| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
AIDS HIV Infection and a Fever ✅
Related Subjects: |AIDS (HIV) Neurological Disease |AIDS (HIV) Respiratory disease |AIDS Dementia Complex (HIV) |AIDS HIV Infection |AIDS(HIV) Gastrointestinal Disease |Acute Retroviral Syndrome (HIV) |HIV and Post-Exposure Prophylaxis (PEP) |HIV and Pre-exposure prophylaxis |HIV associated nephropathy (HIVAN) |HIV disease Assessment |Immune Reconstitution Syndrome |AIDS HAART Antiretrovirals |Kaposi sarcoma (KS)
| Algorithm - Approach to Fever in an HIV Patient (by CD4 Count) 🧪🌡️ |
|---|
|
Teaching Commentary 📘
Anchor your thinking in the CD4 count: - <200 → PCP, candidiasis - <100 → toxoplasmosis, cryptococcus - <50 → CMV, MAC. Remember “common things are common” — bacterial pneumonia, sepsis still predominate in the UK. Early ART reduces severe OIs, but knowledge of CD4 thresholds is essential for exams. 🌡️ Many patients with HIV may be asymptomatic. Always consider risk factors, recent exposures, and perform early testing.
📌 Introduction 🧬
- HIV prognosis has dramatically improved with HAART.
- Late diagnosis (low CD4) worsens outcomes.
- Current common causes of death: CAD, liver failure (HBV/HCV), lymphoma.
- HIV is now a chronic manageable disease with near-normal life expectancy if treated early.
🦠 Virus Overview
- HIV-1: Globally predominant, more virulent.
- HIV-2: Less virulent, mainly West Africa, resistant to NNRTIs.
🔬 Structure & Viral Cycle
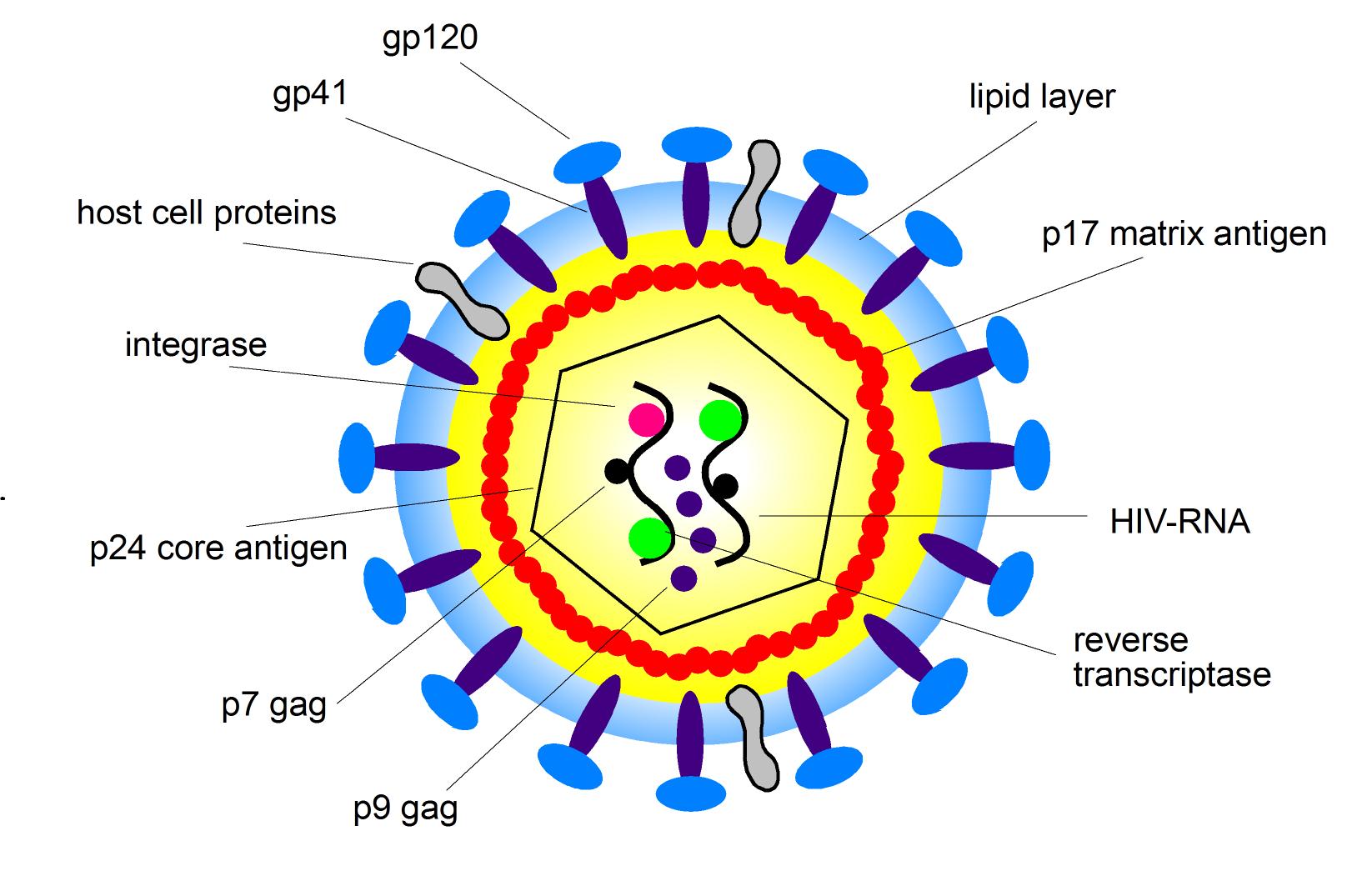
- Single-stranded RNA retrovirus (lentivirus)
- gp120: binds CD4 + CCR5/CXCR4 → entry
- gp41: fusion protein
- p24 capsid antigen: diagnostic marker
- Reverse transcriptase, integrase, protease: essential enzymes
🌀 Viral Life Cycle
- gp120 binds CD4 → chemokine receptor (CCR5/CXCR4)
- Fusion via gp41 and entry into cell
- Reverse transcription: RNA → DNA
- Integration into host genome via integrase
- Viral proteins synthesized by host machinery
- Virion assembly and release
🧬 Genes & Tropism
- gag = structural proteins; pol = enzymes; env = envelope (gp120, gp41)
