| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Anatomy and Physiology of the Bladder
Related Subjects: |Anatomy of the Glomerulus |Anatomy of the Bladder
🫙 The urinary bladder is a hollow, distensible muscular sac in the pelvis that temporarily stores urine (typically 400–600 mL comfortably, up to 800–1000 mL max) before voluntary voiding. It expands dramatically during filling (compliance ~20–40 mL/cm H₂O) and contracts forcefully during micturition to expel urine via the urethra.
🧬 Anatomy of the Bladder
- Location & Relations 📍
- Lies in the true pelvis, behind the pubic symphysis, anterior to the rectum (males) or uterus/vagina (females).
- Superior surface covered by peritoneum → forms anterior peritoneal reflection (vesicouterine/vesicorectal pouch).
- Males: prostate inferiorly, seminal vesicles posteriorly.
- Females: uterus/vagina posteriorly, pubic symphysis anteriorly.
- When full: rises above pubic symphysis → palpable/percussible in lower abdomen.
- External Features
- Apex (Fundus anterior): Superior/anterior point; attached to median umbilical ligament (urachus remnant).
- Base (Fundus posterior): Triangular posterior wall; ureters enter superolaterally.
- Body: Main expandable portion between apex and base.
- Neck: Inferior constriction; continuous with prostatic urethra (males) or urethra (females).
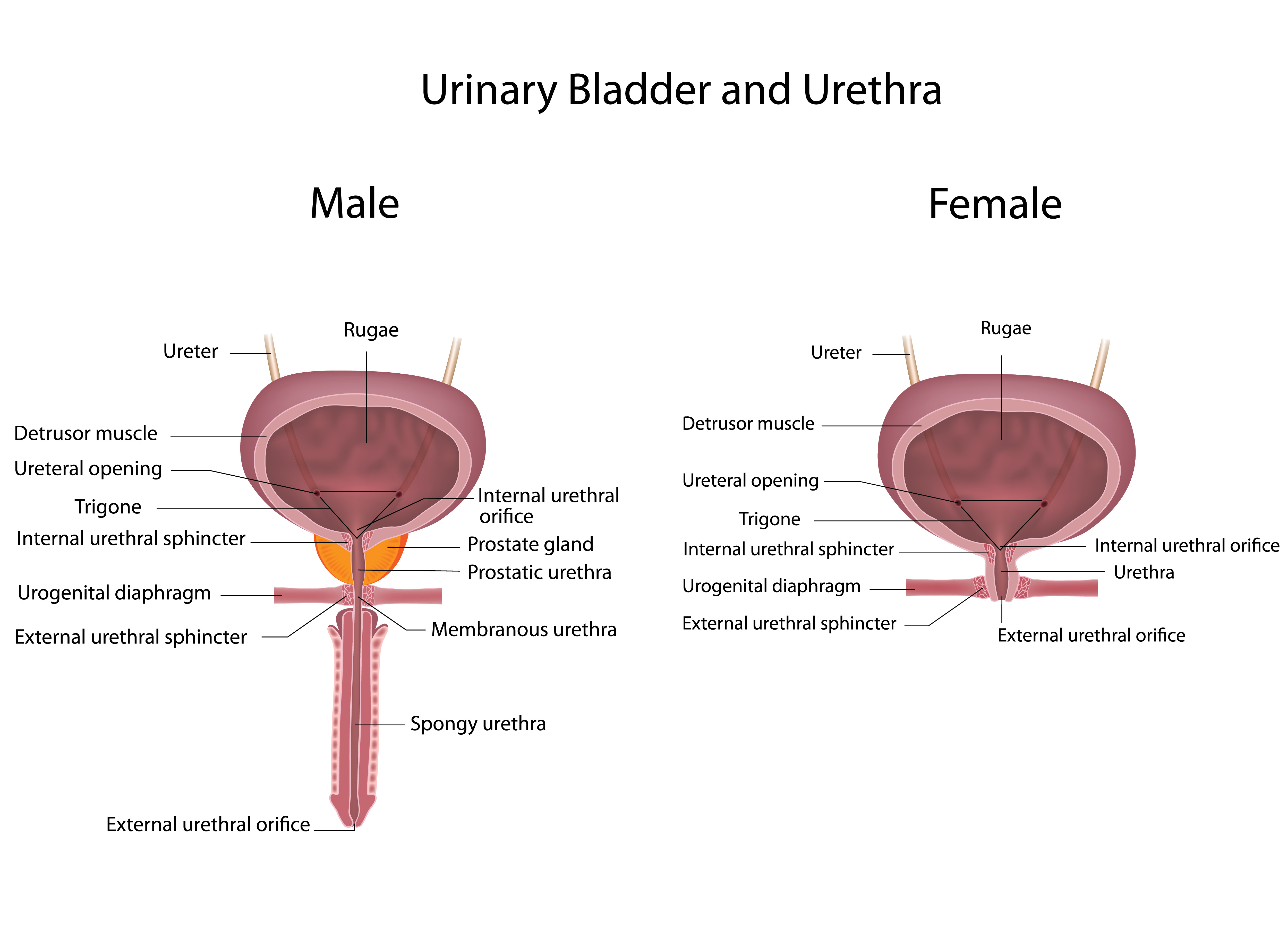
- Internal Features – Trigone 🔺
- Smooth, fixed triangular area on posterior base.
- Boundaries: two ureteric orifices (superolateral) + internal urethral orifice (inferior apex).
- Lined by tightly adherent mucosa (no rugae) → less distensible; embryologically mesodermal (vs endodermal body).
- Interureteric ridge (between ureteric orifices) clinically visible on cystoscopy.
- Histological Layers 🧪
