| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Acute Cardiogenic Pulmonary Oedema (CPO/LVF) ❤️
Related Subjects: |Heart Failure with preserved and reduced EF |Heart Failure and Pulmonary Oedema |Loop Diuretics |Entresto Sacubitril with Valsartan |Ivabradine |Furosemide |Angiotensin Converting Enzyme Inhibitors |Cardiac Resynchronisation Therapy (CRT) Pacemaker
💔 Cardiogenic Pulmonary Oedema (CPO) is a medical emergency. Often triggered by STEMI, arrhythmia, or mechanical failure. Always exclude these early. A simple bedside echo is invaluable. Acute pulmonary oedema is usually driven by a sudden rise in left-sided filling pressures (LV failure/acute MR/MI, hypertensive crisis), forcing fluid across the alveolar-capillary membrane. Your early wins are: improve oxygenation/ventilation (CPAP), offload the lungs (diuresis), and reduce preload/afterload (vasodilators) while treating the trigger.
| 💔 Emergency Management: Cardiogenic Pulmonary Oedema (CPO) |
|---|
|
🪑 Position → Sit upright, comfort, legs dependent, reassure, may need catheter
🫁 Oxygen → Maintain sats >92% (88–92% if COPD); CPAP if hypoxic 💧 Diuretics → Furosemide 40–80 mg IV bolus often as 4mg/kg but may need more rapid if in extremis. Diuresis and venodilates 💉 Opiates → Morphine 2.5–5 mg IV slow + antiemetic 💊 Nitrates → GTN spray; IV infusion if SBP >110 mmHg 🫀 Arrhythmias/STEMI → Treat Fast AF (Digoxin, Amiodarone) /VT (Amiodarone or DC shock), urgent PCI if STEMI 🔌 Advanced Support → CPAP 5–10 cmH₂O/NIV, balloon pump, dialysis if needed, Papillary rupture / VSD → balloon pump + urgent surgery |
💡 Mnemonic: sit up and FONAM = Furosemide, Oxygen Nitrates Arrhythmia Morphine,
📖 About
- CPO = acute left ventricular dysfunction → pulmonary venous hypertension → alveolar flooding.
- Rapidly leads to respiratory failure ± cardiogenic shock.
- 30-day mortality ~15% if NT-proBNP >5000 ng/L.
- LV systolic function strongly influences prognosis.
⚖️ Pathophysiology
- Normally: Plasma oncotic pressure (~25 mmHg) holds water in; Pulmonary capillary pressure (~7–12 mmHg) pushes fluid out.
- If PCP > POP → alveolar oedema → hypoxia, ↑ work of breathing.
🔎 Aetiology
- Poor systolic function (e.g. MI).
- Poor diastolic function (HFpEF).
- Valve lesions (MR, AR, AS).
- Arrhythmias (AF, VT, bradycardia).
- Hypertension, myocarditis, cardiomyopathy.
- Fluid overload (blood transfusion, renal failure).
❓ Precipitating Causes
| Cause | Clues | Diagnostics |
|---|---|---|
| MI | Chest pain, diaphoresis | ECG, troponin, echo |
| AF | Palpitations, irregular pulse | ECG, echo |
| HTN | Headache, chest pain | BP, LVH on echo |
| Valvular disease | Murmur, dyspnoea | Echo, Doppler |
| PE | Pleuritic pain, haemoptysis | CTPA, D-dimer |
| Sepsis | Fever, hypotension | Blood cultures, lactate |
| Drug/alcohol | Recent change | Medication review |
📊 Clinical: Left vs Right HF
The patient may be grey cold clammy and dramatically breathless and struggling to breath with a tachycardia and S3 and possibly murmurs, there is a raised JVP and lungs have fine inspiratory crackles. The sats may be low. Urgent management is needed.
- Left-sided: Tachypnoea, Tachycardia, S3, Murmurs, Orthopnoea, PND, bibasal creps, “bat-wing” CXR.
- Right-sided: Raised JVP, hepatomegaly, ascites, oedema.
- Often coexist → congestive HF.
