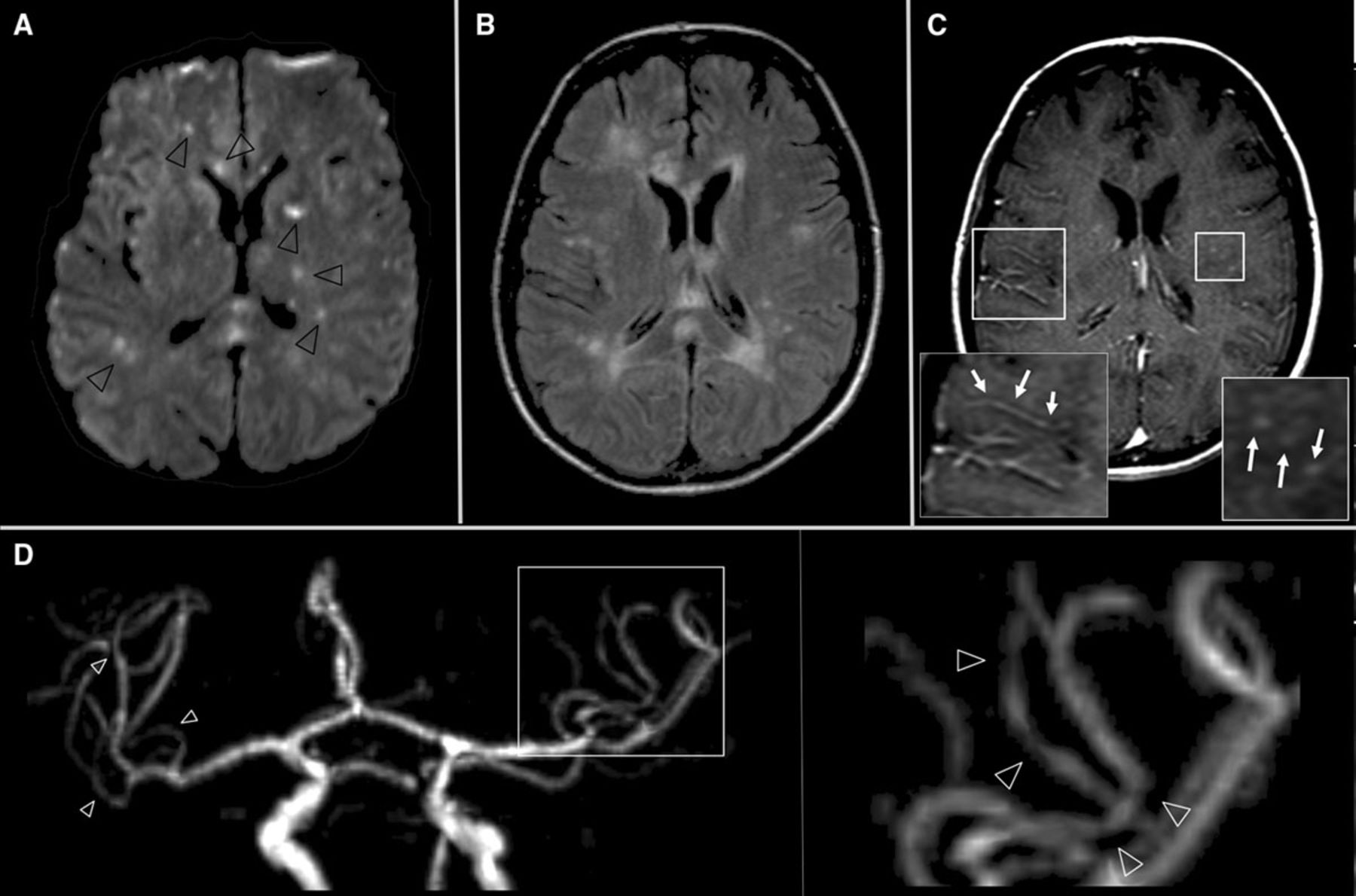
- MRI brain: Multifocal infarcts of different ages; haemorrhage; vessel wall enhancement on high-resolution imaging.
- DSA: May show segmental stenosis and dilatation (“string-of-beads”).
- FDG-PET: Helpful in large vessel systemic vasculitis.
- Biopsy: Definitive diagnosis if positive.
⚖️ Differential Diagnosis of Angiographic “Beading”
- Reversible Cerebral Vasoconstriction Syndrome (RCVS).
- Fibromuscular dysplasia.
- Vasospasm (post-SAH).
- Atherosclerosis.
- Infection-related vasculopathy.
- Embolic phenomena.
💊 Management Principles
- Confirm diagnosis before immunosuppression where possible.
- Exclude infection (critical before steroids).
- Induction therapy: High-dose corticosteroids ± cyclophosphamide.
- Alternative induction: Rituximab (especially ANCA-associated).
- Maintenance: Azathioprine, methotrexate, or mycophenolate mofetil.
- Monitor for drug toxicity (cytopenias, infection, bladder toxicity with cyclophosphamide).
🧠 Clinical Pearl
Not all angiographic beading is vasculitis. RCVS is far more common and does not require immunosuppression. Treating presumed vasculitis without adequate evidence can cause significant harm.
📚 Reference
- Berlit P. Diagnosis and treatment of cerebral vasculitis. Ther Adv Neurol Disord (2010).
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