- Mucosa: Transitional (urothelium) epithelium (6–8 layers when empty → 2–3 when stretched) + lamina propria (connective tissue with blood vessels, nerves, lymphoid follicles).
- Submucosa (lamina propria continuation): loose connective tissue; allows folding (rugae) when empty.
- Muscularis (Detrusor muscle): Thick smooth muscle in 3 poorly defined layers (inner/outer longitudinal, middle circular) → powerful contraction during voiding.
- Adventitia/Serosa: Outer connective tissue; superior surface covered by visceral peritoneum (serosa).
🩸 Vascular Supply
- Arterial ❤️
- Superior vesical arteries (from internal iliac) → anterosuperior bladder.
- Inferior vesical arteries (males) / vaginal artery (females) → posteroinferior bladder.
- Additional: obturator, uterine, middle rectal arteries.
- Venous 💉
- Vesical venous plexus → internal iliac veins (main drainage).
- Connections to prostatic/uterine/vaginal plexuses → risk of spread in malignancy.
- Lymphatic: Follow arteries → internal iliac → common iliac → para-aortic nodes.
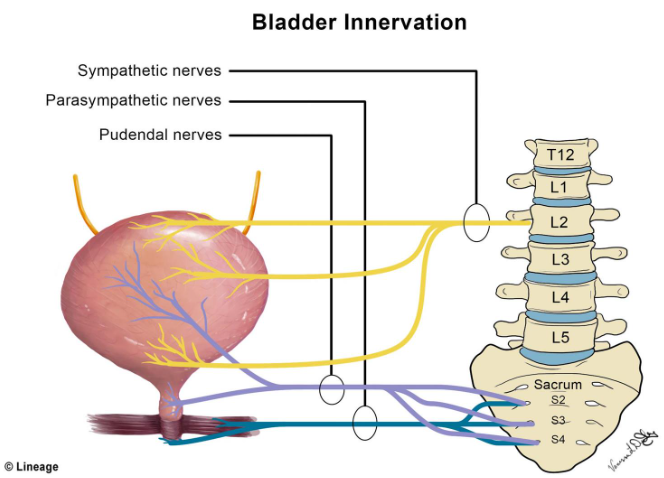
🧠 Neural Supply & Micturition Reflex
| Division | Origin | Target | Effect | Neurotransmitter |
|---|---|---|---|---|
| Sympathetic (storage) | Hypogastric plexus (T10–L2) | Detrusor muscle
Internal urethral sphincter | Relaxes detrusor
Contracts sphincter | Noradrenaline (β₂/β₃ receptors on detrusor, α₁ on sphincter) |
| Parasympathetic (voiding) | Pelvic splanchnic nerves (S2–S4) | Detrusor muscle
Internal urethral sphincter | Contracts detrusor
Relaxes sphincter | Acetylcholine (M₃ receptors) |
| Somatic (voluntary) | Pudendal nerve (S2–S4) | External urethral sphincter (striated muscle) | Voluntary contraction (continence) | Acetylcholine (nicotinic receptors) |
- Storage phase (sympathetic dominance): Low pressure filling (compliance), closed sphincters.
