| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Goitre ✅
Related Subjects: |Neck Swellings by Triangle |Thyroglossal cyst |Head and Neck Cancers |Triangles of the neck |Cervical Lymphadenopathy |Goitre
🧑⚕️ Pemberton’s sign: Raising both arms above the head causes facial congestion, cyanosis, and respiratory distress due to obstruction of the thoracic inlet by a retrosternal goitre. A key bedside OSCE finding; positive in large substernal or mediastinal thyroid enlargement.
📖 About
- Goitre = enlarged thyroid gland (diffuse or nodular).
- WHO definition: thyroid lobes larger than the terminal phalanx of the patient’s thumb.
- Can be diffuse (uniform enlargement) or nodular (single or multinodular).
- May be euthyroid, hyperthyroid, or hypothyroid depending on aetiology.
⚡ Causes of Goitre
- Physiological: puberty, pregnancy
- Autoimmune: Hashimoto’s thyroiditis, Graves’ disease
- Iodine deficiency or excess
- Subacute thyroiditis (de Quervain)
- Medications / goitrogens: 💊 Lithium, Amiodarone; 🚬 smoking
- Idiopathic or familial
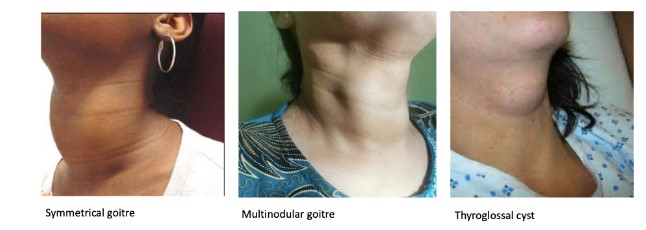
📑 Types
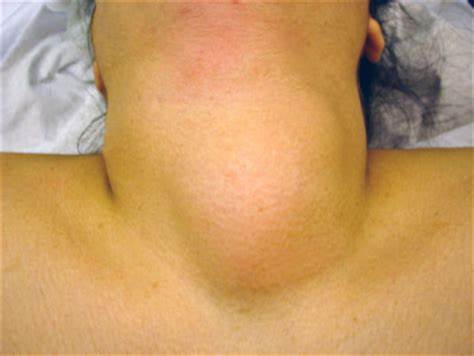
- Diffuse nontoxic goitre: Uniform enlargement, usually euthyroid; may compress trachea or oesophagus if large.
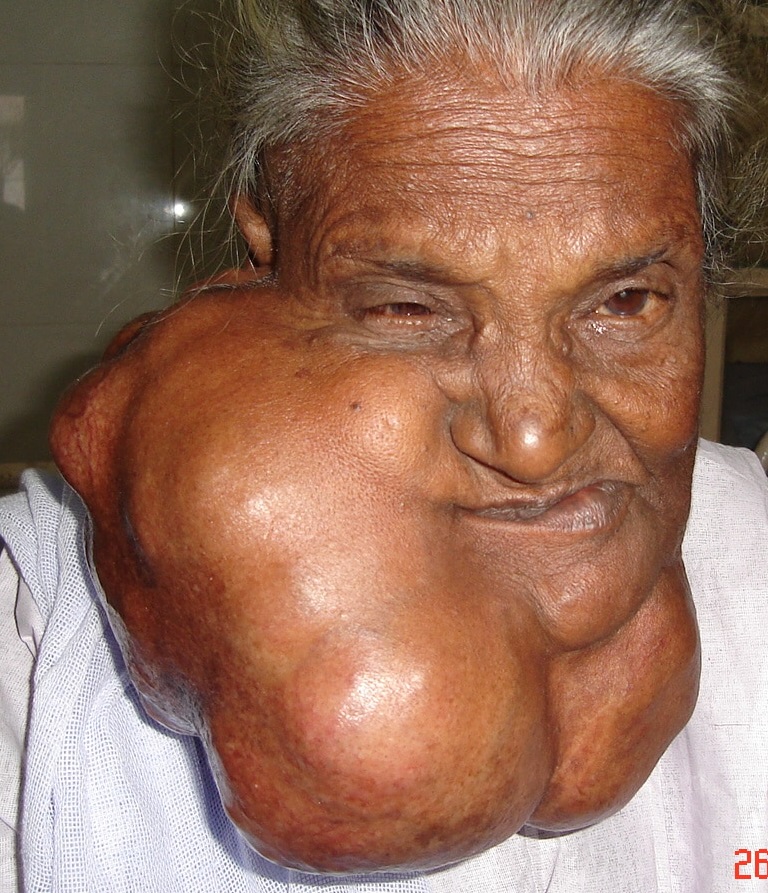
- Nodular / Multinodular goitre: Discrete nodules; may be toxic (autonomous) or non-toxic; compressive symptoms more common.
