| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Granulomas
Related Subjects: | Chronic Granulomatous Disease | Granulomatous Diseases
🧩 Granulomatous diseases are conditions in which the immune system forms granulomas - organised clusters of macrophages, lymphocytes, and giant cells - as a defence mechanism when unable to eliminate a pathogen or trigger. ⚠️ Granulomas are a non-specific pathological pattern and must be interpreted in clinical context.
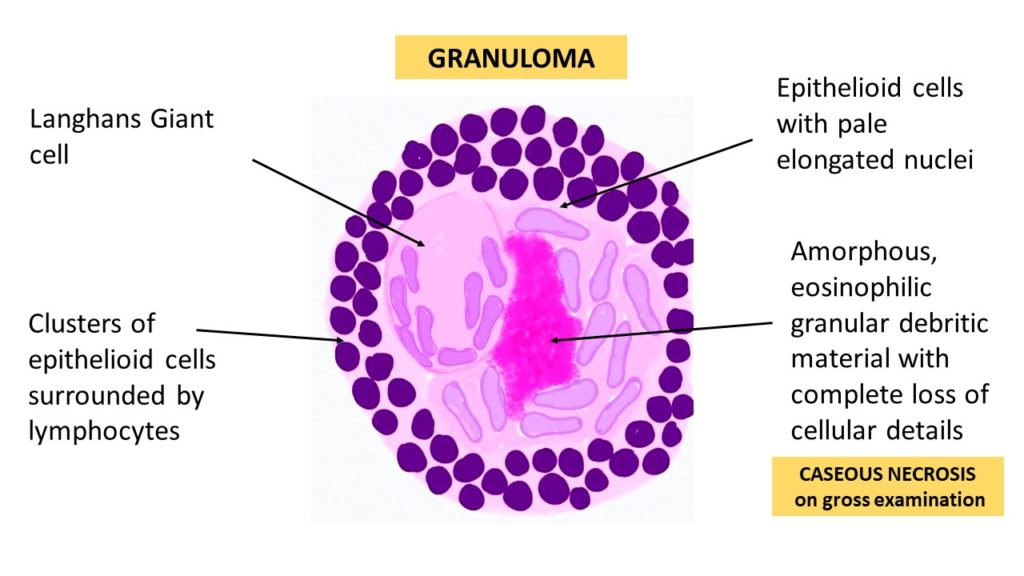
🔬 Characteristics of Granulomas
- Structure 🧱 :
- Aggregates of macrophages (epithelioid cells), lymphocytes, and multinucleated giant cells.
- Caseating granulomas (central necrosis, cheese-like appearance) → classic of TB & fungal infections.
- Non-caseating granulomas (no necrosis) → sarcoidosis, Crohn’s disease.
- Occasional calcification in chronic granulomas.
- Formation 🔄 :
- Triggered by persistent antigenic stimulus.
- Macrophages → epithelioid cells → multinucleated giant cells (Langhans type or foreign-body type).
- T-helper (CD4+) cells, TNF-α, and interferon-γ play central roles.
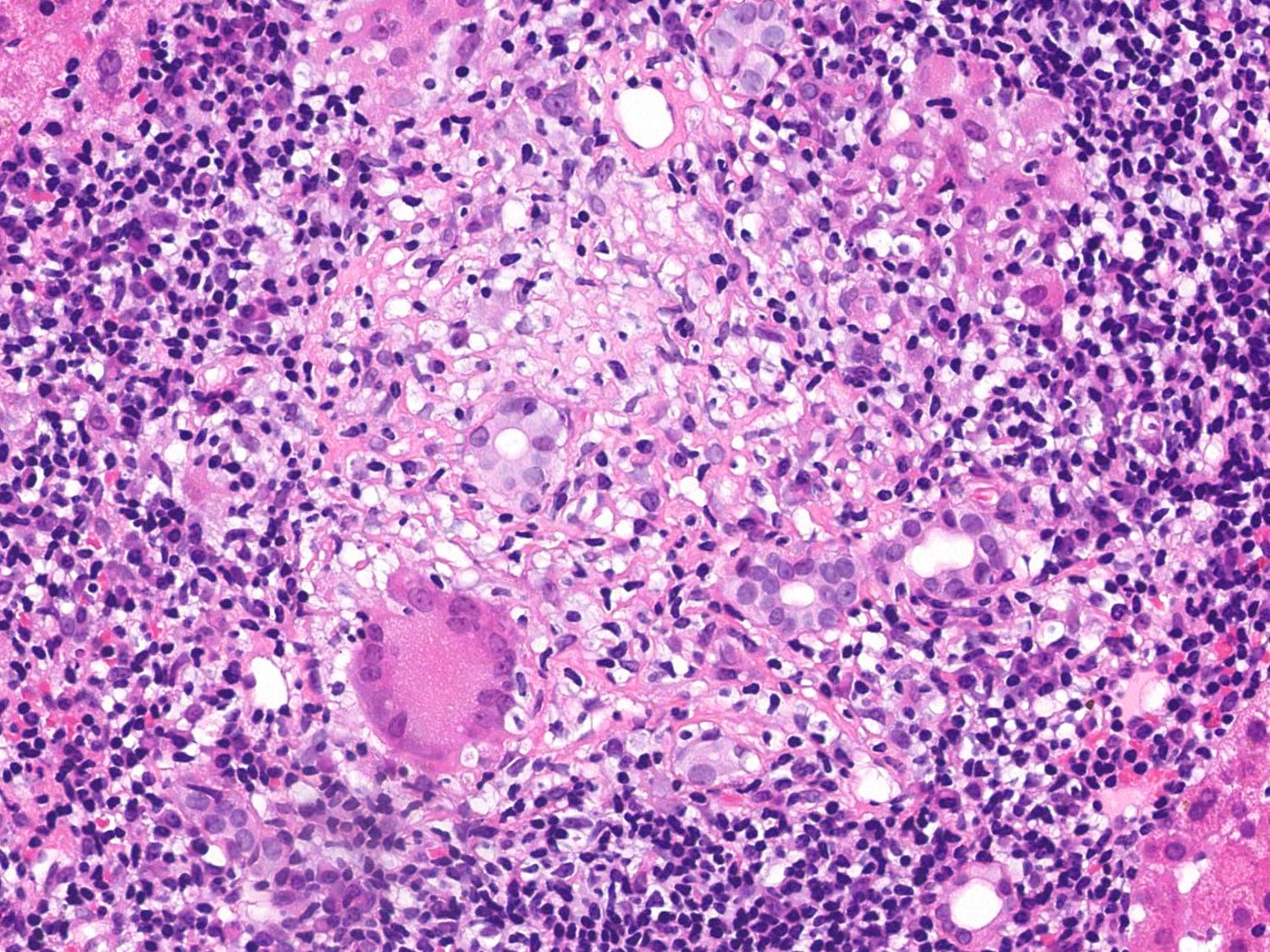
🧾 Common Granulomatous Diseases
- Tuberculosis 🫁 :
- Mycobacterium tuberculosis → caseating granulomas.
- Symptoms: chronic cough, fever, night sweats, weight loss.
- May cavitate and spread (miliary TB).
- Sarcoidosis 🌿 :
- Autoimmune → non-caseating granulomas.
- Affects lungs, lymph nodes, eyes, skin.
- Symptoms: cough, dyspnoea, erythema nodosum, uveitis.
- Granulomatosis with Polyangiitis (GPA) 🩸 :
- Necrotising vasculitis with granulomas.
- Affects ENT, lungs, kidneys.
- Symptoms: sinusitis, haematuria, cough, pulmonary nodules.
- Lab: c-ANCA (PR3 antibodies).
- Leprosy 🧕 :
- Mycobacterium leprae → granulomas in skin, nerves, airway.
- Symptoms: anaesthetic patches, neuropathy, deformities.
- Histoplasmosis 🍂 :