🧪 Investigations (Acute Cardiogenic Pulmonary Oedema)
- Bedside (immediate):
- Vitals + monitoring: RR, BP, HR, temperature, continuous SpO2 + ECG monitoring.
- ECG (12-lead): look for ACS (ST/T changes), arrhythmia (AF, VT), LVH/strain, conduction disease.
- ABG/VBG: pO2/pCO2, pH, HCO3−; identify hypercapnia/tiring (important for NIV/ITU decisions).
- Lactate: marker of hypoperfusion/shock and severity.
- Glucose: especially if diabetic/altered mental state.
- Urine output: catheter if severe illness; helps gauge diuretic response and perfusion.
- Bloods:
- FBC: anaemia (reduces oxygen delivery), leukocytosis (infection trigger).
- U&E/creatinine: baseline renal function, K+/Na+ before diuresis/ACEi; guides dosing and safety.
- LFTs: hepatic congestion or hypoperfusion (“shock liver”).
- Troponin: MI/ischemia trigger (interpret in context; may be type 2 rise in severe HF).
- NT-proBNP: supports HF diagnosis if uncertain (less helpful if obvious clinically or known HF).
- CRP: if infection suspected; blood cultures before antibiotics if septic.
- TFTs: not urgent in resus, but useful if AF/new HF or unexplained decompensation.
- Mg/Ca/phosphate: if arrhythmia or on diuretics (electrolytes drive ectopy and rate control success).
- Imaging:
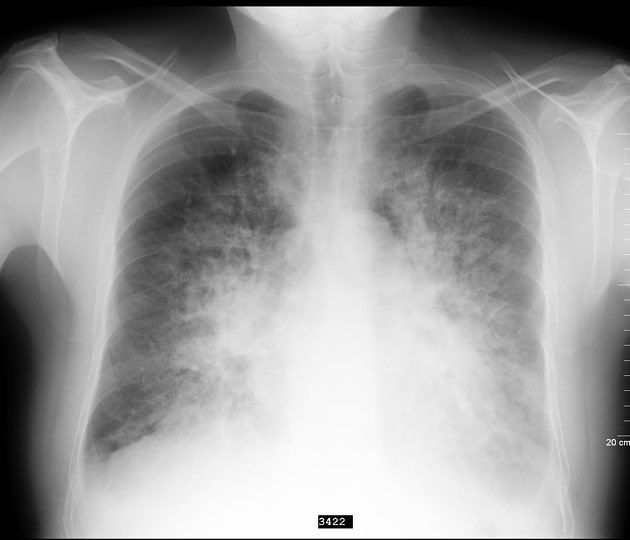
- CXR: cardiomegaly, upper lobe diversion, interstitial oedema (Kerley B lines), perihilar “bat-wing” shadowing, pleural effusions; also exclude pneumonia/pneumothorax.
- Point-of-care ultrasound (if available): lung B-lines, pleural effusions, IVC size; rapid bedside support for congestion.
- Echocardiography (urgent if severe/unclear): LV/RV function, regional wall motion (ischaemia), valve lesions (acute MR/AS), pericardial effusion/tamponade, pulmonary pressures.
- Advanced / specialist tests (selected cases, not acute resus):
- CT pulmonary angiography: if PE is a realistic alternative/trigger (especially if disproportionate hypoxia, RV strain).
- Coronary angiography: if STEMI/NSTEMI or ongoing ischaemia driving ACPO (cardiology pathway).
- Cardiac MRI: myocarditis/infiltrative disease/scar assessment once stabilised.
- Nuclear imaging (SPECT/PET): viability/ischaemia assessment in chronic planning rather than acute management.
⚡ Complications
- Respiratory failure:
- Type 1 (hypoxaemic): alveolar flooding + V/Q mismatch → low pO2.
- Progression to Type 2 (hypercapnic): fatigue, reduced minute ventilation, worsening alveolar ventilation (red flag for NIV failure/ITU).
- Cardiac complications:
- Arrhythmias: AF with fast rate (worsens filling), VT/VF, bradyarrhythmias; risk of sudden cardiac death.
- Myocardial ischaemia/infarction: ACPO can be both a cause and consequence of ACS (type 1 vs demand-mediated injury).