- Micturition reflex:
- Stretch receptors (Aδ/C fibres) in detrusor → pelvic nerves → sacral cord (S2–S4) → pontine micturition centre → cerebral cortex (voluntary control).
- Threshold ~200–400 mL → urge; voluntary relaxation of external sphincter + parasympathetic activation → detrusor contraction + sphincter relaxation.
- Neurogenic bladder: Suprapontine (uninhibited), spinal (detrusor-sphincter dyssynergia), infrasacral (atonic).
🫁 Physiology of the Bladder
- Filling/Storage phase:
- Ureters deliver urine intermittently → bladder fills slowly.
- Detrusor relaxes (sympathetic β₃), sphincters contracted → pressure remains low (<10–15 cm H₂O).
- Capacity: functional 400–600 mL; max ~800–1000 mL before strong urge.
- Voiding phase (micturition):
- Threshold stretch → afferent signals → reflex + voluntary inhibition release.
- Parasympathetic → detrusor contraction (intravesical pressure 40–100 cm H₂O).
- Sphincter relaxation → urine expulsion (~15–25 mL/s flow rate).
- Completion: detrusor relaxes, sphincters close.
🩺 Clinical Relevance
- Urinary incontinence 💦: Stress (pelvic floor weakness), urge (overactive bladder/detrusor instability), overflow (retention), functional (mobility/cognition).
- Urinary retention 🚫: Acute (BPH, drugs, post-op) vs chronic (neurogenic, obstruction) → risk of hydronephrosis, UTI, overflow incontinence.
- Cystitis / UTI 🔥: Bacterial (E. coli), interstitial (painful bladder syndrome), radiation/chemotherapy-induced.
- Bladder cancer 🧬: Transitional cell carcinoma (90%); risk factors: smoking, aromatic amines, schistosomiasis (squamous); painless haematuria most common presentation.
- Neurogenic bladder 🧠: MS, spinal cord injury, diabetic neuropathy → detrusor hyperreflexia/areflexia, dyssynergia → high-pressure retention, reflux nephropathy.
Teaching Point 🩺 Bladder = distensible storage organ (400–600 mL) with transitional epithelium + powerful detrusor. Storage: sympathetic (relax detrusor, contract sphincters). Voiding: parasympathetic (contract detrusor, relax internal sphincter) + voluntary external sphincter relaxation. Trigone = fixed, smooth area (ureteric + urethral orifices). Clinical keys: haematuria → cancer/UTI; retention → overflow incontinence; low compliance → high-pressure damage to kidneys.
📚 References (Feb 2026)
- Gray’s Anatomy 42nd ed. (2020; 2025 online updates).
- Wein AJ et al. Campbell-Walsh Urology (13th ed., 2025).
- EAU Guidelines: Neuro-urology & Incontinence (2025–2026).
- Recent: Bladder mechanosensation & TRP channels (Nature Rev Urol 2025).
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