📏 WHO Grading of Goitre
- Grade 0: Not palpable or visible
- Grade 1: Palpable, not visible in neutral neck; includes small nodules
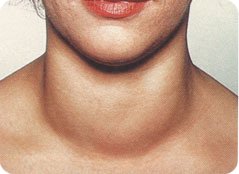
- Grade 2: Clearly visible swelling in neutral neck
🚩 Malignancy High-Risk Features
- Rapid growth or hard, fixed nodule
- Hoarseness (recurrent laryngeal nerve involvement)
- Cervical lymphadenopathy
- History of head/neck irradiation
- Thyroid cancer in first-degree relative
- MEN2 syndrome / elevated calcitonin
- FDG-PET avidity on incidental imaging
🩺 Clinical Examination
- Inspect from front & behind: neck contour, asymmetry, tracheal deviation.
- Palpate thyroid and cervical lymph nodes; assess nodularity, consistency, tenderness.
- Ask patient to swallow: thyroid moves upwards with swallowing.
- Listen for bruit (Graves’ disease).
- Check voice: hoarseness → recurrent laryngeal nerve compression.
- Assess for compressive symptoms: dyspnoea, dysphagia, stridor.
- Perform Pemberton’s manoeuvre if retrosternal extension suspected.
- Evaluate thyroid function signs: hypo- or hyperthyroid features.
🔬 Investigations
- Bloods: FBC, U&E, CRP (infection or inflammation)
- TFTs: TSH, free T4, T3. Hashimoto: ↑TSH; Graves: ↓TSH, ↑T3/T4
- Autoantibodies: Anti-TPO, Anti-Tg; TSH receptor antibodies for Graves’ disease
- Imaging:
- Ultrasound: first-line for morphology, nodule characterization, FNA guidance
- Radionuclide scan: if TSH suppressed (hot vs cold nodules)
- CT thoracic inlet / MRI: for retrosternal or mediastinal extension; use non-contrast to avoid iodine load if future RAI planned
🔍 FNA Indications (Nodules)
- Suspicious nodule + cervical lymphadenopathy
- High-risk history: ≥5 mm
- Microcalcification: >1 cm
- Solid nodule: >1 cm
- Mixed cystic-solid: >1.5–2 cm
- Spongiform: >2 cm
- Pure cystic: no FNA required
💊 Management (NICE-compliant)
- Rule out malignancy: USS ± FNA
- Observation: small, asymptomatic benign goitres; annual clinical review
- Iodine supplementation: if deficiency suspected (esp. endemic areas)
- Medical therapy:
- Thyroxine suppression rarely used; antithyroid drugs (Carbimazole, Propylthiouracil) for toxic goitre
- Radioactive iodine: indicated for toxic diffuse or multinodular goitre
- Surgery: for suspected malignancy, compressive symptoms, cosmetic concern, or failed medical therapy; total or hemithyroidectomy depending on disease
- Monitor airway and postoperative complications (haematoma, hypocalcaemia, RLN injury)
Cases - Goitre (Thyroid Enlargement)
- Case 1 - Multinodular Goitre with Compressive Symptoms 🦴: 68F, neck swelling, intermittent dysphagia, hoarseness. Irregular nodular thyroid, retrosternal extension, tracheal deviation on CXR. TFTs normal. Management: Surgical thyroidectomy, airway monitoring, histology to exclude malignancy.
- Case 2 - Diffuse Toxic Goitre (Graves’) 🔥: 32F, weight loss, heat intolerance, tremor, palpitations. Smooth diffuse goitre with bruit; exophthalmos, pretibial myxoedema. TFTs: TSH suppressed, T3/T4 elevated; TRAb positive. Management: Antithyroid drugs, β-blockers; consider RAI or surgery if relapse; ophthalmology review.
- Case 3 - Endemic Simple Goitre 🌍: 19F, large painless diffuse thyroid, no eye or compressive signs. Low dietary iodine; TFTs normal. Management: Iodine supplementation, dietary education; surgery if very large or disfiguring.
Teaching Commentary 🧠
Goitre assessment integrates function, structure, and compression. - Diffuse: Graves’ (hyperthyroid), Hashimoto’s (hypothyroid), simple/iodine deficiency (euthyroid). - Nodular: multinodular goitre, solitary nodule (benign vs malignant). Red flags: rapid growth, hard/irregular nodule, cervical lymphadenopathy, hoarseness → FNA ± surgery. NICE-compliant management: targeted investigation, risk stratification, stepwise intervention (observation → medical → RAI → surgery) with monitoring of airway and thyroid function.

Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