- Cardiogenic shock: “cold + wet” phenotype with hypoperfusion, rising lactate, oliguria.
- Renal dysfunction:
- AKI / cardiorenal syndrome: low forward flow + venous congestion + diuretics/ACEi exposure → creatinine rise and diuretic resistance.
- Hepatic and splanchnic congestion:
- Congestive hepatopathy: cholestatic LFT pattern; can progress to marked transaminitis if hypoperfusion (“shock liver”).
- Gut oedema: impaired drug absorption (e.g., oral diuretics) and malnutrition.
- Electrolyte and acid–base problems:
- Hyponatraemia: dilutional (ADH-driven) and a marker of severe HF; worsens confusion/falls risk.
- Hypokalaemia / hypomagnesaemia: diuretics → ectopy/VT risk and digoxin toxicity risk.
- Hyperkalaemia: renal impairment + RAAS blockade; conduction disturbance risk.
- Metabolic alkalosis: aggressive diuresis; may worsen CO2 retention in vulnerable patients.
- Thromboembolism:
- VTE: immobility, inflammation and haemoconcentration; consider prophylaxis if safe.
- Stroke/systemic embolism: especially if AF or severe LV dysfunction with thrombus.
- Functional decline and vulnerability:
- Delirium: hypoxia, infection, metabolic disturbance, opioids.
- Frailty, sarcopenia/cachexia: chronic catabolism + inflammation; strongly predicts readmission and mortality.
- Pressure injury/falls: immobility, hypotension, polypharmacy.
💊 Management
- Call for help + monitor: Sit upright, continuous ECG, BP, SpO2, RR; IV access; strict fluid balance + urine output (catheter if very unwell).
- Immediate investigations: ABG/VBG (± lactate), U&E/creatinine, FBC, troponin, glucose; CXR; ECG; bedside echo if available (LV function, MR, tamponade, RV strain).
- Oxygen strategy:
- Give O2 only if hypoxic. Aim SpO2 94–98% (or 88–92% if known CO2 retention).
- Early CPAP/NIV if severe distress/hypoxia despite O2 (often rapidly reduces work of breathing and improves gas exchange).
- Escalate to CCU/ICU/anaesthetics early if tiring, reduced consciousness, or NIV failing.
- Diuretics (decongestion):
- IV loop diuretic (e.g., furosemide 40 mg, 50 mg or 80 mg are all fine as needed or bumetanide 1-2 mg).
- Use higher doses if already on regular diuretics.
- Reassess response (symptoms, RR, crackles, urine output) and check renal function/electrolytes; consider infusion if poor response.
- Vasodilators (reduce preload/afterload):
- If SBP ≥ 110 mmHg and ongoing distress, consider GTN (sublingual or IV infusion) to rapidly reduce pulmonary capillary pressure.
- Avoid if hypotensive, severe aortic stenosis, or suspected RV infarct.
- Analgesia/anxiolysis:
- Avoid routine morphine; if used, do so cautiously (risk of respiratory depression/hypotension) and treat nausea.
- If shock/poor perfusion (cold + wet):
- Urgent senior/ICU input; consider inotropes/vasopressors (e.g., dobutamine ± noradrenaline) guided by echo/BP/perfusion.
- Look hard for reversible causes: MI, acute MR, arrhythmia, tamponade, massive PE.
- Treat the trigger (do not miss):
- ACS/MI: follow local ACS pathway; early cardiology review and reperfusion if indicated.
- Hypertensive ACPO: nitrates + CPAP are often key.
- Arrhythmia (AF with fast rate, VT): rate/rhythm control; urgent DC cardioversion if unstable.
- Acute valvular disease (e.g., acute MR): urgent echo + cardiothoracic/cardiology input.
- Fluid overload/renal failure: consider ultrafiltration/dialysis discussion if diuretic-resistant.
- When improving (transition to chronic HF care):
- Start/optimise disease-modifying therapy once stable: ACEi/ARB/ARNI, beta-blocker, MRA, and consider SGLT2 inhibitor where appropriate (per local/NICE guidance).
