| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Endoscopic Retrograde Cholangiopancreatography (ERCP)
Related Subjects: |Upper Gastrointestinal Bleed |Oesophageal Variceal Bleeding |Dieulafoy Lesion |Mallory-Weiss Tear |Gastric Cancer |Peptic Ulcer Disease |Hypovolaemic or Haemorrhagic Shock |Carcinoma of the Gallbladder |Carcinoma of the Bile Duct |Cholangiocarcinoma
🧾 Magnetic Resonance Cholangiopancreatography (MRCP) is now the preferred diagnostic tool for suspected biliary obstruction. ⚡ Endoscopic Retrograde Cholangiopancreatography (ERCP) is reserved mainly for therapeutic interventions such as stone extraction, sphincterotomy, and stent placement.
📖 About ERCP
- Combines upper GI endoscopy with fluoroscopic X-ray imaging.
- Used to visualise the bile ducts, pancreatic duct, and gallbladder.
- Crucially, ERCP is both diagnostic and therapeutic (unlike MRCP).
🩺 ERCP Procedure
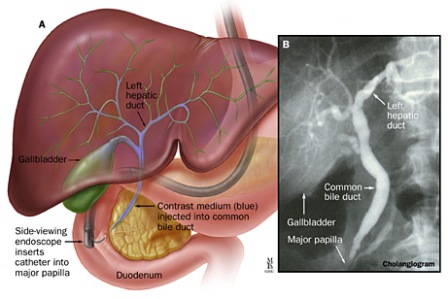
During ERCP, an endoscope is advanced to the duodenum. The bile duct is cannulated, and contrast dye is injected under X-ray guidance. ➡️ This provides detailed duct imaging and allows real-time interventions (stone removal, stent placement, biopsies).
📌 Indications for ERCP
- 🪨 Diagnosis and removal of common bile duct (CBD) stones.
- 🧬 Investigation and dilatation/stenting of biliary strictures (benign or malignant).
- 🧠 Diagnosis and palliation in cholangiocarcinoma or pancreatic cancer.
- ✂️ Sphincterotomy – cutting the sphincter of Oddi to aid stone clearance.
- 🩺 Pancreatic duct stenting in selected cases.
- 🔬 Biopsy or brush cytology of strictures or tumours.
🔎 Procedure Steps
- 🔒 Patient fasts and receives IV sedation ± analgesia.
- 📍 Endoscope passed via mouth → stomach → duodenum.
- 💉 Cannulation of bile/pancreatic duct, followed by contrast injection.
- 🧾 X-rays taken to identify stones, strictures, or tumours.
- ⚙️ Interventions performed as required (stone extraction, stenting, biopsy, sphincterotomy).
🪨 Example: Large CBD Stone
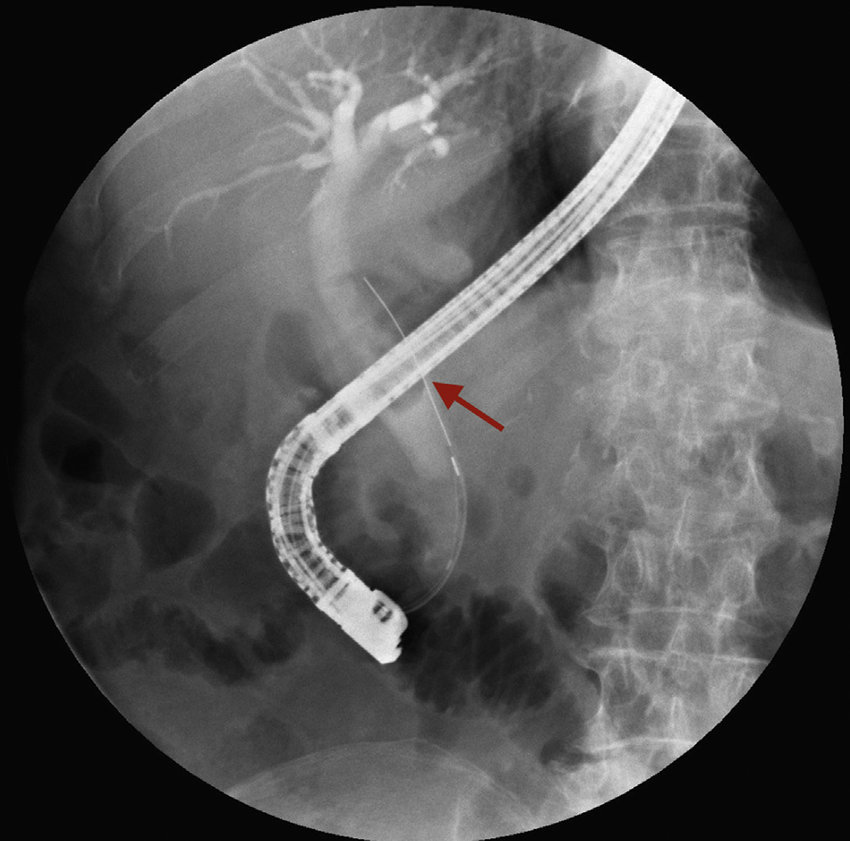
ERCP allows direct removal of obstructing CBD stones, restoring bile flow and preventing jaundice or cholangitis.
⏱️ Duration
- Typically lasts 60–120 minutes.
- Patients are sedated; recovery requires monitoring for a few hours post-procedure.
📝 Pre-Procedure Checklist
- ✅ Clotting screen (INR, platelets) if sphincterotomy likely.
- ✅ Review anticoagulants/antiplatelets → liaise with gastroenterology/haematology if on warfarin or DOACs.
- ✅ Consent discussion: include risk of pancreatitis, bleeding, infection, perforation.
⚠️ Potential Complications
- 💤 Sedation-related respiratory compromise.
- 🩸 Bleeding (~2% risk, especially post-sphincterotomy).
- ⚡ Acute pancreatitis (~5% risk; most common serious complication).
- 🦠 Cholangitis (biliary infection).
- 🕳️ Perforation of duodenum or ducts.
- ☢️ Cumulative radiation exposure (rarely significant).
📚 References
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