- tat, rev = regulatory proteins; vif, vpr, vpu = accessory proteins
- Targets: CD4+ T cells, macrophages, dendritic cells → gradual CD4 depletion → immunodeficiency
📡 Transmission & Epidemiology
- Sexual contact (↑ risk with STIs) 💏
- Blood: needles, transfusions 💉
- Vertical: pregnancy, delivery, breastfeeding 🤱
- Worldwide burden highest in Sub-Saharan Africa 🌍
- Window period: 2–6 weeks → antibody-negative but highly infectious ⚠️
🔎 Clinical Clues to Test HIV
- Herpes zoster, recurrent infections
- Unexplained lymphadenopathy, fever
- Recurrent pneumonia, TB, lymphoma
⚠️ AIDS-Defining Conditions
- Infections: PCP, cryptococcosis, CMV, TB, MAC
- Cancers: Kaposi’s sarcoma, invasive cervical cancer, NHL
- Other: HIV encephalopathy, wasting syndrome
💊 ART & Prophylaxis
- Start ART for all patients, irrespective of CD4
- Suppress viral load, restore CD4, prevent transmission
- Prophylaxis:
- CD4 <200 → co-trimoxazole for PCP
- CD4 <100 → fluconazole for cryptococcus (high-risk)
- CD4 <50 → azithromycin/clarithromycin for MAC, regular fundoscopy for CMV
- Monitor: viral load, CD4, renal, liver, metabolic profile
- Vaccinations: inactivated vaccines; live vaccines avoided if CD4 <200
CD4 Count Thresholds & Opportunistic Infections 📊
| CD4 Count | Common Opportunistic Infections 🦠 | Prophylaxis / Notes 💊 |
|---|---|---|
| <500 | Oral candidiasis, shingles, Kaposi’s sarcoma | No routine prophylaxis; start ART |
| <200 | PCP, oesophageal candidiasis, cryptosporidium | Co-trimoxazole daily (stop once CD4 >200 on ART) |
| <100 | Toxoplasmosis, cryptococcal meningitis, disseminated Candida | Co-trimoxazole for toxoplasmosis; consider fluconazole prophylaxis |
| <50 | CMV retinitis/colitis, MAC, PML | Azithromycin weekly for MAC; regular fundoscopy for CMV monitoring |
📚 References
- NICE Guideline NG60: HIV testing and management
- BHIVA Guidelines
- Gazzard BG, HIV Medicine, 2018
- Panel on Opportunistic Infections in HIV-Infected Adults and Adolescents, CDC
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