- Plan follow-up, education (daily weights, salt/fluids), and review precipitant + adherence.
- Advanced/definitive options (selected patients): CRT, ICD, LVAD, transplant (specialist pathways).
✅ Quick practical timing prompts
- 0–10 minutes: Sit up, monitoring, ABG/VBG, CPAP/NIV early if needed; if SBP ≥110, start GTN (SL then IV).
- 10–60 minutes: IV loop diuretic if congested; reassess BP/respiratory effort every 5–15 min; ECG/CXR; start ACS/arrhythmia pathway if indicated.
- 1–6 hours: Review urine output, repeat gases if severe, check U&E/K/Mg; consider escalation (infusions, inotropes, ICU) or specialist add-ons (metolazone/ultrafiltration) if resistant.
💊 Drug Table
| Drug | When to use | Typical dose | Timing / titration | Key cautions |
|---|---|---|---|---|
| GTN (glyceryl trinitrate) – sublingual spray/tablet | Severe dyspnoea with SBP ≥110 mmHg, especially hypertensive ACPO, while preparing IV infusion | 400 micrograms (1 spray) SL | Repeat every 5 minutes as needed while monitoring BP (commonly up to 3 doses) | Avoid/very cautious in hypotension, severe aortic stenosis, suspected RV infarct, recent PDE5 inhibitors |
| GTN – IV infusion | Ongoing distress despite oxygen/NIV, hypertensive pulmonary oedema | Start 5–10 micrograms/min | Increase by 5–10 micrograms/min every 3–5 min to symptom relief/BP target (often 20–200 micrograms/min; higher in monitored/ICU settings) | Continuous BP monitoring; stop/reduce if SBP falls or headache/hypotension develops |
| Furosemide – IV bolus | Clinical fluid overload, raised JVP/oedema, or known HF with congestion | 40 mg IV (if diuretic-naïve). If already on loop diuretic: same as or up to 2× their usual total daily oral dose as IV equivalent (senior-led) | Assess urine output and symptoms at 30–60 min. Consider repeat dosing if inadequate response | Can worsen hypotension/AKI; check U&E, watch K/Mg; avoid “diuretic-first” if profoundly hypertensive distress where nitrates/NIV are the rapid wins |
| Bumetanide – IV bolus | Alternative loop diuretic (e.g., poor response to furosemide, significant gut oedema, or local preference) | 1 mg IV (roughly ≈ furosemide 40 mg) | Reassess at 30–60 min; repeat/step up guided by response | Same cautions as loop diuretics; electrolyte depletion |
| Loop diuretic infusion (e.g., furosemide) | Diuretic resistance or repeated boluses needed; ICU/CCU-style pathway | Common approach: loading bolus then 5–10 mg/hour (ranges vary) | Titrate every 1–2 hours to urine output/clinical congestion; close U&E monitoring | Requires careful monitoring; risk of AKI, ototoxicity at very high doses/rapid pushes; senior-led |
| Morphine – IV (NOT routine) | Only if severe distress/pain/anxiety persists despite NIV and haemodynamic stabilisation, and senior agrees | 1–2 mg IV slow, small aliquots | Reassess after 5–10 min; repeat cautiously if needed | Respiratory depression, hypotension, nausea/vomiting; avoid if drowsy/CO2 retaining/hypotensive |
| Antiemetic (e.g., ondansetron) | If opioid used or significant nausea/vomiting | 4 mg IV | Single dose; reassess | QT prolongation risk (check ECG if concerns) |
| Dobutamine – IV infusion | Cold + wet (hypoperfusion/shock) with low cardiac output, typically ICU/CCU after echo/senior review | Start 2.5 micrograms/kg/min | Titrate every 10–20 min (typical range 2.5–20 micrograms/kg/min) to perfusion/BP/urine output | Arrhythmias, tachycardia, myocardial ischaemia; needs monitoring and clear diagnosis |
| Noradrenaline (norepinephrine) – IV infusion | Hypotension/shock to maintain perfusion pressure (often alongside inotrope), ICU pathway | Common starting range 0.05 micrograms/kg/min (local protocols vary) | Titrate every 2–5 min to MAP/BP target | Extravasation risk; ideally central access; treat the cause (MI, MR, tamponade etc.) |