- Fungal → caseating granulomas in lung & lymph nodes.
- Can mimic TB; disseminates in immunocompromised hosts.
- Cryptococcosis 🍄 :
- Cryptococcus neoformans → lung + brain granulomas.
- Symptoms: cough, chest pain, meningitis in HIV.
- Cat-Scratch Disease 🐱 :
- Bartonella henselae → granulomatous lymphadenitis.
- Symptoms: fever, fatigue, tender lymph nodes after cat scratch/bite.
🔍 Diagnosis
- Clinical 🩺 : Symptoms vary by organ system.
- Imaging 🖼️ : CXR/CT (lung granulomas), MRI/CT (CNS involvement).
- Lab 🧪 :
- Blood tests (inflammatory markers, serology).
- Tuberculin skin test / interferon-gamma release assay (TB).
- ANCA (vasculitis), ACE level (sarcoidosis).
- Histology 🔬 : Biopsy shows granuloma type (caseating vs non-caseating).
💊 Treatment
- Infectious 🌡️ :
- TB → multi-drug therapy (RIPE regimen).
- Leprosy → rifampicin + dapsone ± clofazimine.
- Fungal infections → antifungals (Itraconazole, Amphotericin B).
- Autoimmune 🛡️ :
- Sarcoidosis/GPA → corticosteroids, methotrexate, azathioprine, biologics (rituximab for GPA).
- Supportive 🩹 :
- Pain control, oxygen therapy for lung disease, immunosuppression monitoring.
⚠️ Clinical Pearls
- Always distinguish infectious vs autoimmune → treatment differs radically (antibiotics vs immunosuppression).
- Caseating granulomas → usually TB/fungal. Non-caseating → sarcoid, Crohn’s, GPA.
- Some granulomas calcify → appear as incidental CXR/CT findings.
- Chronic granulomas can lead to fibrosis and organ dysfunction.
📚 Summary
Granulomatous diseases represent a spectrum of infectious 🦠, autoimmune 🌿, and inflammatory 🔥 conditions. Histology (caseating vs non-caseating), microbiology, and systemic context guide diagnosis. Treatment may involve antimicrobials, antifungals, corticosteroids, or immunosuppressants, tailored to the underlying cause.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
