| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
ECG - ST segment changes
Related Subjects: |ECG Basics |ECG Axis |ECG Analysis |ECG LAD |ECG RAD |ECG Low voltage |ECG Pathological Q waves |ECG ST/T wave changes |ECG LBBB |ECG RBBB |ECG short PR |ECG Heart Block |ECG Asystole and P wave asystole |ECG QRS complex |ECG ST segment |ECG: QT interval |ECG: LVH |ECG RVH |ECG: Bundle branch blocks |ECG Dominant R wave in V1 |ECG Acute Coronary Syndrome |ECG Crib sheets
📌 About
- The ST segment represents the period between ventricular depolarisation and repolarisation.
- It is normally isoelectric (flat) and shifts up or down when the myocardium is injured, inflamed, or stressed.
- Careful interpretation is vital as ST changes can indicate life-threatening cardiac pathology.

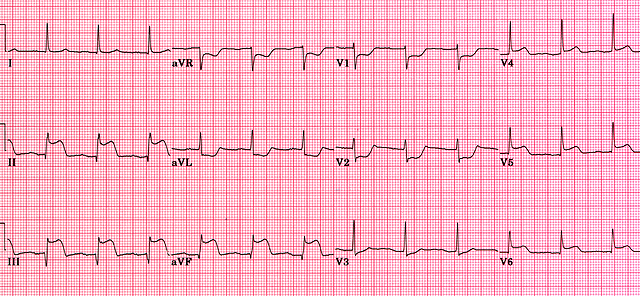
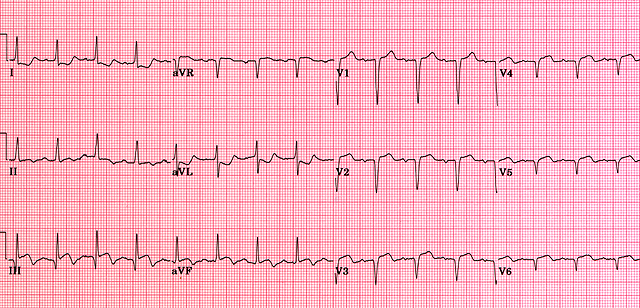
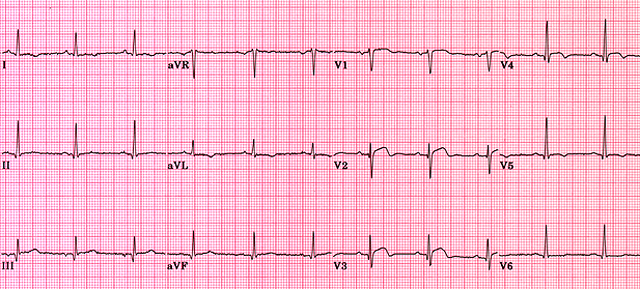
⬆️ ST Elevation
- Physiological “high take-off”: Fixed, benign elevation in V1–V3 (young healthy adults).
- Acute MI 🚑: ≥1 mm in 2 contiguous limb leads OR ≥2 mm in 2 chest leads. Often convex “tombstone” with reciprocal depression elsewhere.
- Pericarditis/Myocarditis ❤️🔥: Widespread, saddle-shaped, concave ST elevation (spares aVR, V1).
- LBBB: ST elevation can accompany abnormal conduction (use Sgarbossa criteria if MI suspected).
- LVH strain: ST elevation in right chest leads; usually with deep S waves and T inversion elsewhere.
- Brugada Syndrome ⚡: Coved ST elevation in V1–V3 (“shark fin” morphology); risk of sudden cardiac death.
- Coronary Spasm (Prinzmetal’s angina): Transient ST elevation resolving with nitrates.
- LV Aneurysm (post-MI scar): Persistent ST elevation without reciprocal changes.
⬇️ ST Depression
- Myocardial Ischaemia 🫀: Horizontal or down-sloping ST depression (≥1 mm) in V4–V6 = significant. Severity: Down-sloping > Flat > Up-sloping.
- LVH strain pattern: ST depression with asymmetrical T inversion in lateral leads.
- Digoxin effect 💊: “Reverse tick” scooped ST depression – classic exam favourite.
- Electrolyte disturbance: Hypokalaemia causes ST depression + U waves.
- Non-cardiac causes: Hyperventilation may mimic transient depression.
🚑 Immediate Action
- Suspected ACS: Treat as emergency if chest pain + ST changes.
- Give O₂ (if hypoxaemic), GTN spray, Aspirin 300 mg.
- Call 999 (UK) for rapid transfer to PCI centre if STEMI or ACS equivalent.
- Always compare with old ECGs to distinguish chronic vs acute changes.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