| Nitroprusside – IV infusion (specialist) | Refractory hypertensive ACPO with severe afterload problem (ICU/CCU only) | Start 0.3 micrograms/kg/min | Titrate every 3–5 min (typical max ~10 micrograms/kg/min short term) | Cyanide/thiocyanate toxicity risk, hypotension; requires invasive monitoring |
| ACE inhibitor (e.g., captopril – oral) (selected cases) | After initial stabilisation, persistent hypertension with HF once not in shock and no contraindications | 6.25 mg PO | Can repeat/uptitrate cautiously after 30–60 min with BP monitoring (senior-led) | Avoid in hypotension, AKI, hyperkalaemia, bilateral RAS, pregnancy; not a “first 10 minutes” drug |
⚡ Additional interventions
| Trigger / scenario | Drug(s) | Typical dose | Timing / titration | Key cautions / notes |
|---|---|---|---|---|
| Suspected ACS / MI | Aspirin | 300 mg PO (chewed) if not already taken | Give immediately once ACS suspected (per ACS pathway) | Contra: true aspirin allergy, active major bleeding |
| Suspected ACS / MI | P2Y12 inhibitor (specialist pathway) | Common UK practice: Ticagrelor 180 mg PO loading or Clopidogrel 300–600 mg PO loading (varies by STEMI/NSTEMI pathway) | As per local cardiology/PCI pathway (often after ECG confirmation and discussion) | Bleeding risk; avoid if urgent surgery likely; follow trust protocol |
| Suspected ACS / ongoing ischaemic pain | GTN (as per core table) | SL 400 micrograms q5 min PRN; IV start 5–10 micrograms/min | Titrate every 3–5 min to pain relief/BP | Avoid in hypotension, severe AS, RV infarct, recent PDE5 inhibitors |
| AF with fast ventricular response (haemodynamically stable) | Digoxin (rate control in HF) | 500 micrograms IV (or PO) then 250 micrograms at 6 hours and again at 12 hours (max 1.0–1.5 mg in 24 h depending on age/renal function) | Slower onset; reassess rate and symptoms over hours | Reduce dose in elderly/renal impairment; toxicity risk (arrhythmias, GI, confusion); check K/Mg |
| AF with fast rate (stable, BP ok) | Amiodarone (rhythm control / rate control alternative) | 300 mg IV over 20–60 min, then infusion 900 mg over 24 h | Use when appropriate (often senior-led/cardiology) | Hypotension/bradycardia; interacts with warfarin/digoxin; needs ECG monitoring |
| Unstable tachyarrhythmia (AF/VT with hypotension, ischaemia, pulmonary oedema) | DC cardioversion | Energy per ALS protocol (biphasic escalating) | Immediate | Not a drug, but the correct “dose” is electricity; involve resus/anaesthetics |
| VT / Electrical storm (with ACPO) | Amiodarone | 300 mg IV over 20–60 min (can repeat per ALS), then 900 mg/24 h | Early, alongside correction of K/Mg and ischaemia treatment | Consider magnesium; urgent cardiology/ICU for recurrent VT/VF |
| Torsades / hypomagnesaemia | Magnesium sulfate | 2 g IV (8 mmol) over 10–15 min | May repeat once if needed; then consider infusion per protocol | Monitor reflexes/respiration in renal failure; correct K as well |
| Hypertensive emergency driving ACPO | GTN IV (first-line add-on) | Start 5–10 micrograms/min, titrate rapidly | Increase every 3–5 min to symptom/BP response | Often the “fastest fix” with CPAP; avoid if severe AS/RV infarct/hypotension |
| Acute severe mitral regurgitation (papillary muscle dysfunction/rupture, endocarditis etc.) | Vasodilator (GTN) ± inotrope (dobutamine) | GTN as above; dobutamine start 2.5 micrograms/kg/min | Titrate GTN every 3–5 min; dobutamine every 10–20 min | Needs urgent echo + cardiology/cardiothoracic; may require mechanical support/urgent surgery |
| Suspected sepsis/pneumonia precipitant | Antibiotics (per local guideline) | Depends on source and severity | Give within 1 hour if sepsis suspected | Fluid resuscitation must be cautious in ACPO—senior review; use vasopressors if shock rather than large fluids |
| Thromboembolism risk / immobility | VTE prophylaxis (if no contraindication) | Example: Enoxaparin 40 mg SC OD (adjust for renal function/weight) | Once stable and bleeding risk assessed | Follow local VTE policy; avoid if active bleeding/very high risk |
| Fluid overload + renal failure / diuretic resistance | Metolazone (specialist add-on) | 2.5 mg PO | Often single dose, reassess over 6–12 h; may repeat cautiously (senior-led) | Profound diuresis/hypoNa/hypoK; close U&E monitoring; usually HF specialist decision |
| Persistent congestion despite loops | Chlorothiazide IV (less common UK) / thiazide-type add-on | Varies by local availability | Specialist/ICU pathway | Electrolyte depletion; monitor Na/K/Mg closely |
| After stabilisation: start disease-modifying HF therapy | ACEi/ARB/ARNI; beta-blocker; MRA; SGLT2 inhibitor | Start low (agent-specific) once euvolaemic and BP/renal function acceptable | Usually on the ward once off IV nitrates/inotropes and not in AKI | Not “resus drugs”; avoid initiating/up-titrating beta-blocker during acute decompensation/shock |
📉 Prognosis
- HF prognosis worse than many cancers.
- EF <35% = poor marker.
- NT-proBNP correlates with survival.
- Consider palliative care in end-stage disease.
📚 References
Cases - Acute Heart Failure & Pulmonary Oedema
- Case 1 - Hypertensive Emergency 💥: A 72-year-old man with untreated hypertension presents acutely breathless at night, unable to lie flat. Exam: BP 210/110, tachypnoea, widespread crackles, S3 gallop. CXR: bilateral perihilar “bat-wing” shadowing. Diagnosis: Acute pulmonary oedema triggered by hypertensive crisis. Acute Management: Sit upright, oxygen, IV furosemide, IV GTN infusion, morphine if distressed, strict BP control. Monitor U&Es and fluid balance.
- Case 2 - Acute MI Complication ❤️: A 64-year-old man presents with acute chest pain followed by severe dyspnoea. Exam: hypotension, crackles to mid-zones, raised JVP, cool peripheries. ECG: anterior STEMI. Echo: severe LV systolic dysfunction. Diagnosis: Acute cardiogenic pulmonary oedema secondary to MI. Acute Management: Sit upright, O₂, IV diuretics, cautious opioids; urgent PCI for MI; inotropes or mechanical support (IABP) if shock persists.
- Case 3 - Acute Decompensation in Chronic HF 🌀: A 78-year-old woman with known HFrEF (EF 30%) presents with sudden worsening breathlessness after a chest infection. Exam: tachypnoeic, bibasal crackles, elevated JVP, peripheral oedema. BNP elevated, CXR: pulmonary congestion. Diagnosis: Acute decompensated heart failure with pulmonary oedema, triggered by infection. Acute Management: Sit upright, O₂, IV furosemide; treat infection (antibiotics); optimise chronic therapy (ACEi, beta-blocker, spironolactone) once stable.
Teaching Commentary 🧠
Acute heart failure with pulmonary oedema is a medical emergency. - Pathophysiology: raised LV end-diastolic pressure → pulmonary venous congestion → alveolar fluid → hypoxia. - Precipitants: MI, arrhythmias, hypertensive crisis, infection, fluid overload, non-compliance. - Clinical: severe breathlessness, orthopnoea, crackles, frothy pink sputum, gallop rhythm. - Acute management (“PODMAN”): Position upright, Oxygen, Diuretics (IV loop), Morphine, Afterload reduction (nitrates), Non-invasive ventilation if hypoxic. Long-term: optimise HF therapy (ACEi/ARNI, beta-blockers, MRA, SGLT2 inhibitors); lifestyle and fluid restriction; device therapy (CRT, ICD) in select patients.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
